If you've recently been told you have gum disease, your mind probably went straight to the unpleasant possibilities. Deep cleaning. Surgery. Needles. Time off work. A sore mouth for days. That reaction is common, especially if you're already a bit nervous in the dental chair.
Laser periodontal therapy often comes up at exactly that moment. It sounds modern, and it is. It can also be gentler than many people expect. But it's not magic, and it isn't the right answer for every gum problem. The most useful way to understand it is to look at what it does well, where its limits are, and how it fits alongside proven periodontal care.
A Modern Approach to Gum Health
Gum disease usually doesn't feel dramatic at first. Many people notice a little bleeding when brushing, some tenderness, bad breath, or gums that seem to be pulling away from the teeth. By the time pockets have formed around teeth, the condition often needs more than a standard clean.
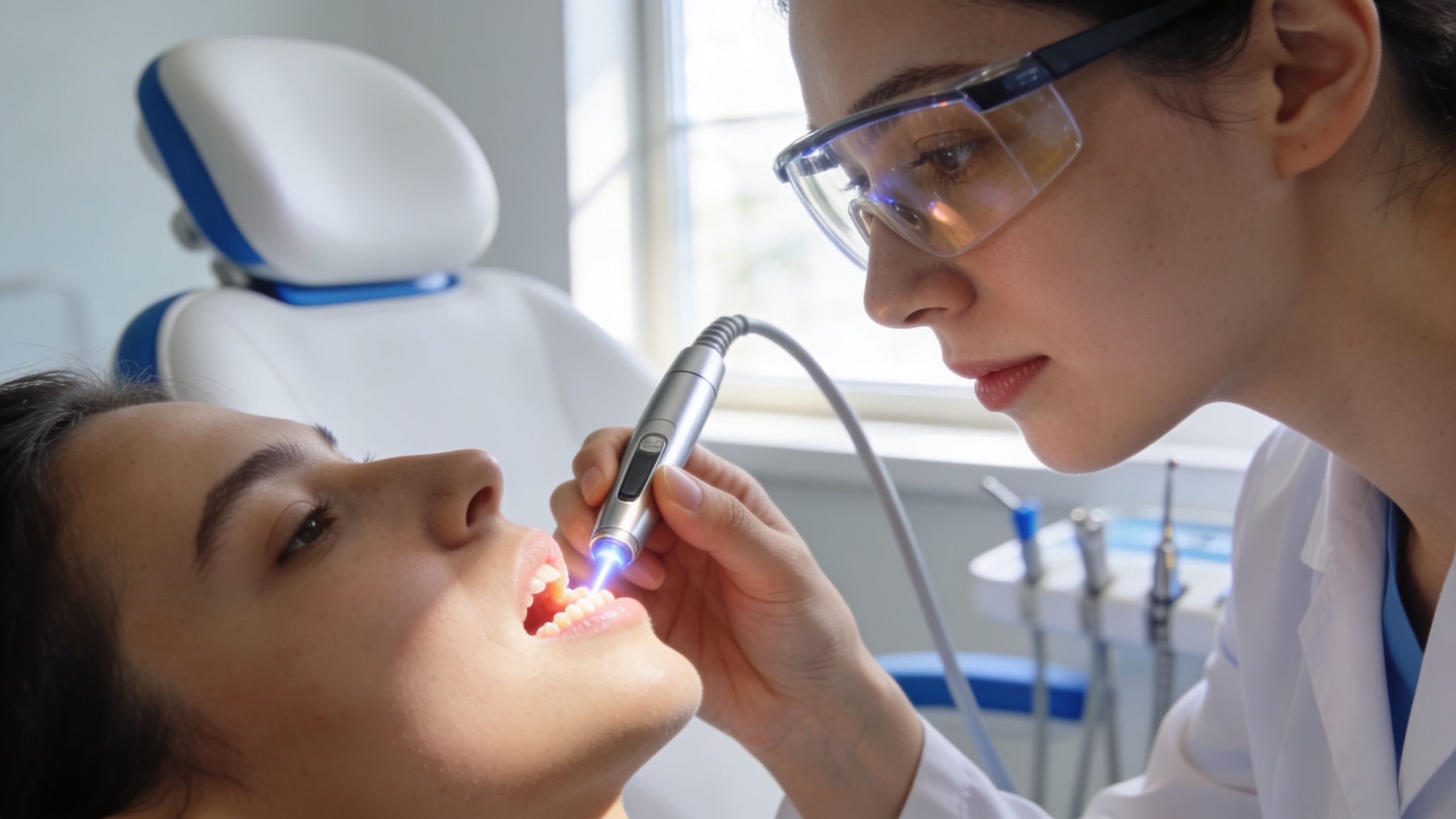
That's where laser periodontal therapy can sound appealing. Instead of relying only on hand instruments or more invasive surgery, dentists can use focused light energy to target diseased tissue inside the gum pocket. For anxious patients, that matters. The idea of a more precise, less intimidating treatment can make it easier to stop delaying care.
