A missing tooth rarely feels like “just one tooth”.
It changes small moments first. You chew on one side. You avoid crusty bread or steak. You notice yourself smiling with your lips closed in photos. If the gap is near the front, even speaking can feel different. If it’s further back, you might tell yourself it doesn’t matter much, until the neighbouring teeth start shifting or the area becomes harder to keep clean.
For many people in Dulwich Hill and the Inner West, the next question is simple but stressful. What’s the best way to replace it without ending up with something bulky, loose, or obvious?
An endosseous dental implant is the modern answer many dentists recommend because it replaces the missing tooth from the root up, not just the visible part. It’s designed to restore chewing, appearance, and day-to-day confidence in a way that feels stable and natural.
If you’re still weighing things up, it helps to see what implant treatment can achieve in real patients. These dental implants before and after examples give a useful visual reference for how a gap can be restored.
Restoring Your Smile Starts Here
A patient might come in saying, “I can manage fine.” Then, as we talk, the full story emerges.
They’ve stopped chewing on one side. They feel self-conscious at work meetings. They don’t like how the gap catches in the mirror. Sometimes the tooth has been missing for years, and they’ve adapted. People are very good at adapting, even when something is affecting comfort, confidence, and oral health.
That’s why implant treatment matters. It isn’t only about filling a space. It’s about restoring what the original tooth used to do.
Why a missing tooth affects more than appearance
