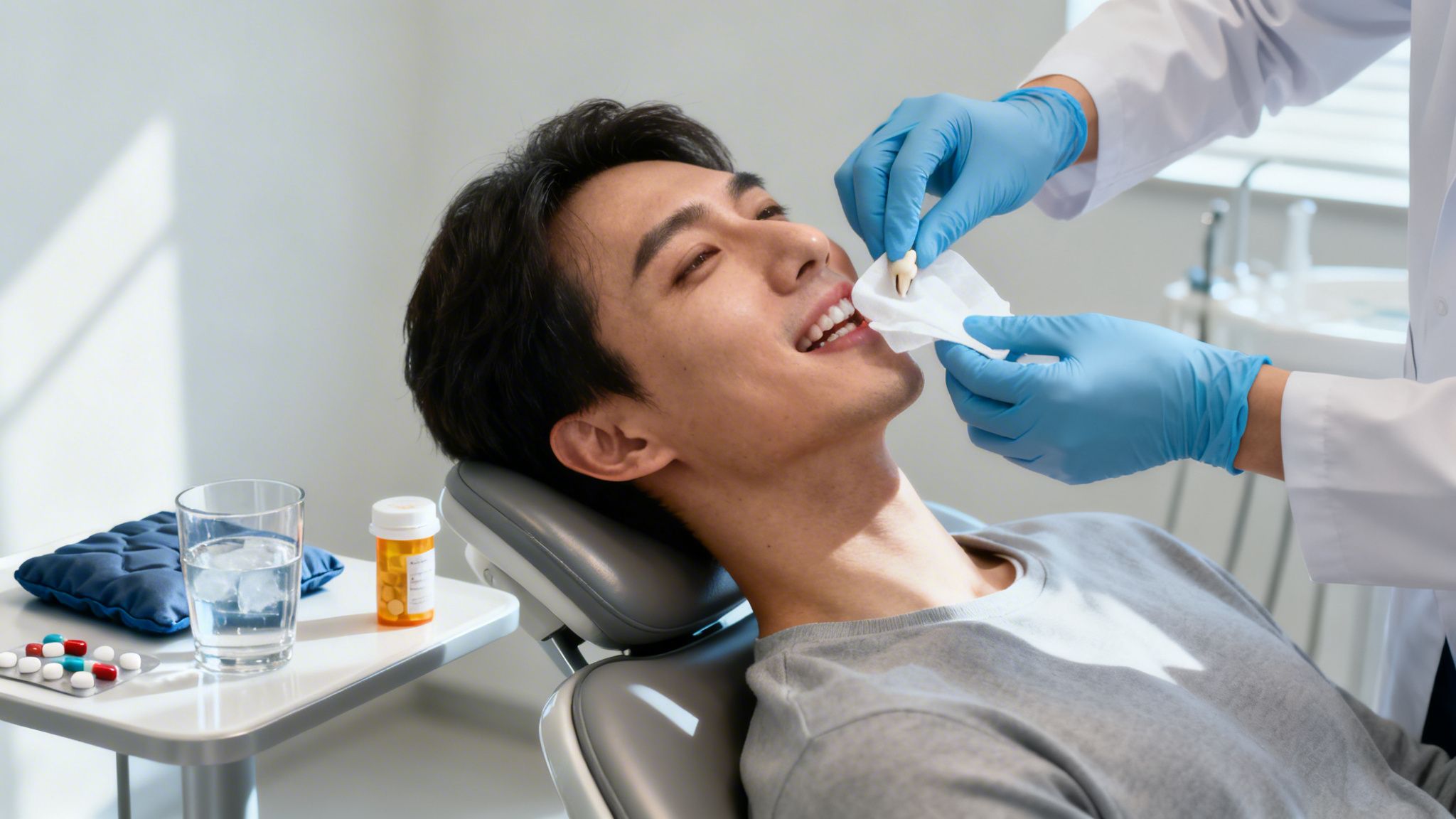
The very idea of wisdom tooth removal pain is often what worries people the most. But the truth is, while some discomfort is a normal part of healing, knowing what to expect can make the whole experience much less stressful and help you recover smoothly.