Why patients ask about lasers
Patients aren't looking for “high-tech dentistry” for its own sake. They want three things:
- Less fear: They want treatment that feels more controlled and less confronting.
- Less disruption: They want to get back to work, school runs, meals, and sleep without a rough recovery.
- Clear answers: They want to know whether a laser is better for their situation, not just better marketed.
A laser can be a very useful tool when used thoughtfully. In practice, the biggest advantage is often precision. The dentist can work inside infected gum pockets in a way that aims to remove diseased tissue while being conservative around healthy structures.
A good periodontal plan isn't about choosing the fanciest device. It's about choosing the least invasive option that still gives the gums a real chance to stabilise.
Gentle doesn't mean casual
This part matters. Gum disease is a chronic infection-driven condition. A gentler technique is only helpful if it still addresses the underlying problem. That means proper diagnosis, careful cleaning of the root surfaces, realistic follow-up, and home care that supports healing.
Patients who value a calm, low-pressure experience often start by looking for a gentle dentist near me. That instinct makes sense. The right environment can make it much easier to begin treatment early, before the gums and supporting bone are affected more severely.
Laser therapy fits that modern, comfort-focused approach well. But the honest version is better than the glossy version. Sometimes it's an excellent adjunct. Sometimes conventional treatment is enough. Sometimes surgery is still the right call.
Understanding How Dental Lasers Treat Gum Disease
Think of an infected gum pocket like a narrow garden bed with weeds growing between delicate roots. You don't want to rip up the whole garden. You want to remove the unhealthy material as precisely as possible, reduce the bacterial load, and give the healthy tissue a better environment to recover.
That's the principle behind laser periodontal therapy.
What the Biolase laser actually does
