A missing tooth rarely feels like a small problem. You notice it when you chew on one side, when food catches in the gap, and often when you smile in photos or speak with confidence you used to take for granted.
For many people in Dulwich Hill and the Inner West, the next question is not just whether an implant can replace the tooth. It is whether the result will still be working well years from now. That is the right question to ask, because a dental implant is not a short-term patch. It is a long-term treatment, and it deserves a clear, honest answer.
Your Guide to the Lifespan of Dental Implants
A patient might sit down for a consultation after putting off the decision for months. They may have managed around the gap, chewed more carefully, and told themselves it was not urgent. Then a bridge, denture, or implant enters the conversation, and one concern rises above the rest. If I do this, how long will it last?
That concern is sensible. An implant involves surgery, healing, time, and cost. No one wants vague reassurance. People want to know what is likely, what can go wrong, and what they can do to help the treatment succeed.
The practical answer is this. Dental implants can last for a very long time, and in many cases the implant fixture has the potential to remain in place for life. But that outcome depends on several moving parts. The quality of the bone matters. The placement matters. The design of the restoration matters. Home care matters. Smoking matters. Regular review matters.
It also helps to separate what patients often group together as “the implant”. There is the part in the bone, and there is the tooth you see above the gumline. They do not always age in the same way, and understanding that distinction makes the whole topic much clearer.
Dr. Dimitrios Thanos has worked in implant dentistry since 1996, and one of the most useful conversations any dentist can have with a patient is a realistic one. Not pessimistic. Not overly optimistic. Realistic. That means explaining that longevity is possible, but not automatic. Good dentistry and good habits work together.
How Long Do Dental Implants Really Last?
The simplest way to understand implant lifespan is to think of a house.
The implant fixture is the foundation. It sits below the surface, anchored in bone, and if it integrates well it is built to stay. The crown is the visible structure above it. It looks like the tooth, does the day-to-day work, and naturally takes the wear from chewing, grinding, and years of use.
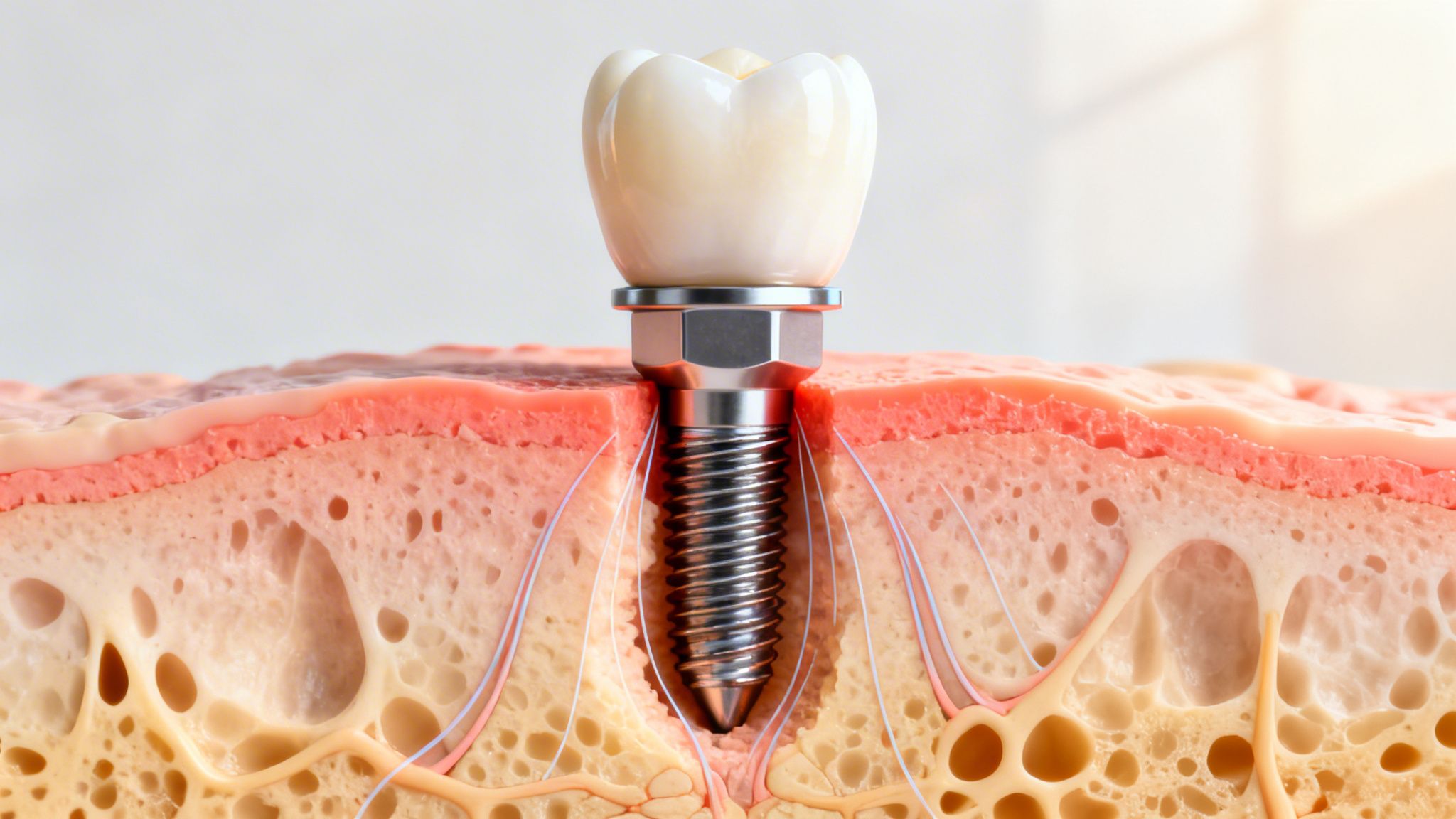
The part in the bone lasts longer than the part you chew on
This distinction matters because patients often hear one number and assume it applies to everything. It does not.
