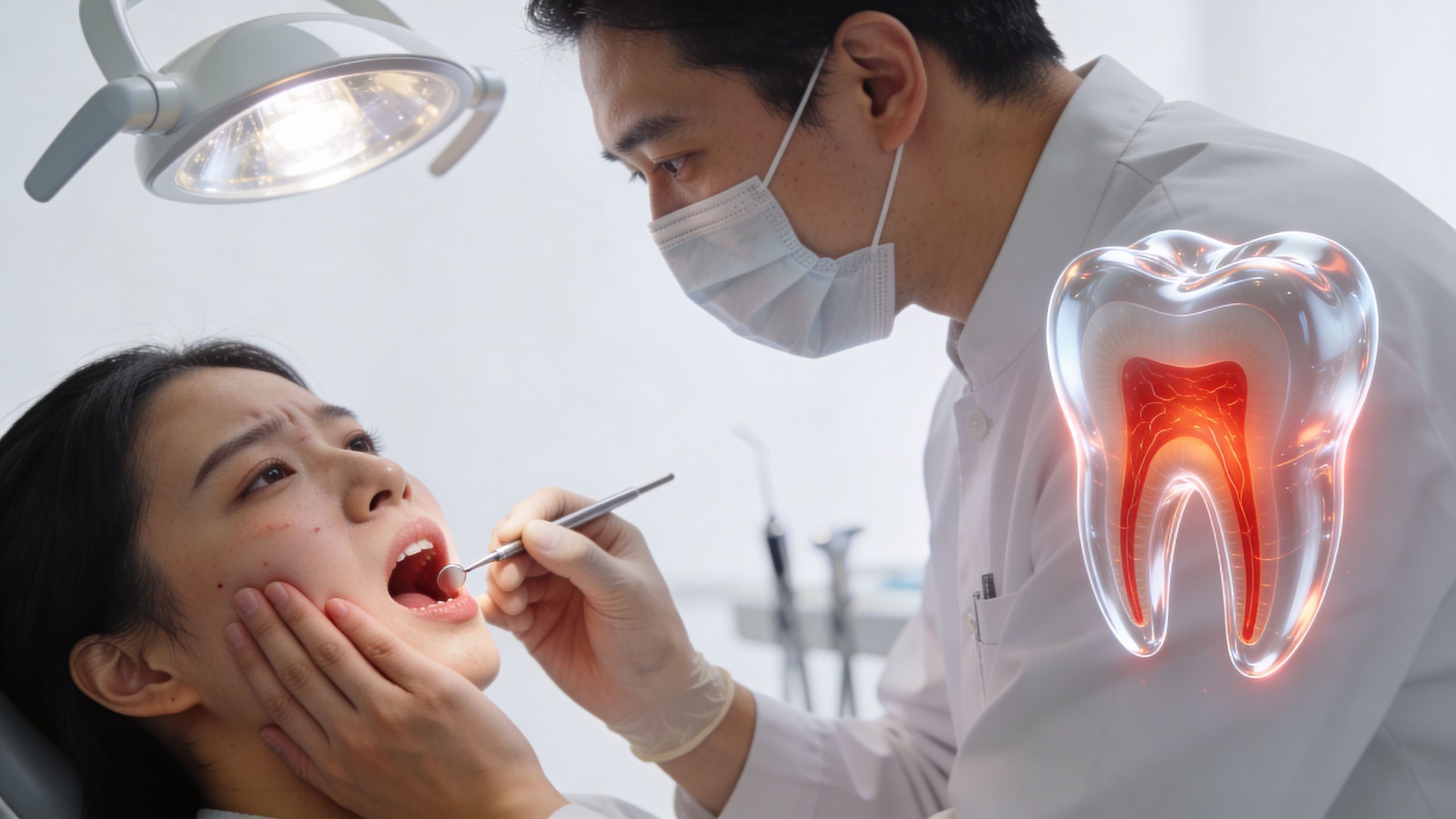
It often starts in an ordinary moment. You take a sip of coffee, bite into toast, or chew on one side, and one tooth answers back. Then the pain settles, and it is easy to hope it was nothing.
Intermittent symptoms are one reason people delay treatment. In practice, that stop-start pattern can still point to a deeper problem inside the tooth. An irritated or infected pulp does not always cause constant pain. Early signs can be subtle. A tooth may feel tender, unusually sensitive, or “off” for a few days before it becomes harder to ignore.