Biolase systems use light at specific wavelengths to target infected tissue and bacteria inside periodontal pockets. According to the verified clinical summary, the laser fibre is just 200 to 400 μm thick, which allows access into narrow areas, and its pulsed energy has a bactericidal effect that can reduce harmful pathogens such as Porphyromonas gingivalis by up to 99.9% in vitro, while helping minimise thermal damage to surrounding healthy tissue and supporting formation of a stable fibrin clot for healing (clinical overview of Biolase laser effects).
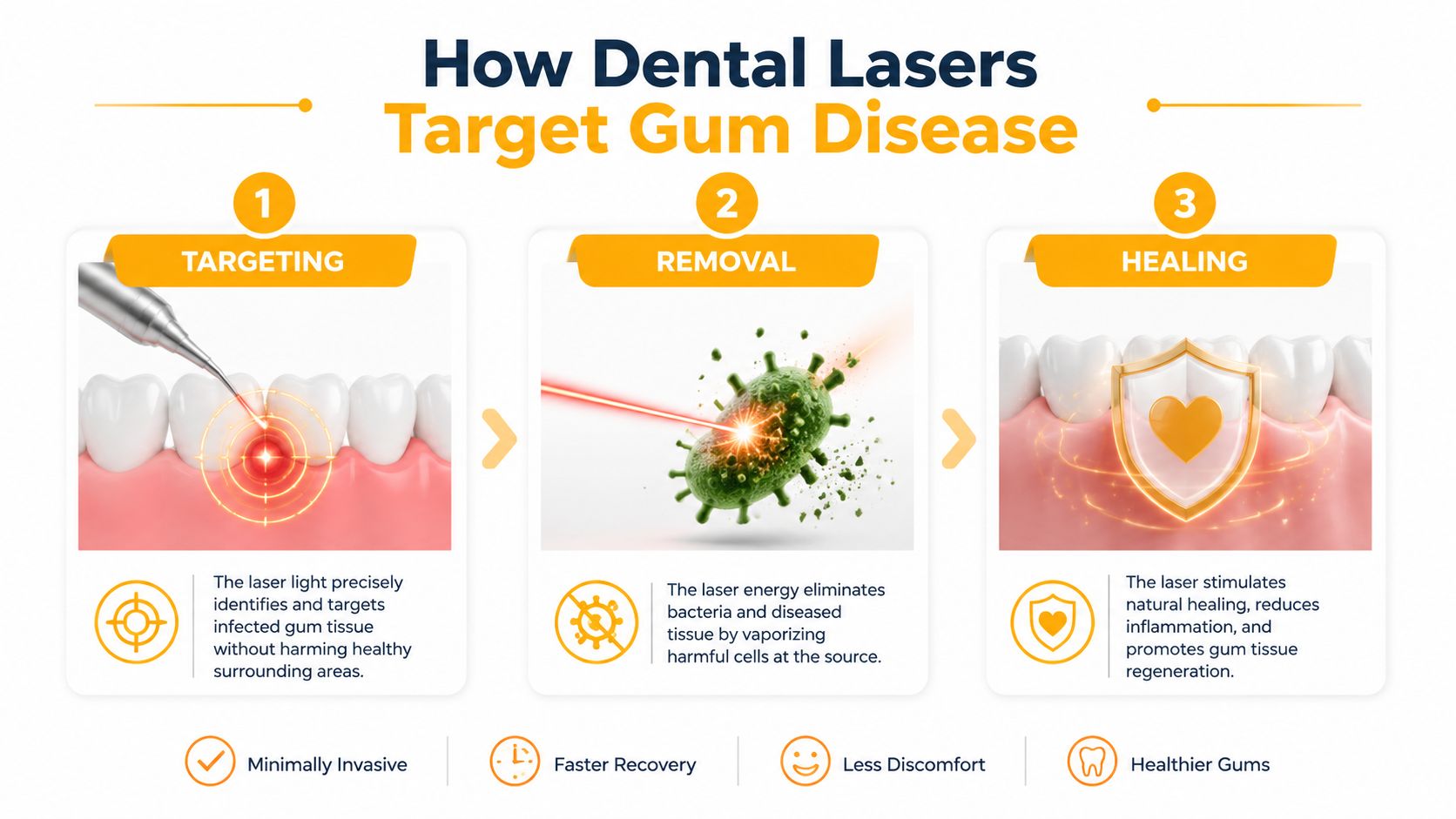
Why that precision matters
The practical aim isn't just “zap the gums”. The aim is to improve the condition inside the pocket.
A laser can help by:
- Targeting diseased tissue: It focuses treatment where inflammation and infection are active.
- Reducing bacteria: Lowering the bacterial load may help calm the environment around the tooth.
- Supporting clot stability: A stable fibrin clot helps protect the treated site during early healing.
- Limiting collateral trauma: Precision matters in areas where the gum, root surface, and supporting tissues are already under stress.
That's one reason many clinicians use laser therapy as part of a broader periodontal plan rather than as a stand-alone event. It can complement mechanical debridement instead of replacing the fundamentals.
Technology helps, but process still matters
Even advanced equipment only works well when the appointment is organised carefully. In healthcare settings, the workflow around treatment matters almost as much as the device itself. Good timing, proper follow-up, and consistent protocols all affect patient experience. If you're curious how operational systems shape care quality more broadly, this guide to healthcare compliance in scheduling gives a useful behind-the-scenes view.
Precision technology works best when the diagnosis is accurate, the operator is skilled, and the treatment plan is realistic.
Patients who want a closer look at how this fits into modern care can read more about laser dentistry in Dulwich Hill. The key point is simple. The laser isn't there to replace judgement. It's there to improve how carefully treatment can be delivered.
Your Laser Therapy Appointment Step by Step
For many people, the hardest part is not the treatment itself. It's not knowing what the appointment will feel like. A clearer picture usually reduces anxiety fast.