The titanium fixture is designed for long-term retention through osseointegration, which means the bone heals around the implant and holds it in place. Australian data reflects strong long-term outcomes, with 96.4% survival at 10 years and approximately 80% survival at 20 years, while non-smokers with good oral hygiene show 90 to 95% success over 10 years according to Australian implant survival data summarised here.
That is why dentists often say the implant itself may last a lifetime. We are usually talking about the fixture in the jawbone.
The crown is different. It faces constant force. Every coffee, sandwich, late dinner, clenched jaw during traffic, and accidental crunch on a seed or olive pit adds up over time. The crown may eventually need repair or replacement even when the implant underneath remains healthy.
Key takeaway: When people ask how long do dental implants last, the most accurate answer is often “the implant fixture and the crown have different lifespans”.
What survival rate means in plain English
A survival rate is not the same thing as saying an implant looks brand new decades later. In clinical terms, survival usually means the implant remains in place and functional. It can still be supporting a crown successfully even if some maintenance has been needed along the way.
That is not unusual in dentistry. Natural teeth need maintenance too. Fillings are replaced. Crowns are renewed. Bite guards are made when grinding becomes a problem. Longevity in the mouth is usually about ongoing stewardship, not untouched perfection.
A good comparison is cosmetic dentistry. If you have ever looked into veneers, you already know that the visible restoration has its own lifespan and maintenance cycle. The same principle applies to implant crowns. If that topic interests you, this guide on how long porcelain veneers last offers a useful parallel in how restorative materials age under daily function.
What should you expect in real life
A realistic expectation looks like this:
- The fixture may stay stable for decades if it integrates well and the surrounding gum and bone remain healthy.
- The crown may need replacement later because wear and tear affect the chewing surface and margins over time.
- Maintenance is part of success, not a sign of failure.
- The better the planning and aftercare, the better the odds that the implant remains a long-term solution.
People often find this reassuring once it is explained properly. It replaces the all-or-nothing idea with a more accurate one. An implant is not fragile, but it is also not self-maintaining. It is a durable treatment that rewards careful placement and consistent care.