A tooth does two jobs. The crown is the visible chewing surface. The root sits in the jaw and helps the bone stay active. When a tooth is lost, both functions disappear.
Patients often notice:
- Eating changes: chewy or crunchy foods become awkward
- Speech can feel less precise: especially with front teeth
- Confidence drops: many people smile differently without realising it
- The gap becomes a weak point: food traps, shifting teeth, and bite changes can follow
An endosseous implant addresses the missing root as well as the missing tooth. That’s the key difference.
A well-planned implant doesn’t just “fill a hole”. It rebuilds support where the natural tooth used to be.
For a new patient, the term can sound technical. It isn’t as complicated as it seems. Once you understand the parts and the healing process, the treatment makes much more sense, and usually feels much less intimidating.
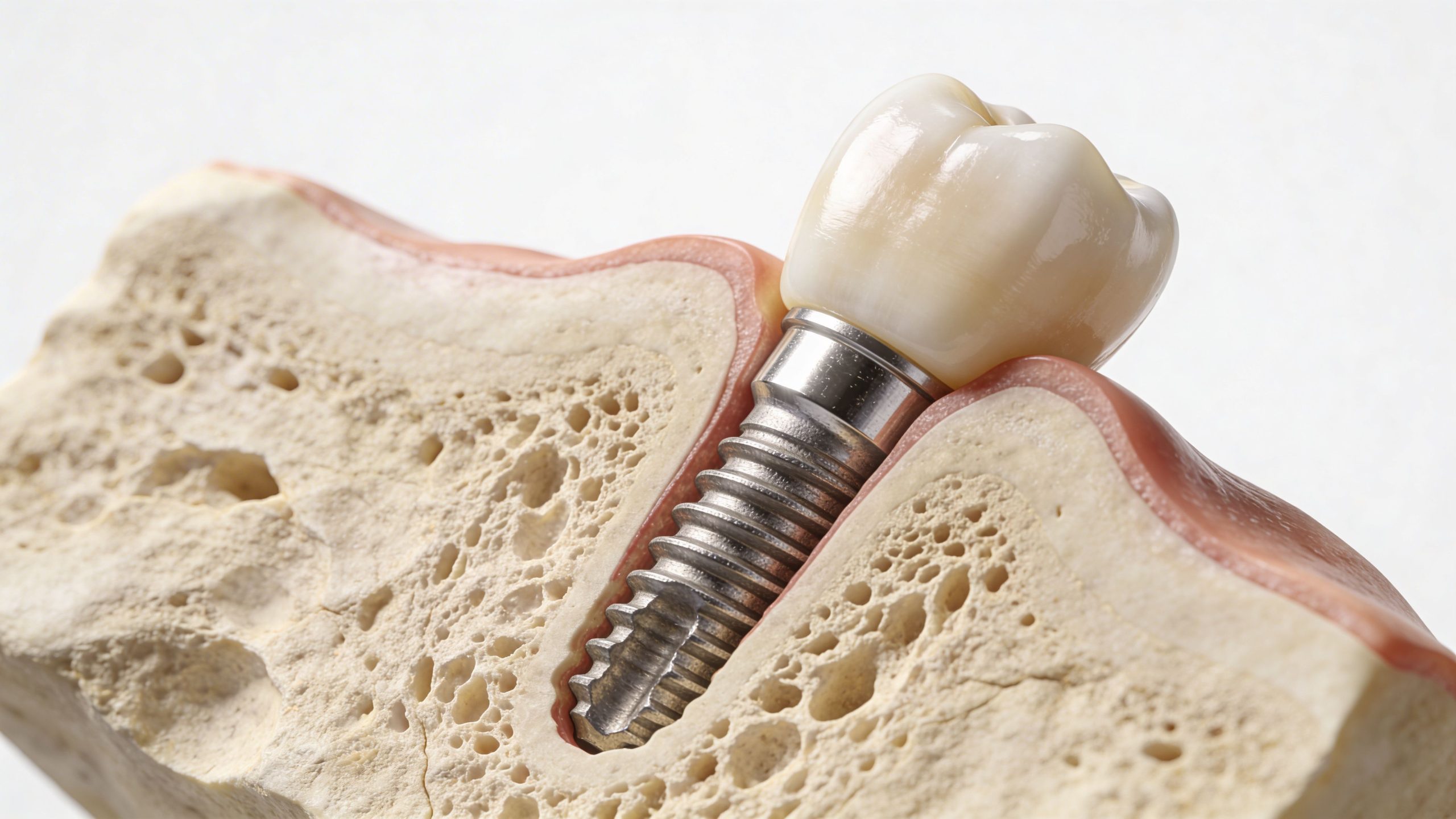
What Is an Endosseous Dental Implant
The word endosseous means within the bone. So an endosseous dental implant is an implant placed into the jawbone, where the root of your natural tooth once sat.
That may sound surgical, but the idea is straightforward. Think of it as a replacement root with a new tooth attached on top.
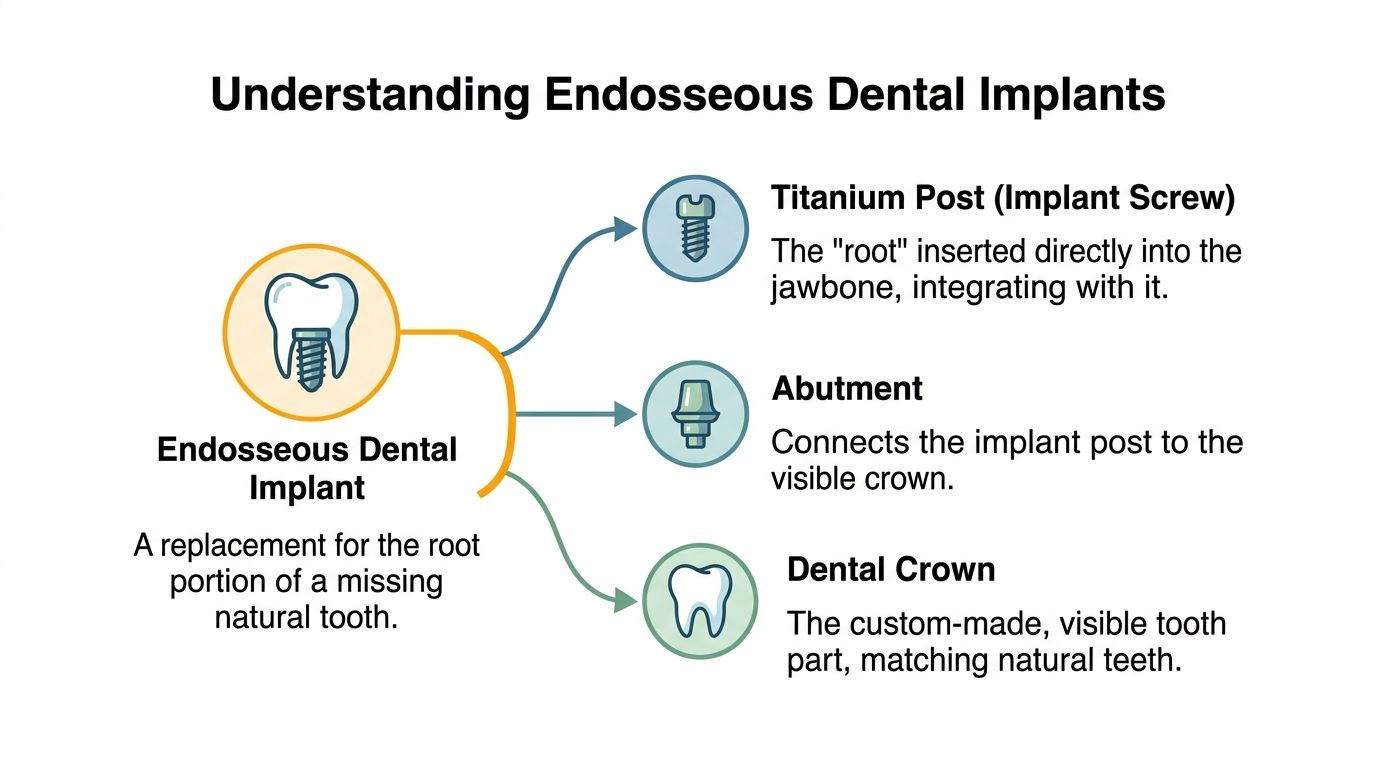
The three parts that make up the implant
Every implant restoration has three main components:
The implant post
This is the part placed into the jawbone. It acts like an artificial root.The abutment
This small connector sits between the implant and the final tooth.The crown
This is the visible part that looks like a natural tooth and does the chewing.
A simple way to picture it is a wall anchor system. The post is the anchor inside the wall, the abutment is the connector, and the crown is the finished item you see.