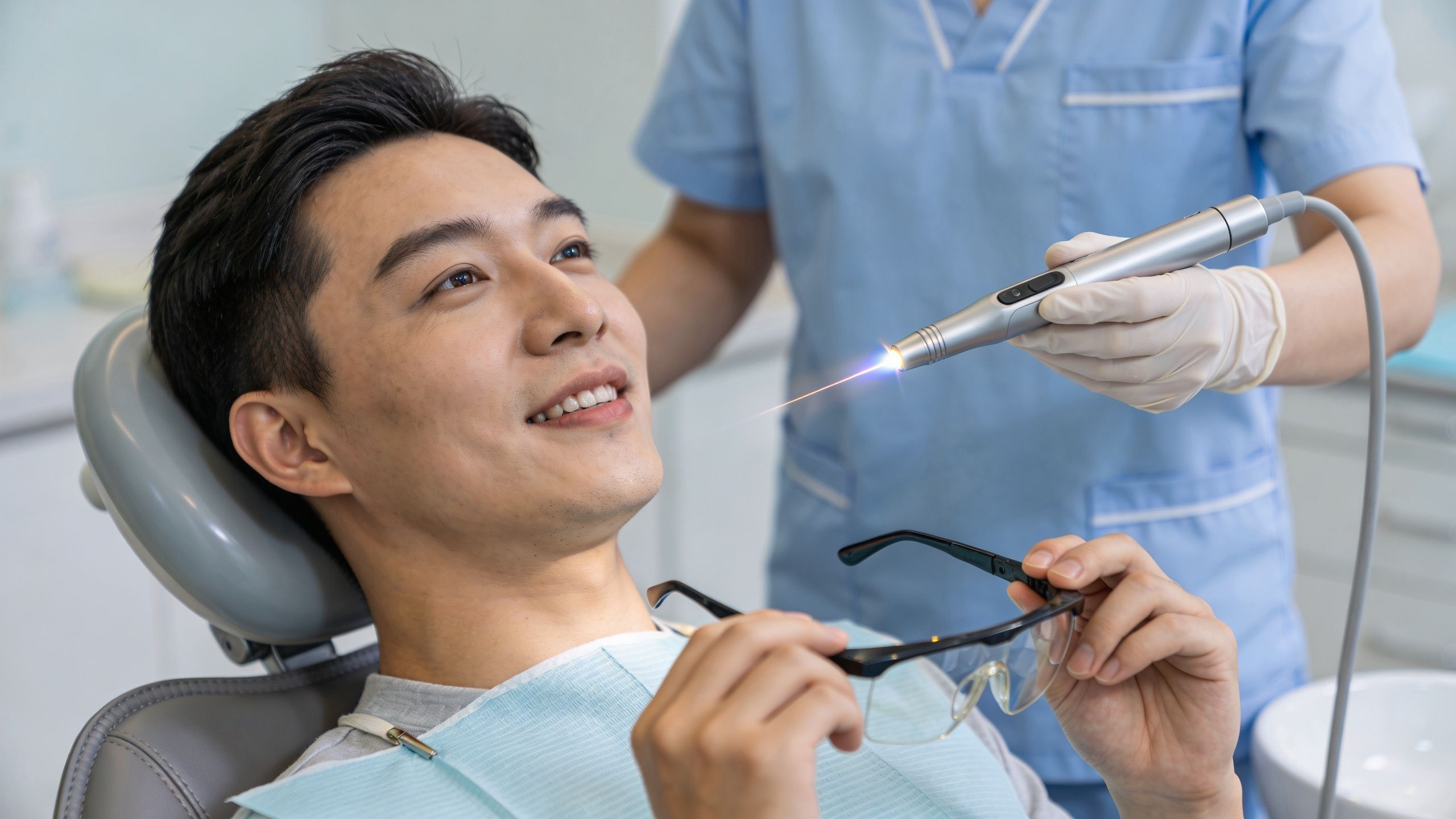
Before the laser starts
The appointment usually begins with an examination of the gums, pocket measurements, and a discussion of what the treatment is trying to achieve. If there's heavy calculus, inflammation, or deeper pocketing, laser therapy is usually planned as part of a broader periodontal approach rather than as a cosmetic add-on.
Comfort is addressed early. Some patients need local anaesthetic, and some need very little, depending on the area being treated and how inflamed the gums are. If you're anxious, say so plainly. That changes how the appointment is paced.
During treatment
Once the area is numb, the laser fibre is guided into the gum pocket. Patients often describe the sensation less as pain and more as pressure, vibration, or an odd awareness that something precise is happening. The goal is controlled treatment of diseased tissue and bacterial contamination inside the pocket.
A simple way to think about the sequence is this:
- Access the pocket and identify the treatment area.
- Use the laser carefully within the diseased space.