What Determines Your Dental Implant's Success?
Some implants fail early. Some remain stable for many years. The difference usually comes down to a handful of practical factors, and most of them are not mysterious.
A healthy implant needs clean conditions around the gumline, enough bone support, a manageable bite, and a patient who treats maintenance as part of the treatment rather than an optional extra.
Oral hygiene decides what happens around the implant collar
Implants do not get decay, but the tissues around them can still become inflamed. That is the beginning of trouble.
If plaque sits around the implant for long periods, the gum can become sore and bleed. If inflammation continues and the bone starts to recede, the situation becomes more serious. Patients often assume a titanium implant is immune to the problems that affect natural teeth. It is not. The risk is different, but the need for cleaning is just as real.
At home, the basics still matter:
- Brush carefully around the gumline with a soft toothbrush.
- Clean between teeth and around the implant using floss, interdental brushes, or a water flosser if that suits your dexterity better.
- Report bleeding early rather than waiting to see if it settles by itself.
- Protect the bite if you clench or grind.
A common mistake is brushing the crown well while neglecting the narrow area where the gum meets the implant restoration. That margin is where many problems begin.
Smoking is one of the clearest risks
Smoking affects healing, blood supply, and the tissue environment around implants. It is one of the strongest predictors of trouble that dentists discuss before treatment.
Australian data indicates that smokers have 2.4 times higher odds of dental implant failure, and a source cited for the Inner West suggests around 25% of adults smoke locally, which makes this especially relevant in everyday practice. The same source notes that smoking can reduce implant lifespan from 20+ years to under 10 without proper management and cessation support, as described in this discussion of smoking and implant longevity in the Dulwich Hill context.
Those numbers should not be used to frighten patients. They should be used to guide decisions. If you smoke, the conversation should be more detailed. The treatment plan may still be appropriate, but it must be planned with open eyes.
Practical advice: If you are considering implants and you smoke, the best time to address that habit is before surgery, not after complications appear.
Bone quality and general health still matter
Implants depend on bone. If the bone is thin, soft, or has already shrunk after tooth loss, planning becomes more important.
The same applies to general health. Diabetes, for example, can complicate healing and bone response. Bruxism can overload a new crown. A history of gum disease may call for closer maintenance. None of these automatically rule out treatment, but they change how a careful dentist approaches it.
A sound implant assessment does not just ask, “Can we place an implant here?” It also asks:
| Clinical question | Why it matters |
|---|---|
| Is there enough bone volume? | The implant needs stable support from the beginning. |
| Are the gums healthy now? | Existing inflammation increases risk around a future implant. |
| Is the bite balanced? | Heavy force can overload the implant crown or surrounding bone. |
| Does the patient grind or clench? | Mechanical stress shortens the life of restorations. |
| Are there medical factors affecting healing? | Healing quality influences integration and long-term stability. |
Technique and technology make a difference
A well-planned implant is not placed by guesswork. Position, angulation, depth, and restorative design all affect how cleanable and durable the final result will be.
Experience matters here. So does using tools that allow precise, minimally invasive treatment where appropriate. In practices that use Biolase laser dentistry, soft tissue management can often be gentler and more controlled. That matters for patient comfort, healing, and access around the implant site. For anxious patients, sedation can also make it easier to complete treatment calmly and predictably.
This short video gives a helpful visual overview of what patients often want to understand before treatment:
Success is shared between dentist and patient
The strongest implant treatment plans are partnerships.
The dentist controls diagnosis, planning, placement, and restoration design. The patient controls cleaning, smoking, attendance, and whether small warning signs are ignored or checked early. Problems usually develop when one side of that partnership breaks down.
That is why long-lasting implants tend to belong to patients who do ordinary things consistently. They keep review appointments. They replace a worn night guard. They clean around the restoration properly. They come in when something feels different.
Do All-on-4 Implants Last as Long as Single Implants?
A single implant replaces one missing tooth. All-on-4 uses a small number of implants to support a full-arch prosthesis when many or all teeth in one jaw need to be replaced.