What osseointegration means
The most important concept is osseointegration. This is the biological process that gives implants their stability.
Osseointegration is the bond that forms when the jawbone heals closely around the implant surface, helping it become secure enough to support a replacement tooth.
I often explain it like a tree root settling into soil. At first, the root is placed carefully into position. Over time, the surrounding ground firms around it and holds it steady. With an implant, your bone does that job.
That’s why the healing period matters. The implant doesn’t rely on glue or pressure alone. It relies on your own bone healing around it.
Why this type of implant is so widely used
Endosseous implants are the most common implant type used in modern dentistry. Their uptake is broad enough that the global market is valued at approximately $5 billion in 2025 and projected to grow to over $9 billion by 2033, reflecting how established they’ve become in practice (endosseous dental implant market data).
If you’ve heard of full-arch solutions, the same principle applies there too. Treatments such as All-on-4 dental implants use strategically placed implants to support a complete arch of teeth.
For a single missing tooth, multiple missing teeth, or a full-arch case, the foundation is the same. A stable root replacement inside the bone gives the final teeth something secure to sit on.
Exploring Implant Materials and Designs
Not every implant is identical. Dentists choose materials and shapes based on your bone, your bite, and the goals of treatment.
The two material discussions patients ask about most are titanium and zirconia. Then there’s design, especially whether an implant is tapered or more parallel-sided.