- Clean the root surface as needed so the pocket isn't left with the underlying cause untouched.
- Allow the tissue to settle so healing can begin in a cleaner environment.
If you like seeing procedures before you commit, this short video can make the process feel much more familiar.
Right after the appointment
Most patients don't walk out feeling as though they've had major surgery. The gums may feel tender, a little tight, or slightly sensitive, but the experience is usually easier to tolerate than many people expected before coming in.
Common post-treatment advice includes:
- Eat gently: Soft, non-irritating foods are usually easier at first.
- Clean carefully: You'll be told how to brush around the treated area without disrupting healing.
- Keep review visits: Periodontal treatment succeeds with monitoring, not wishful thinking.
If you've ever put off gum treatment because you were worried about the appointment itself, a simple check-up and clean is often the best first step. It gives you measurements, options, and a plan before anything more involved is decided.
Benefits of Laser Therapy Compared to Traditional Treatment
Laser therapy gets talked about as though it automatically beats older methods. That isn't the right comparison. The better question is where it offers practical advantages, and where conventional treatment still holds its ground.
A fair side-by-side view
| Concern | Laser periodontal therapy | Conventional scaling or surgery |
|---|---|---|
| Patient comfort | Often feels less invasive to patients, especially those worried about cutting and sutures | Familiar, proven, but can feel more confronting when surgery is required |
| Precision | Can target diseased tissue within the pocket with a very fine fibre | Mechanical instruments remain highly effective for root surface cleaning |
| Recovery experience | Many patients report an easier immediate recovery experience | Recovery varies widely, especially if flap surgery is involved |
| Role in treatment | Often best used as an adjunct | Remains the core foundation of periodontal therapy |
| Evidence base | Promising in some protocols, mixed in others | Long-established and still the benchmark for many cases |
Where regenerative protocols stand out
Some advanced laser protocols are designed not just to disinfect a pocket, but to support regeneration. Verified data for LANAP states that multicentre trials showed 2 to 4 mm of clinical attachment level gain and significant bone density increases at 2 years, compared with 0.5 to 1 mm with conventional scaling and root planing alone, with the proposed mechanism linked to laser biostimulation of growth factors that support new tissue formation (LANAP patient protocol summary).
That's important, but it needs context. Not every laser treatment is LANAP. Not every patient is suitable for a regenerative protocol. And not every gum problem should be framed as a race between “old dentistry” and “new dentistry”.
What works best in real life
In everyday care, treatment choice usually comes down to three questions:
- How advanced is the disease?
- How deep are the pockets?
- Can the patient maintain the result afterwards?
For some people, deep cleaning and ongoing maintenance are enough. For others, adding a laser improves access and comfort. For advanced cases, surgery may still be the most predictable option, including procedures discussed under gum surgery in Dulwich Hill.
Better technology is only better when it improves the outcome for that patient, in that mouth, at that stage of disease.
Is Laser Periodontal Therapy Right for You?
The honest answer is that laser periodontal therapy is ideal for some people and unnecessary for others.
That shouldn't put you off. It should reassure you. Ethical periodontal care isn't about squeezing every patient into the same treatment. It's about matching the method to the condition.
Patients who may benefit most
Laser therapy is often attractive for people who want a less invasive experience and who have gum pockets that justify more than a routine clean. It can also suit patients who have avoided care because the idea of traditional gum treatment feels overwhelming.
A good candidate often looks like this:
- Moderate periodontal disease: There's enough active disease to warrant targeted periodontal treatment.
- Dental anxiety: The idea of a more conservative approach helps the patient move forward with care.
- Need for adjunctive support: Mechanical cleaning alone may benefit from added bacterial reduction and tissue management.
When it may not be the best option
This is the part many marketing pages gloss over. Verified guidance notes that laser therapy is often promoted as a “no cut, no sew” cure-all, but its effectiveness is nuanced. It tends to work best as an adjunct to traditional methods, patients with shallow pockets of less than 5 mm may see negligible benefit over conventional cleaning, and severely compromised cases may still need surgical treatment (clinical discussion of when laser is recommended).
That means laser therapy may not be the best fit if:
- Your gum issues are mild: A conventional clean may do the job well.
- The disease is advanced and structurally complex: Surgery may still offer the clearest access and control.
- Home care is inconsistent: No technology can compensate for poor long-term plaque control.