That difference changes the mechanics. A single implant supports one crown. An All-on-4 case supports a larger bridge that spreads force across the arch. The biology of osseointegration is the same, but the restoration above the implants has a bigger job.
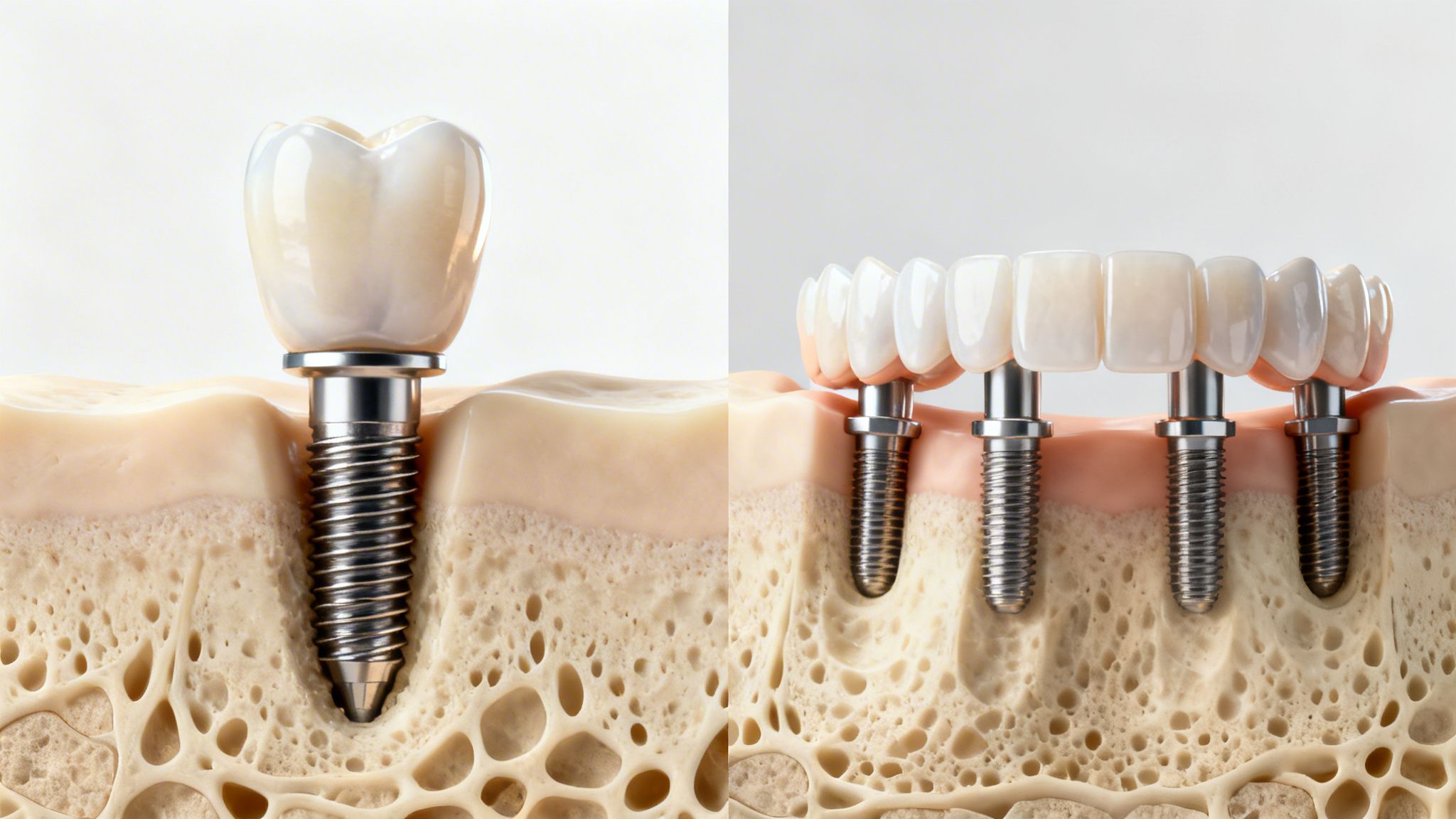
The implants can be durable in both systems
Australian clinics report a 92% 10-year success rate for All-on-4, and the same source notes that crowns on single implants can last 15 to 25 years, while long-term studies show over 90% of implants placed decades ago remain functional with excellent hygiene. That summary appears in this article on implant longevity and All-on-4 outcomes.