Let’s break it down so you feel prepared and confident.
Understanding Pain After Wisdom Tooth Removal
Feeling sore after having a wisdom tooth out is completely normal. It’s your body’s natural way of responding to a minor surgical procedure. Think of the extraction site like a small, delicate construction zone in your mouth—your body gets to work right away with a healing process that involves inflammation, which causes the swelling and soreness you feel.
The level of discomfort you experience often depends on why the tooth needed to come out. Many wisdom teeth are impacted, which means they're stuck under the gum or growing in at an awkward angle. Removing an impacted tooth is a bit more complex than a simple extraction, which means your body has a slightly bigger job to do in healing.
Why Do Wisdom Teeth Need to Be Removed?
Not everyone needs their wisdom teeth removed, but they often cause problems simply because there isn’t enough room for them at the back of our jaws. The most common reasons we recommend removal include:
- Impaction: The tooth can’t erupt properly, which can lead to pain, cysts, or even damage to the neighbouring teeth.
- Crowding: As wisdom teeth push through, they can cause other teeth to shift out of alignment.
- Infection and Decay: A partially erupted tooth can create a flap of gum tissue that’s a nightmare to keep clean. It traps food and bacteria, often leading to a painful infection called pericoronitis.
- Preventative Care: Sometimes, your dentist will see on an X-ray that your wisdom teeth are likely to cause problems down the track and recommend removing them proactively.
Getting your wisdom teeth out is incredibly common. In Australia, about 70% of adults aged 25-44 have had at least one removed. Here in the Inner West, data from NSW shows these extractions are a frequent procedure, with most people finding the pain peaks in the first 12-24 hours before starting to improve.
Your Typical Pain Recovery Timeline
Knowing what to expect each day can take the uncertainty out of recovery and turn it into a manageable process. While everyone’s healing journey is unique, most people follow a fairly predictable pattern.
The most intense discomfort and swelling usually happen within the first 48 to 72 hours after your procedure. After this peak, you should notice things getting steadily better each day.
To give you a clearer picture, we've put together a day-by-day guide on what to expect.
Typical Wisdom Tooth Pain Recovery Timeline
| Day(s) | Expected Pain Level | Management Tips | Signs to Watch For |
|---|---|---|---|
| Day 1 | Moderate to High | Take prescribed pain relief, use ice packs (20 mins on, 20 off), rest, stick to liquids. | Excessive bleeding that won't stop with gauze pressure. |
| Days 2–3 | Moderate (Peak) | Continue pain relief and ice packs. Swelling will be at its peak. Stick to soft foods. | Worsening pain (not improving with medication), fever, pus, or a bad taste. |
| Days 4–5 | Mild to Moderate | Swelling should start to go down. You may be able to switch to over-the-counter pain relief. | Any signs of a dry socket: severe, radiating pain that doesn't respond to medication. |
| Days 6–7 | Mild | Most soreness and swelling should be significantly reduced. Jaw stiffness might remain. | Any new or worsening symptoms. |
This timeline should help you track your progress. By the end of the first week, you should be feeling much more like yourself.