The right question isn't “Do you offer lasers?” It's “Am I the kind of case that benefits from one?”
When patients are comparing providers, they often look at patient experiences online. That's sensible, as long as reviews don't replace a clinical exam. If you're interested in how dental practices build trust and feedback systems, this overview on improving online reviews for dentists offers a useful perspective.
Understanding the Costs and Insurance Coverage
This is one of the most important parts of the decision, and it's the part patients are often left to figure out on their own.
A verified review of the patient information gap around laser treatment notes that total cost of ownership and insurance coverage are often unclear, and that patients frequently don't know whether a higher upfront fee is balanced by fewer repeat treatments or whether major Australian health funds will contribute at all (discussion of cost and insurance information gaps).
What actually affects the price
The final fee usually depends on the clinical picture, not on the word “laser” alone. Cost can vary based on:
- How many areas need treatment
- How deep and widespread the periodontal pockets are
- Whether this is adjunctive therapy or part of a more advanced periodontal plan
- How much follow-up maintenance is required
That means asking for a single flat quote over the phone usually won't give you a meaningful answer.
How to think about value
The better way to assess cost is to ask practical questions:
| Question | Why it matters |
|---|---|
| What exactly is included? | You need to know whether reviews, cleaning, laser use, and maintenance are all part of the fee |
| Is this replacing surgery or adding to basic care? | A premium fee makes more sense if it changes the treatment pathway meaningfully |
| What maintenance will I still need? | Gum disease management never ends with one appointment |
| Will my health fund recognise the item numbers used? | Cover often depends on the treatment code, not the marketing label |
Insurance and out-of-pocket reality
In Australia, private health cover may contribute to periodontal treatment, but cover depends on your fund, level of extras, annual limits, and the item numbers claimed. Laser use itself isn't always the part a health fund cares about. The claim may be assessed under the underlying periodontal procedure.
A practical approach is to ask the clinic for a written treatment plan and item numbers before committing. Then ask your insurer what portion is likely to be covered and what your out-of-pocket cost will be.
If spreading treatment costs is a concern, it's worth reading about dentists with payment plans near me. The key is transparency. You shouldn't have to choose between vague promises and financial guesswork.
Frequently Asked Questions
Is laser periodontal therapy scientifically proven to be better?
Not across the board. Verified evidence states that the American Academy of Periodontology does not currently recognise laser therapy as a superior standalone treatment, and major reviews have found inadequate evidence to conclude that laser therapy alone is superior or even comparable to conventional periodontal therapy for outcomes such as attachment gain or pocket depth reduction (systematic review and AAP position summary).
A separate meta-analysis found that Er:YAG laser adjunctive therapy showed a pooled mean difference of 0.319 mm in clinical attachment level gain compared with scaling and root planing alone, but this was not statistically significant, with a 95% confidence interval of −0.097 to 0.735 mm. That review concluded that improvements may be short term and clinically small, and that evidence for other laser systems remains inconclusive due to study limitations and lack of long-term data. In short, lasers should be viewed as supplementary rather than routine adjuncts to conventional therapy.
Does that mean lasers don't work?
No. It means the answer depends on how the laser is used, what protocol is being followed, and what problem is being treated. In practice, lasers can be helpful tools. They just shouldn't be sold as automatic upgrades over every standard treatment.
What is aftercare like?
Aftercare is usually straightforward, but it matters. You'll normally be given guidance about gentle cleaning, food choices, and when to return for review. The healing period is only the first chapter. Long-term stability depends on plaque control, maintenance visits, and keeping inflammation down.
How long do results last?
That depends less on the machine and more on the biology and the habits that follow treatment. If bacterial build-up returns, gum disease can return. Patients who keep up with maintenance and home care give any periodontal treatment a much better chance of lasting.
Is laser treatment a replacement for deep cleaning?
Often, no. Many cases still need conventional root surface debridement as the foundation. Laser therapy may be added to improve tissue management and bacterial reduction, but it usually works best as part of a complete periodontal plan rather than as a shortcut around one.
If you're dealing with bleeding gums, bad breath, gum recession, or a periodontal diagnosis you don't fully understand, the next step is a proper assessment with a team that will explain the trade-offs clearly. The Smile Spot offers advanced, gentle dental care in Dulwich Hill, including laser dentistry, periodontal treatment, and practical guidance on costs, comfort, and what's right for your mouth.