Titanium vs zirconia implants
Titanium remains the standard option in most implant dentistry because it has a long clinical track record. Zirconia is the main metal-free alternative.
| Feature | Titanium Implants | Zirconia Implants |
|---|---|---|
| Material | Metal implant material with a long history of use | Ceramic, metal-free material |
| Clinical track record | Strong long-term evidence base | Growing evidence, but less established |
| Performance in cited Australian-related data | Titanium implants show 95.8% survival in the cited comparison | Zirconia shows 90.9% survival in the cited comparison |
| Typical reason for selection | Proven osseointegration and versatility | Preference for a metal-free option |
| General takeaway | Most commonly recommended | Suitable in selected cases |
The broader longevity discussion matters to patients too. If you want a practical view of maintenance and durability, this guide on how long dental implants last is a useful companion read.
Why implant shape matters
Shape influences how the implant grips the bone at placement.
According to the cited health technology assessment summary, screw-type tapered endosseous implants increase bone-implant contact by 20 to 30% at 4 weeks compared with cylindrical designs and are often preferred for high initial stability, with torque benchmarks of 35 to 45 Ncm (INAHTA summary on tapered implant design).
That sounds technical, but the patient version is simple. A tapered implant often behaves a bit like a well-designed screw in timber. It can engage the surrounding bone more firmly at the start.
What this means in the chair
Your dentist may recommend one implant over another because of:
- Bone quality: softer bone may benefit from a design that improves initial grip
- Position in the mouth: front teeth and back teeth can place different demands on the restoration
- Bite force: heavy clenching or grinding can influence the choice
- Aesthetic needs: especially where the smile line is high
- Material preference: some patients specifically ask about metal-free options
Practical rule: the “best” implant isn’t a brand slogan or a trendy material. It’s the one that fits your anatomy, bite, and long-term treatment plan.
Patients sometimes assume they need to choose the implant themselves. In reality, your role is to understand the options and ask good questions. Your dentist’s role is to match the design to your case.
Are You a Suitable Candidate for Implants
This is usually the first big concern. Not “What is it?” but “Am I a candidate?”
Many people are candidates for an endosseous dental implant, even if they’ve been told they have bone loss, gum issues in the past, or a medical condition that needs to be managed carefully. The key is proper assessment.

What dentists look for first
A consultation usually focuses on a few essentials:
- Healthy gums or controllable gum disease: active infection needs attention before implant placement
- Enough bone support: if the area is thin or reduced, grafting may be considered
- Stable general health: healing matters
- Commitment to home care: implants need ongoing cleaning and reviews
Age alone doesn’t usually decide suitability. A healthy older adult may be a stronger candidate than a younger person with uncontrolled gum disease and poor oral hygiene.
Smoking and diabetes
Some conditions don’t automatically rule implants out, but they do change the level of planning.
In NSW, daily smokers can have implant failure rates 2 to 3 times higher than non-smokers, while the 10% of Inner West adults with diabetes may see a 15 to 20% higher complication rate, though these risks can often be managed with advanced clinical protocols (NSW smoking and diabetes considerations for endosteal implants).
That doesn’t mean “you can’t have implants.” It means your dentist needs to assess healing carefully, discuss risk openly, and build a treatment plan around it.
Questions worth asking at your consult
If you’re unsure whether implants are worth pursuing, ask direct questions:
- How much bone is available in my case
- Do I show signs of grinding or bite overload
- Would I need grafting before or during treatment
- How do my smoking or medical history affect healing
- What can I do before treatment to improve success
For people comparing replacement options, this article on whether dental implants are worth it can help frame the decision.
The best candidate isn’t the person with the “perfect mouth”. It’s the person whose risks are understood and managed well.
That’s especially important for anxious patients. A calm, detailed assessment often removes more fear than people expect, because uncertainty is usually the hardest part.
Your Implant Journey from Consultation to Aftercare
The implant process feels much easier when you know the sequence. Anxiety often comes from not knowing what happens next.
Most treatment follows a clear path. There may be small variations depending on whether you need an extraction, grafting, or a temporary tooth, but the general journey is consistent.