A root canal is designed to save that tooth. The treatment removes infected or inflamed tissue from inside the tooth, disinfects the canal space, and seals it so the tooth can stay in function. For many patients, this is the most conservative way to get rid of pain and avoid an extraction.
Patients are often relieved to learn how manageable the process is.
At The Smile Spot, the path is straightforward. We start by identifying the source of the pain, confirming whether the nerve is involved, and discussing the best option for the tooth. If a root canal is the right treatment, modern techniques, including Biolase technology and sedation options where appropriate, can make care far more comfortable than people expect. The final step is restoring the tooth properly so you can chew with confidence again.
If you are trying to sort out whether your discomfort sounds like nerve pain or general relief for sensitive teeth, context helps, but it should not replace an exam. If you are already relying on stronger pain relief while waiting for care, our guide to Panadeine Forte for tooth extraction pain and what to know before taking it explains a few practical points.
The signs below are the ones dentists take seriously. Some are obvious. Others are easy to miss until the problem has progressed.
1. Severe Tooth Pain When Chewing or Biting
A tooth that hurts when you bite down is one of the clearest warning signs. It’s different from general sensitivity. You can usually point to one tooth, one side, or one exact spot that flares when pressure lands on it.
That matters because the nerve inside the tooth can become inflamed after deep decay, a crack, trauma, or even a large filling that no longer seals properly. Patients often describe it as a sharp jab when they bite into an apple, followed by an ache that hangs around after they stop chewing.

What this pain often feels like
Sometimes the pain is immediate and strong. Sometimes it’s more deceptive. You chew normally for most of the meal, then one particular bite sends pain through the tooth and into the jaw.
A common real-life example is the patient who had a large filling or crown placed months ago and thought everything was fine. Then chewing starts to feel tender again, especially on hard food like nuts, crusty bread, or muesli bars. That pattern deserves attention because pressure pain can mean the pulp has become irritated beyond what a simple adjustment will fix.
Practical rule: If you’re avoiding one side of your mouth because a single tooth hurts under pressure, don’t assume it will settle on its own.
There’s also a trade-off here. Resting the tooth may reduce pain for a day or two, but it won’t remove infection if the nerve is already compromised. Pain tablets can make things more tolerable temporarily, but they can also mask worsening symptoms. If you’ve been relying on medication, it’s worth reading about Panadeine Forte after dental treatment so you understand where pain relief helps and where it doesn’t replace care.
What helps while you wait for an appointment
A few simple steps can stop you aggravating the area further:
- Chew on the other side: Give the sore tooth a break until it’s assessed.
- Notice the trigger: Hard foods, seeded bread, and chewy meats often expose pressure pain fastest.
- Use pain relief carefully: Over-the-counter medication may reduce discomfort, but it won’t solve the cause.
- Book promptly: Early diagnosis usually gives you more treatment options.
If you’re trying to judge whether this is “just sensitivity” or something deeper, this overview of relief for sensitive teeth when biting down can help you compare symptoms. But if the pain is localised, repeatable, and tied to biting pressure, dentists start thinking about the pulp, not just the enamel.
2. Prolonged Sensitivity to Hot and Cold Temperatures
You take a sip of coffee, and one tooth keeps aching after the mug is back on the table. Or cold water sets off a sharp response that lingers longer than it should. That pattern deserves attention because timing matters. Brief sensitivity often points to exposed dentine or enamel wear. Pain that hangs on after the trigger is gone raises more concern about the pulp inside the tooth.
In practice, this is one of the clearest differences patients can notice at home. A quick zing that stops straight away can come from gum recession, whitening products, a worn area near the gumline, or a recently cleaned tooth. Lingering pain suggests the nerve is inflamed and struggling to recover.
A common example is a tooth that had a filling weeks ago and still reacts every time cold touches it. Another is a back tooth that feels fine most of the day, then flares with soup, tea, or ice cream and stays sore for several minutes. If the sensation is becoming deeper, sharper, or easier to trigger, the problem may be moving beyond ordinary sensitivity.
Surface sensitivity and nerve pain can feel similar at first. The difference is what happens next. Surface sensitivity settles quickly. Nerve-related pain tends to linger, recur, and gradually interfere with normal eating and drinking.
What to do before it gets worse
A few practical steps can reduce irritation while you arrange an assessment:
- Brush with a soft brush: Heavy brushing can worsen exposed areas near the gumline.
- Reduce acids for now: Soft drinks, citrus, and sports drinks can aggravate already sensitive teeth.
- Use desensitising toothpaste for a short trial: If there is no clear improvement, the tooth needs testing rather than more guesswork.