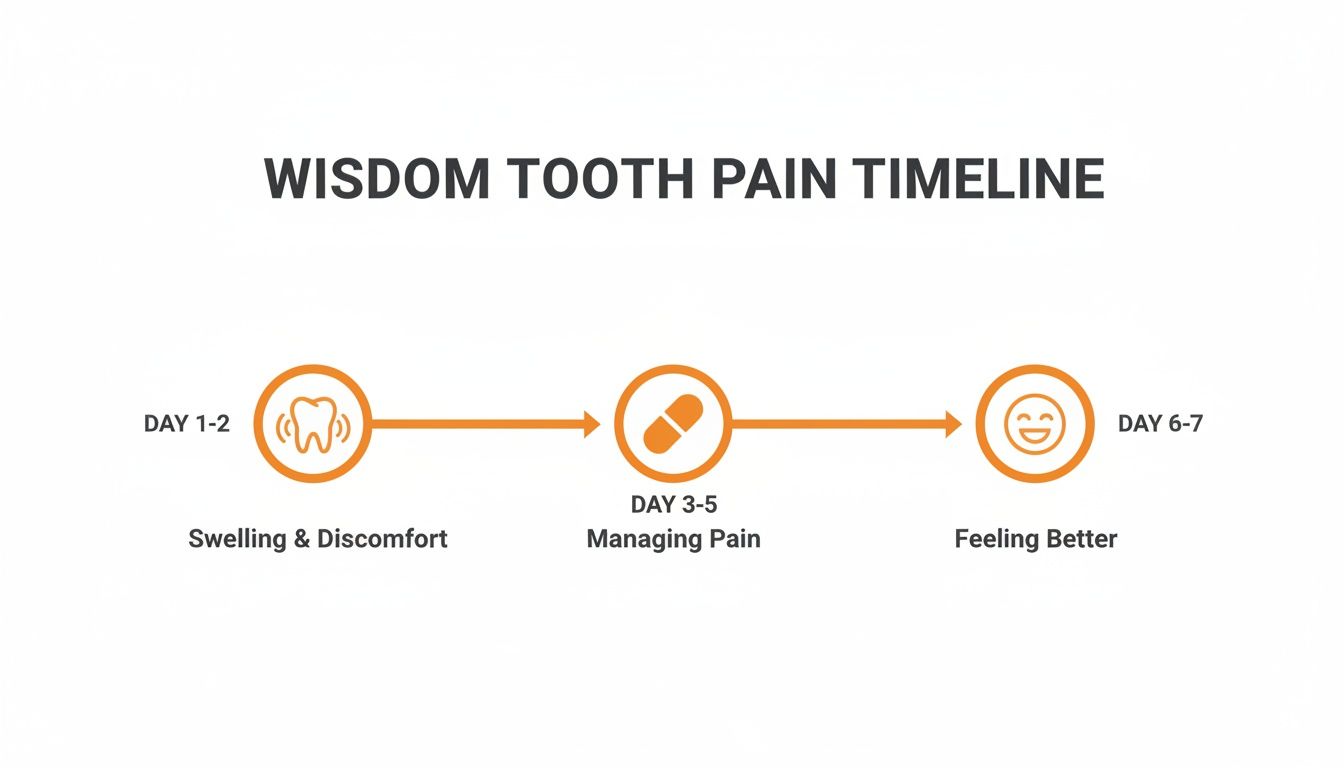
As you can see, the first few days are all about managing swelling, followed by a focus on pain relief. By understanding this natural progression, you can confidently tell the difference between normal healing and something that might need a follow-up call. If you ever experience an urgent issue, you can learn more about how our team provides emergency dental care.
Navigating the First 72 Hours of Recovery

The first three days after your wisdom tooth removal are the most important for a smooth and comfortable recovery. This is the period where swelling and discomfort tend to peak, but with a clear plan, you can manage this phase confidently and get on the road to healing.
Think of these first 72 hours as laying the groundwork for your entire recovery. The steps you take now have a direct impact on how quickly you feel better and can help you avoid complications down the track.
Your Immediate Post-Op Care Plan
Once you’re home, the focus is on two key things: managing discomfort and protecting the extraction site. Your body gets to work right away, forming a crucial blood clot in the empty socket. This clot is like a natural bandage, protecting the bone and nerves underneath.
Your main job is to do everything you can to keep that clot safe and sound. If it gets dislodged, it can lead to a painful condition called dry socket, which will set your healing back.
The first 24 hours are all about rest and keeping things stable. Prioritise keeping your head elevated, even when you sleep, and give your body the best chance to focus its energy on healing.
To manage the initial wisdom tooth removal pain and swelling, here’s what to do straight away:
- Rest Completely: Avoid any strenuous activity, bending, or heavy lifting. Now is the time to take it easy.