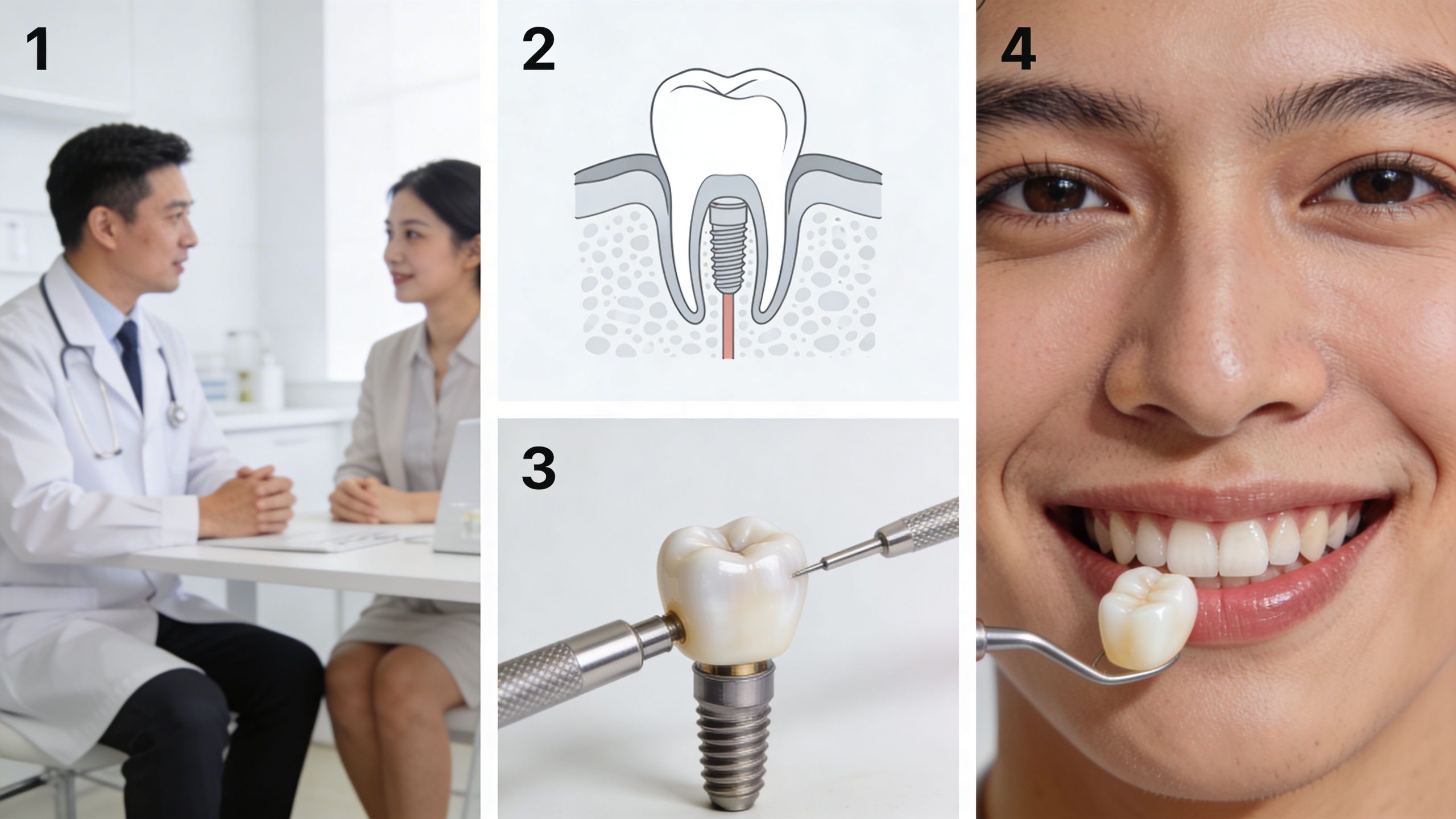
Consultation and planning
The first visit is about diagnosis, not rushing into surgery.