That tells us something important. All-on-4 is not a lesser version of implant treatment. It is a different design used for a different problem.
Where the trade-offs show up
The main differences are usually practical, not theoretical.
A single implant crown is easier to visualise because it behaves like one replacement tooth. If it chips, loosens, or wears, the issue is localised. An All-on-4 bridge carries the chewing load of a whole arch, so maintenance can be more involved. Hygiene under the bridge also requires more commitment and the right tools.
Patients considering full-arch treatment should think about three things:
- Cleaning access
A full-arch prosthesis has areas underneath that need deliberate cleaning every day. - Bite forces
The bridge takes broad chewing loads, so bite design and follow-up matter. - Maintenance mindset
The implants may remain stable while the prosthesis needs servicing, adjustment, or renewal over time.
Helpful comparison: Single implants replace a tooth. All-on-4 replaces a system. The more teeth a prosthesis is doing the work for, the more maintenance planning matters.
Which option lasts longer
That is not always the right question. The better question is which option best fits the condition of your mouth.
If one tooth is missing and the surrounding teeth are healthy, a single implant is often the most conservative choice. If many teeth are failing, or the remaining dentition cannot be predictably saved, All-on-4 may offer a more stable and functional long-term result than trying to maintain multiple compromised teeth.
Patients weighing that decision often also want to understand the broader planning and financial side. This guide on All-on-4 dental implants cost in Australia helps place the treatment in context.
Comparing Lifespans Implants Bridges and Dentures
Choosing between implants, bridges, and dentures is not just about replacing a gap. It is about deciding how much structure you want to preserve, how much maintenance you can commit to, and how you want the mouth to function over time.
The lifespan conversation becomes more useful when the options sit side by side.
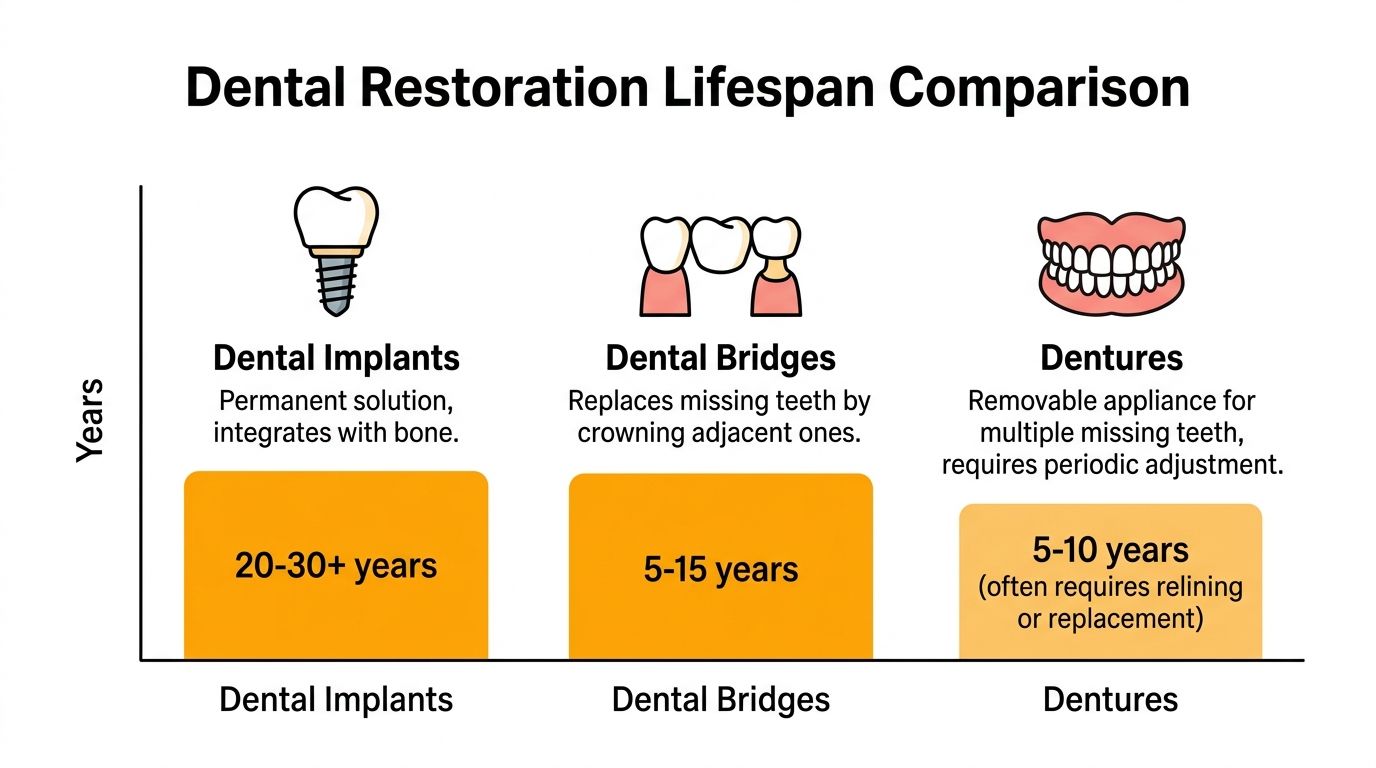
The key difference is what gets replaced when something wears out
With implants, the fixture in the bone and the restoration above it are separate components. That matters. A crown may wear and need replacement, while the implant fixture remains stable.
That is very different from traditional alternatives. A source discussing implant lifespan notes that the prosthetic crown typically requires replacement every 10 to 15 years due to wear, while the implant fixture has potential lifetime durability. It also points out that with bridges or dentures, failure often means replacing the entire structure, and bridges may involve adjacent healthy teeth. That distinction is explained in this article on the lifespan of implant components versus other restorations.