- Notice recent changes: Whitening, a new filling, clenching, or a cracked cusp can all change how a tooth responds to temperature.
Cosmetic products can confuse the picture. Whitening treatments often cause temporary sensitivity, but they should not create lingering pain in one specific tooth. If you have been using whitening products recently, it helps to understand the difference between expected short-term sensitivity and a deeper problem. Our guide to professional teeth whitening options explains what is normal and what deserves a dental review.
Many patients delay care because they assume a root canal will be painful. The usual reality is the opposite. The aim of treatment is to remove the inflamed or infected tissue, settle the pain, and keep the tooth. At The Smile Spot, we can confirm the cause with proper testing, then talk through the least invasive next step. Some teeth need monitoring, a filling, or bite adjustment. If the pulp is beyond recovery, root canal treatment can often be completed comfortably with sedation options and Biolase-assisted care, followed by full restoration of the tooth.
If hot or cold sets off pain that lingers after the sip or spoonful, book an examination promptly. Earlier diagnosis usually means a clearer plan and a better chance of saving the tooth before the problem becomes more complicated.
3. Tooth Discolouration or Darkening
A tooth that slowly turns grey, brown, or noticeably darker than the teeth around it deserves attention, even if it doesn’t hurt much. Surface stains from coffee, tea, or red wine usually affect multiple teeth and sit on the outside. A single tooth changing colour can point to internal damage.
This often happens after trauma. A child bumps a front tooth during sport. An adult chips a tooth in a fall and forgets about it because the pain settles. Months later, that tooth looks duller or darker than the others. In many cases, that change means the pulp inside has been damaged or has died.
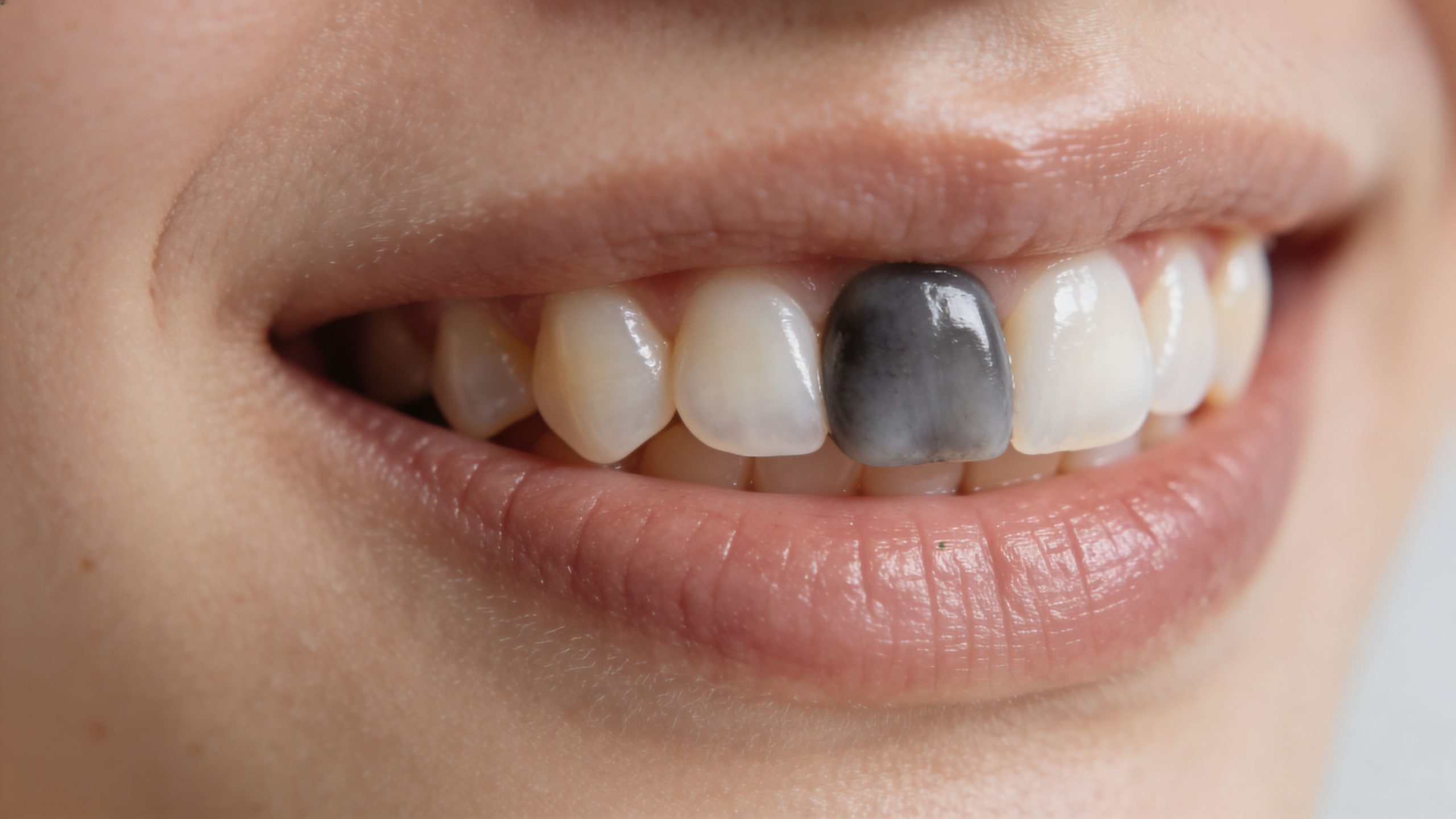
Why whitening usually doesn’t fix this
People often lose time in this situation. They assume the problem is cosmetic and try whitening toothpaste, strips, or a whitening treatment. If the darkening comes from inside the tooth, whitening the enamel alone won’t solve it.