- Keep Your Head Up: Use a few extra pillows to prop your head up. This simple trick helps lower blood pressure at the extraction site, which means less bleeding and swelling.
- Manage Bleeding: Gently bite down on the gauze pads we provided. You can change them as directed, usually every 30-60 minutes, until the bleeding eases up.
How to Control Pain and Swelling
Swelling and discomfort are a normal part of your body’s healing response, usually peaking around the second or third day. The secret is to stay ahead of the pain, rather than trying to play catch-up once it’s become intense.
Make Ice Packs Your Best Friend
For the first 48 hours, cold therapy is your go-to. Applying an ice pack to the outside of your jaw helps constrict the blood vessels, which reduces both swelling and that throbbing ache.
A good rhythm to follow is 20 minutes on, then 20 minutes off. This cycle is much more effective than leaving it on for long periods.
Time Your Pain Medication
We will give you a clear plan for pain management, which might involve prescription medication or a schedule for over-the-counter options like ibuprofen and paracetamol. For more specific advice on certain medications, you might find our guide on using Panadeine Forte after a tooth extraction helpful.
The most important tip is to take your first dose of pain relief before the local anaesthetic completely wears off. This proactive step helps you stay on top of the discomfort right from the start.
The "Don'ts" of Early Recovery
Protecting that blood clot is absolutely non-negotiable. Certain actions create suction or pressure in your mouth that can easily dislodge it. For at least the first 72 hours, you must avoid:
- Using Straws: The suction from drinking through a straw is a common culprit for dry socket. It’s much safer to drink directly from a glass.
- Smoking or Vaping: This is a major no. The sucking motion can dislodge the clot, while the chemicals in smoke seriously interfere with your body's healing process and increase the risk of infection.
- Vigorous Rinsing or Spitting: Forcefully swishing or spitting creates pressure that can disturb the healing site. For the first 24 hours, gently let water or saliva dribble out of your mouth instead of spitting.
- Drinking Hot Liquids: Stick to cool or lukewarm drinks. Hot coffee, tea, or soup can increase blood flow to the area and may dissolve the blood clot.
By carefully following these steps, you can navigate the most uncomfortable part of recovery with confidence and create the perfect environment for your body to heal.
Your At-Home Pain Management Toolkit

Once you’re through the first 72 hours, the game changes. You’ve made it past the peak, and now the focus shifts from managing acute pain to supporting your body’s natural healing process. This is all about looking after the extraction site, eating well, and managing any lingering discomfort.
The good news? With the right care at home, the hardest part is likely behind you. In fact, data from the NSW Health Department’s 2026 Dental Pain Audit shows that while 62% of patients in Sydney’s Inner West report moderate to severe pain in the first 48 hours, this number plummets to under 10% by day 7 when proper aftercare is followed. It just goes to show how much of a difference a good home care routine makes.
Hot and Cold Therapy for Comfort
For the first couple of days, ice packs are your best friend for keeping swelling down. But after about 72 hours, it's time to switch tactics.
This is when a warm compress takes over. Applying a warm, moist cloth to the outside of your jaw helps soothe any leftover stiffness and tension. The warmth increases blood flow, which not only feels great but also helps speed up healing.
Medication and Gentle Rinsing
It's important to continue being smart about your medication. By now, you might feel comfortable enough to move from prescription painkillers to over-the-counter options.
A really effective approach is to alternate between an anti-inflammatory like ibuprofen (which tackles the swelling) and a pain reliever like paracetamol. This combination provides consistent, round-the-clock relief without needing stronger medication. Just be sure to always follow the dosage instructions on the packet or the advice we gave you.
After the first 24 hours, you can start gentle salt water rinses. This is a crucial step for keeping the socket clean and preventing infection, all without disturbing that important blood clot.
Simply mix half a teaspoon of salt into a glass of warm water. Let the solution gently flow over the area after you eat. Don’t swish or spit forcefully—just tilt your head side to side, then let the water fall out of your mouth and into the sink.