Side-by-side comparison
| Option | Typical longevity | What it relies on | What happens over time | Main trade-off |
|---|---|---|---|---|
| Dental implant | Long-term fixture potential, with crown replacement expected as it wears | Bone integration and healthy gums | The crown may be renewed while the implant remains in place | Higher treatment complexity at the start |
| Bridge | Often a medium-term solution | Support from adjacent teeth | Wear, leakage, or trouble in a supporting tooth can affect the whole bridge | Requires preparation of neighbouring teeth |
| Denture | Often needs relining, adjustment, or replacement sooner | Fit against gums and underlying ridge | The fit can change as the jawbone changes shape | Less stability and chewing confidence for many patients |
Why implants often offer better long-term value
Patients do not live with a restoration on paper. They live with it at work, over meals, while travelling, and through ordinary years of use.
That is where implants often stand out:
- They preserve oral structure better because they do not rely on cutting down adjacent healthy teeth.
- They feel more secure in function because they are anchored rather than resting on gum tissue.
- They separate the long-term foundation from the wear component so maintenance can be more targeted.
- They support the jawbone better over time than options that do not transmit chewing force into bone in the same way.
This does not mean bridges and dentures are poor treatments. They still have a place. A bridge can be a sensible option when implant surgery is not appropriate. A denture can be the right interim or definitive choice in some mouths and budgets.
But if the question is purely about preserving structure and creating a long-term replacement for a missing tooth, implants usually have the advantage.
For patients comparing a tooth-supported restoration with an implant-supported one, it also helps to understand how crowns and bridges function in their own right. This overview of dental crowns and bridges is useful background if you are weighing both paths.
Decision rule: If two options can replace the tooth, the one that preserves more natural structure and isolates future maintenance more cleanly usually offers the stronger long-term position.
Protecting Your Investment A Maintenance Schedule for Your Implants
The people whose implants last well are rarely doing anything dramatic. They are doing the routine things properly, and they are doing them for years.