Your dentist examines the mouth, reviews your health history, and uses imaging to see the bone and nearby structures clearly. For anxious patients, this appointment is also where comfort planning begins. If someone has had difficult dental experiences before, it helps to say that early. It changes how the whole journey is managed.
Typical planning points include:
- The position of the missing tooth
- Bone width and height
- Gum condition around the area
- Bite pressure and spacing
- Whether a temporary tooth will be needed
If bone support is limited
This is one of the most common points of confusion. Patients often hear “bone graft” and assume the whole plan has collapsed. It hasn’t.
Some sites need additional support before or at the time of implant placement. For patients with bone deficiencies, prosthetically guided bone augmentation has shown a 92% success rate in gaining bone volume, and this is especially relevant because 25% of NSW residents aged 55+ have a history of severe periodontitis (ITI discussion of hard and soft tissue deficiencies around implants).
In plain terms, if the bone isn’t ideal, there are often ways to rebuild the foundation rather than abandon the idea of an implant.
The day of implant placement
This is usually more controlled and less dramatic than patients imagine.
The area is numbed thoroughly. If you’re nervous, talk to your dentist about sedation options. A gentle team, clear communication, and minimally invasive methods can make a major difference. In practices that use advanced tools such as Biolase laser dentistry, treatment may be planned to reduce tissue trauma and support cleaner, more precise site management.
You may feel pressure or vibration during placement, but pain should be controlled.
Most patients say the anticipation was worse than the procedure itself.
Healing and osseointegration
After placement, the implant needs time to integrate with the bone. This is the quiet phase, but it’s one of the most important.
Healing instructions usually focus on protecting the site, keeping it clean, and avoiding unnecessary pressure. Depending on the case, you may wear a temporary replacement while the area settles.
Some patients like seeing a visual overview of the process before treatment. This short explainer can help make the stages feel more familiar.
Abutment and final crown
Once integration is confirmed, the connecting piece is fitted and the final crown is made to match your bite and surrounding teeth.
At this stage, the treatment begins to feel “real” for many people. Up until then, patients tend to think mostly about surgery. At this stage, the focus shifts to function, comfort, and appearance.
The final checks usually include:
- Fit and stability
- Bite balance
- Shape and colour match
- Cleaning access around the implant
Aftercare in daily life
An implant isn’t high-maintenance, but it isn’t maintenance-free either.
You still need regular reviews, careful brushing, and cleaning around the gumline. If you clench or grind, a night guard may be recommended. Long-term success depends on both the clinical work and the home care that follows it.
For anxious patients, aftercare matters psychologically as well. Knowing what is normal, who to call, and when to come back gives the whole experience a calmer feel.
Weighing the Benefits and Risks of Dental Implants
A good treatment decision needs honesty. Implants offer major advantages, but no dental procedure is risk-free.
The strongest argument for implants is that they replace a missing tooth in a way that feels close to natural structure and function. They sit independently, so neighbouring teeth usually don’t need to be cut down the way they often do for a traditional bridge. They also feel more secure than a removable denture for many people.
Why many patients prefer implants
The practical benefits tend to matter most:
- Chewing confidence: food feels easier to manage
- A natural appearance: the restoration is designed to blend with surrounding teeth
- Speech support: especially where missing teeth have affected pronunciation
- Jawbone support: replacing the root helps preserve function in the area
- No reliance on adjacent teeth: healthy teeth often remain untouched
The risks to understand
The main risks include failure to integrate, infection around the implant, and mechanical problems such as loosening of components. Rarely, treatment can be complicated by anatomy, bite force, or delayed healing.
The reassuring part is that modern implant dentistry performs well over time when planning and aftercare are done properly. Australian studies report a 95%+ success rate for endosseous implants over 15 years, with peri-implantitis at 2.6%, while traditional bridges have a 20 to 30% failure rate within 10 years (Australian-related implant longevity and bridge comparison data).