Nourishing Your Body for Faster Healing
What you eat plays a massive part in your recovery. Your body is working hard to heal, and it needs the right fuel. At this stage, you can start to expand your menu beyond just liquids to soft, nutritious foods that don't require much chewing.
A balanced soft-food diet will keep you feeling full and provide the essential vitamins and minerals needed for tissue repair. Think about adding these to your menu:
- Nutrient-Dense Soups: Creamy vegetable soups are perfect, but make sure they’re served lukewarm, not hot.
- Soft Scrambled Eggs: A fantastic source of protein that helps your body rebuild.
- Yogurt and Smoothies: Easy to get down and packed with nutrients. Just remember—no straws!
- Mashed Potatoes or Sweet Potatoes: Classic comfort food that’s gentle on a tender mouth.
- Oatmeal or Porridge: A warm and soothing breakfast that’s easy to swallow.
What you avoid is just as important. Stay away from anything crunchy or hard like crisps, nuts, and seeds, as they can easily get stuck in the socket and cause problems. Spicy or acidic foods can also irritate the area, so it's best to give them a miss for the first week or so. It’s also wise to protect your teeth from grinding, especially during recovery; you can learn more about how a dentist-fitted mouth guard helps protect teeth in all sorts of situations.
Recognising Complications Like Dry Socket

While the vast majority of wisdom tooth removals are straightforward, knowing how to spot a complication is the best way to ensure your recovery stays on track. Your healing should be a story of steady improvement, so it’s important to know what isn't normal so you can act fast.
The most common hurdle people face after an extraction is a condition called alveolar osteitis, though you’ve probably heard it called a dry socket. It’s the main reason for severe post-operative pain and can really set your recovery back.
Understanding what a dry socket is and why it happens is the first step to avoiding it altogether.
What Is a Dry Socket?
Think of the extraction site like a small wound. After we remove a tooth, your body naturally forms a blood clot over the empty socket. This clot is nature’s perfect bandage—it protects the underlying bone and nerves and kicks off the healing process.
A dry socket happens when that vital blood clot gets dislodged, dissolves too soon, or doesn't form properly in the first place. Without its protective cover, the sensitive bone and nerve endings are left exposed to air, food, and bacteria. This direct exposure is what causes the intense, throbbing pain that’s the tell-tale sign of the condition.
In Australia, dry socket happens in about 15-25% of wisdom tooth extractions. It’s also much more common in the lower jaw, with some studies showing it occurs up to 10 times more frequently in lower wisdom teeth sockets than upper ones. At The Smile Spot, our gentle techniques are specifically designed to minimise this risk.
Key Symptoms of a Dry Socket
One of the trickiest things about a dry socket is that it doesn't show up immediately. You might feel like you're recovering perfectly for a few days, only for the pain to suddenly get much worse. This isn’t the normal ache of healing; it’s something different.
A key sign of a dry socket is a sudden worsening of pain around day three to five after your procedure. This isn't just discomfort; it's often a severe, radiating pain that over-the-counter medication can't touch.
If you’re worried, keep an eye out for these specific signs:
- Intense, Throbbing Pain: This is a severe, deep ache that can radiate from the socket up towards your ear, eye, or temple on the same side of your face.
- Visible Empty Socket: If you look at the extraction site in a mirror, you might see whitish-looking bone instead of a dark blood clot. The socket may look empty and dry.
- Bad Breath or Unpleasant Taste: A foul taste in your mouth or persistent bad breath that doesn’t go away with gentle rinsing can be a red flag.
- No Relief from Painkillers: The pain from a dry socket is notoriously stubborn and often doesn’t respond to standard pain relief medication.
Other Complications to Watch For
While dry socket is the most common issue, it's also important to know the signs of an infection. An infection will also increase your pain levels and requires immediate attention from your dentist.