Implant maintenance works best when it is built into normal life. If your care plan is too complicated to follow on a rushed weekday morning, it will not last. The goal is a routine you can keep.
Daily care at home
Think of home care as the first line of defence against inflammation around the implant.
A solid daily routine includes:
- Brush the gumline carefully
Spend time where the crown meets the gum, not just on the visible chewing surface. - Use a cleaning aid that fits the space
Some patients do well with floss. Others clean more effectively with interdental brushes or a water flosser. - Notice changes early
Bleeding, a bad taste, food trapping, or tenderness around the implant should not be ignored. - Wear a night guard if prescribed
If you clench or grind, that extra protection can reduce stress on the crown and surrounding structures.
Professional reviews every 6 to 12 months
Regular maintenance is where many implant problems are caught before they become expensive or difficult.
At a review appointment, a dentist or hygienist can assess:
| What is checked | Why it matters |
|---|---|
| Gum health around the implant | Early inflammation can often be managed before bone is affected |
| Plaque and calculus build-up | Deposits around implants are harder to judge accurately at home |
| Bite and wear | Heavy contact can damage the crown or overload the implant |
| Stability of components | Small mechanical issues can be corrected before they become larger ones |
| Bone support on imaging when needed | X-rays help confirm the tissue support below the gumline |
Australian guidance referenced in the verified material supports maintenance every 6 to 12 months for long-term implant performance. In practice, the right interval depends on your history, dexterity, gum health, and risk factors.
What should send you back sooner
Do not wait for severe pain. Implant complications often start subtly.
Book an earlier appointment if you notice:
- Bleeding when cleaning around the implant
- Persistent puffiness or redness
- A loose feeling in the crown
- A new clicking sensation when chewing
- Recurrent food packing in an area that was previously easy to clean
Tip: “It doesn’t hurt” is not a reliable way to judge implant health. By the time an implant problem becomes painful, the issue is often more advanced.
Maintenance is part of the treatment, not an add-on
This point is worth being direct about. If someone is not prepared to maintain an implant, they are not prepared to have one.
That is not said to discourage treatment. It is said because implants do best when patients understand the commitment from the beginning. You are not buying an object. You are entering a long-term maintenance relationship with your mouth.
If you want a good baseline for routine preventive visits, this guide to a check-up and clean explains what regular monitoring and professional cleaning involve.
Start Your Journey to a Lasting Smile in Dulwich Hill
The most useful answer to how long do dental implants last is not a single number. It is a principle.
Implants last best when the foundation is planned properly, the restoration is designed well, and the patient looks after it consistently. That is the pattern behind long-term success.
For some people, the right next step is replacing one missing tooth before the bite shifts further. For others, it is deciding whether several failing teeth are worth saving, or whether a broader solution makes better sense. The correct choice depends on the condition of the teeth, gums, bone, bite, health, and habits. No statistic can replace that individual assessment.
A proper consultation should leave you with clear expectations, not pressure. You should understand what is possible, what the likely maintenance looks like, and what risks apply in your situation. If anxiety has delayed treatment, that should also be part of the discussion. Gentle techniques, laser-assisted care, and sedation options can make treatment far more manageable than many patients expect.
For busy Inner West patients, convenience matters too. Late appointments, Saturday availability, and online booking make it easier to keep the maintenance side of treatment on track once the implant is in place. That ongoing follow-up is part of what protects the result.
If you have been comparing options, looking at old photos, chewing around one side, or wondering whether now is the right time, a consultation is often the point where uncertainty becomes a plan. Seeing real treatment outcomes can help as well. This gallery-style discussion of dental implants before and after gives a clearer sense of what implant treatment can achieve in everyday cases.
The goal is not just to replace a tooth. It is to restore function in a way that still makes sense years from now.
If you are ready to talk through your options, The Smile Spot offers personalised implant consultations in Dulwich Hill with Dr. Dimitrios Thanos, along with advanced laser dentistry, sedation options for anxious patients, and practical appointment times for busy Inner West families and professionals.