A balanced way to think about it
Dentures and bridges still have a place. Some patients are better suited to them. Some prefer them. Some need them as interim treatment.
But if your goal is a fixed solution that restores support from the bone upward, an endosseous dental implant is often the closest replacement to the structure of a natural tooth.
Good implant treatment isn’t about pretending there are no risks. It’s about reducing them through diagnosis, planning, skilled placement, and careful maintenance.
That’s the mindset patients should look for in any implant consultation.
Your Local Implant Solution at The Smile Spot
Choosing implant treatment is one decision. Choosing where to have it done is another.
For patients in Dulwich Hill, Marrickville, Ashfield, Summer Hill, Lewisham, Petersham, Earlwood, and nearby parts of the Inner West, convenience matters, but so does trust. Implant care works best when the clinic combines experience, thoughtful planning, and a calm approach for patients who feel nervous about dental treatment.
Dr. Dimitrios Thanos has led The Smile Spot since 1996, bringing long-standing clinical experience to family, restorative, and implant dentistry. That matters because implant cases aren’t only about placing a fixture in bone. They involve diagnosis, bite planning, aesthetics, maintenance, and understanding how to care for patients who may already feel apprehensive.
Comfort matters as much as the technical work
Many people who delay treatment aren’t worried only about the result. They’re worried about the experience.
That’s where gentle technique, clear communication, and advanced tools can make a real difference. The Smile Spot uses Biolase laser dentistry as part of its minimally invasive approach, and sedation is available for anxious patients. For someone who has postponed care for months or years, that can be the difference between staying stuck and finally moving forward.
Clear fees and practical planning
Patients also want transparency.
The final cost of implant treatment depends on factors such as the number of teeth being replaced, whether bone grafting is needed, the complexity of the restoration, and the type of implant-supported solution chosen. What helps is having those factors explained plainly, without pressure.
The Smile Spot is known for straightforward care planning and transparent fees, including a $240 complete care package for exam, X-rays, scale and fluoride as part of its broader philosophy of making dental care easier to understand and access.
If you’d like to explore options for a single implant or a more complex restoration, the clinic’s dental implants page for Dulwich Hill is the best place to start.
For busy families and professionals, practical details matter too. Online booking, late appointments, and Saturday availability make it easier to fit treatment into normal life.
Frequently Asked Questions About Endosseous Implants
Is getting an implant painful
Most patients say it’s more manageable than they expected. The area is numbed thoroughly during the procedure, and anxious patients can often discuss sedation options in advance. After treatment, it’s normal to have some soreness, but it’s usually described as post-procedure tenderness rather than severe pain.
How long does an endosseous dental implant last
With good placement, regular reviews, and careful home care, implants can serve for many years. Their long-term performance depends on the bone, the bite, medical factors, and how well the area is kept clean.
Do implants feel like real teeth
They can feel very natural because they are fixed in place rather than removable. Once the final crown is fitted and your bite is balanced properly, many patients stop noticing the implant in day-to-day life.
Do I need special cleaning tools
Not always, but you do need excellent cleaning habits. Your dentist may recommend specific brushes, floss aids, or other cleaning tools depending on the implant’s position and the shape of the restoration.
Can anxious patients still have implant treatment
Yes. In fact, anxious patients often do very well when the process is explained carefully and managed in stages. Knowing what’s happening, having enough time to ask questions, and planning comfort measures in advance can change the experience completely.
What if I’ve been missing the tooth for a long time
That doesn’t automatically rule you out. Long-standing gaps can sometimes mean reduced bone in the area, but many patients can still be treated, sometimes with additional planning or augmentation. The only way to know is with a proper examination and imaging.
If you’re considering an implant and want clear advice without pressure, The Smile Spot can help. Book a consultation to find out whether an endosseous dental implant is right for you, and get a personalised plan built around comfort, function, and long-term oral health.