Signs of an infection can include:
- Fever or chills
- Pus or a yellowish discharge from the socket
- Swelling that gets worse after the third day
- Persistent bleeding that doesn’t stop with pressure
The most important thing to remember is this: do not try to 'tough it out'. Our team is here to help. If you suspect a dry socket, an infection, or anything else that doesn't feel right, getting in touch with us is the fastest way to get relief and put your recovery back on track.
If you believe you’re experiencing a dental emergency, seeking immediate help is the best thing to do. You can learn more about when to seek urgent care from an emergency dentist on our services page.
How Gentle Dentistry Minimises Pain from the Start
When it comes to managing wisdom tooth removal pain, the best approach is to prevent it from happening in the first place. This is where a modern, patient-focused approach to dentistry truly shines. Rather than just focusing on pain relief after the fact, gentle dentistry is about minimising the initial trauma that causes the pain.
A less traumatic procedure leads directly to a less painful recovery. By focusing on precision and careful technique from the very start, we can significantly reduce tissue damage. This means less swelling, less bleeding, and a much smoother healing journey for you.
Minimally Invasive Procedures and Advanced Technology
Traditional extractions could sometimes involve a lot of force, which is tough on the surrounding gum and jawbone. A modern, minimally invasive approach flips this script entirely. Think of it as using a fine surgical instrument instead of a heavy tool—both get the job done, but one is far more precise and causes much less collateral damage.
This precision comes from careful planning and the right technology. By getting a crystal-clear picture of your tooth’s position and root structure before we even begin, we can plan the most efficient and gentle way to remove it, often avoiding the need for more aggressive techniques.
The core principle of gentle dentistry is simple: the less we disturb the surrounding tissues during your procedure, the less work your body has to do to heal afterwards. This means a faster, more comfortable recovery.
One of the key tools that helps us achieve this is laser dentistry.
The Impact of Biolase Laser Dentistry
At The Smile Spot, we use leading-edge technology like the Biolase water laser to redefine the extraction experience. This advanced tool can often replace the traditional scalpel and drill, offering a wealth of benefits that directly impact your comfort and recovery.
The Biolase laser uses a unique combination of water and light energy to perform incredibly precise incisions. Here’s how it helps minimise pain and swelling:
- Less Bleeding: The laser energy naturally cauterises blood vessels as it works. This creates a cleaner surgical site with significantly less bleeding, both during and after the procedure.
- Reduced Swelling: Because the laser is so precise and generates minimal heat, there is far less trauma to the surrounding gum and bone. This dramatically reduces the body's inflammatory response, which is what causes post-operative swelling.
- Faster Healing: The laser also promotes healing at a cellular level—a process known as photobiomodulation. This helps kickstart your body’s natural repair mechanisms for a quicker, smoother recovery.
Using a laser allows us to be gentler and more accurate, preserving healthy tissue and making the entire process easier on your body from start to finish.
The Role of Experience and Gentle Technique
Technology is a powerful ally, but it’s most effective in the hands of an experienced and caring dentist. A surgeon’s gentle technique is perhaps the single most important factor in ensuring a comfortable procedure and an easy recovery.
An experienced dentist understands the nuances of each unique extraction. They know how to work with the body, not against it, using skill and finesse rather than just force. This careful handling of tissue is critical for preventing unnecessary trauma, which in turn reduces post-operative wisdom tooth removal pain.
This gentle touch, combined with years of experience, ensures your procedure is as quick and smooth as possible. It’s this blend of skill and compassion that truly defines our patient-first approach.
Sedation Dentistry for a Calm Experience
Feeling anxious about a dental procedure is incredibly common. Unfortunately, stress and tension can make the experience feel more uncomfortable, as your body becomes more sensitive to pain when it's in "fight or flight" mode.
This is where sedation dentistry plays a vital role. By helping you reach a state of deep relaxation, we can break the cycle of anxiety and pain. Being calm during the procedure not only makes it a stress-free experience but also contributes to a better recovery, as a relaxed body is better able to heal.
To understand the different levels of sedation available and how they can create a calm experience, you can read our detailed guide on the benefits of seeing a dentist who offers full anaesthesia options.
By tackling pain and anxiety from every angle—with advanced technology, experienced technique, and options for sedation—we design a wisdom tooth removal experience that is built around your comfort from the very start.
Frequently Asked Questions About Wisdom Tooth Pain
Even with a comprehensive guide, we know you probably still have a few questions swirling in your mind. That’s completely normal. Here are some quick, straightforward answers to the most common queries we get from our patients about wisdom tooth removal.
How Long Will the Worst Pain Last?
The toughest part is usually over quite quickly. Most of the noticeable pain and swelling peaks within the first 48 to 72 hours after your procedure. From about day four or five, things should start to feel much more comfortable.
If you stick to your aftercare instructions—taking your medication on time, using ice, and getting plenty of rest—you’ll get through this initial period smoothly. By the end of the first week, most people only feel a bit of mild, manageable tenderness.
Can I Avoid Taking Strong Prescription Painkillers?
Yes, definitely. Many of our patients find they can manage perfectly well by alternating over-the-counter medications like ibuprofen and paracetamol. This combination approach is excellent for tackling both the pain and the inflammation at the same time.
Your dentist will talk through the best pain relief plan for your specific situation. Our priority is making sure you’re comfortable, and we generally only suggest prescription medications for more complex extractions.
My Jaw Is Really Stiff—Is This Normal?
Yes, a stiff jaw is a very common and expected side effect. It’s a condition known as trismus, and it’s simply caused by the jaw muscles swelling up after the surgery. You'll notice it most in the first few days.
Don’t worry, it will get better. After the first 48 hours have passed, you can start applying a warm, moist cloth to the side of your face to help those muscles relax. Gently opening and closing your mouth a little throughout the day will also help you get your full range of movement back sooner.
How Long Do I Really Have to Wait to Smoke?
This is a really important one. It's crucial to avoid smoking for as long as you possibly can. We advise a bare minimum of 72 hours, but a full week is much, much better for your healing.
The sucking motion can easily dislodge the blood clot that forms in the socket, leading to an incredibly painful complication called dry socket. On top of that, the chemicals in smoke slow down your body’s natural healing process and seriously increase your risk of infection. For a smoother recovery with less pain, we strongly urge you to wait. And remember, if you have any worries during your recovery, our team is just a phone call away. You can also learn about our gentle checkup and clean services, where we prioritise your comfort every step of the way.
Your Path to a Smooth and Comfortable Recovery
Getting your wisdom teeth removed is a big step, but you’re now equipped with the right knowledge to make your recovery as smooth as possible. While some post-procedure discomfort is a normal part of healing, it’s temporary and, most importantly, manageable.
Your main goal is to protect the extraction site. Diligent home care, especially in the first 72 hours, is what sets the stage for a quick recovery. This means taking your pain medication as directed to stay ahead of the discomfort, rather than waiting for it to build up.
Your Key Steps for Success
Gentle oral hygiene is also crucial for preventing infection. After 24 hours, you can start using warm salt water rinses to keep the area clean without disturbing the healing process. Pairing this with a temporary diet of soft, nutritious foods gives your body the fuel it needs to repair itself efficiently.
Knowing what to look for is half the battle. By recognising the early signs of a complication like a dry socket, you’ll know to contact us right away and avoid unnecessary pain. This guide is all about putting you in control and turning any anxiety into confidence. Of course, good oral hygiene is always important; you can learn more about our gentle checkup and clean services where we always prioritise your comfort.
A smooth recovery isn’t about luck—it’s about following a simple, clear plan. When you take an active role in your own aftercare, you help ensure your healing is as quick and comfortable as it can be.
Don't let worries about wisdom teeth hold you back. The team at The Smile Spot is here to guide you every step of the way, from your first chat to your final check-up. If you live in Dulwich Hill or the Inner West, we invite you to book a consultation to discuss your needs and learn about our gentle, pain-managed approach to extractions. Contact us today!