The right sequence is diagnosis first, then appearance. If the nerve has died or become infected, the internal problem must be treated before cosmetic work. Once the tooth is healthy and sealed, you can look at options to improve colour and appearance.
A common scenario in practice is a front tooth that darkens long after a childhood accident. The patient isn’t in severe pain, so they delay. But a dark tooth can be a silent warning sign, not just a cosmetic nuisance.
A tooth can need treatment even when it isn’t screaming at you. Colour change is one of the quieter signs.
What usually works better than waiting
When a tooth darkens, the useful details are its timing and history. Did it happen after trauma? After a deep filling? After an old dental procedure?
Bring that timeline to your appointment. It helps the dentist work out whether the issue is likely internal staining, pulp death, previous trauma, or something more superficial. If treatment is needed, the next step after root canal therapy is often a protective or cosmetic restoration. People who first look into professional teeth whitening are sometimes surprised to learn the darker tooth may need endodontic care before any whitening plan makes sense.
Waiting doesn’t usually improve a darkening tooth. It only delays the answer.
4. Persistent or Recurring Pimple-Like Bump on the Gums
A small bump on the gum that keeps appearing in the same place is one of the classic signs dentists watch for. Patients often call it a pimple, blister, or little boil. It may be tender, or it may not hurt much at all.
What makes it important is the pattern. It comes up near one tooth, sometimes drains, then seems to settle. That temporary release can trick people into thinking the problem has healed. It hasn’t. In many cases, the bump is a drainage point for infection linked to the tooth root.
Why this bump matters
When infection builds around the root, pressure needs somewhere to go. The body sometimes creates a small channel through the gum, which is why the bump may flatten after it leaks fluid and then return later.
That cycle doesn’t mean the tooth is recovering. It usually means the infection is still there. Australian dental reporting has noted that untreated cases can progress to abscess formation in a meaningful share of instances, which is one reason gum swelling and recurring drainage should never be brushed off as minor irritation.
A patient might notice the bump while flossing near an upper molar, or see a small white spot above a front tooth after an old injury. Others report a bad taste in the mouth that comes and goes. Those details matter because they point to an infection that may already be draining.
What not to do
The worst approach is trying to pop it yourself. That can push bacteria into surrounding tissue and make the area more inflamed.
Instead:
- Keep the area clean: Brush gently and don’t skip flossing around nearby teeth unless instructed otherwise.
- Use warm saltwater rinses: This may soothe the area, but it won’t eliminate the infection.
- Arrange urgent dental care: If the bump is recurring, the cause needs diagnosis.
- Watch for spread: Increasing swelling, fever, or feeling unwell raises the urgency.
A recurring gum pimple is one of those signs you need a root canal that patients often underestimate because the pain isn’t always severe. But a draining abscess is still an abscess. The right response is to treat the source, not just the symptom.
5. Swelling of the Face, Jaw, or Lymph Nodes
A patient may start the day with a sore tooth and end it with visible swelling along the cheek or jaw. That change matters. It often means the infection has spread beyond the tooth and is now irritating the surrounding tissues.
Swelling can show up in a few different ways. One side of the face may look puffy. The jaw may feel tender or tight. Some patients notice sore glands under the jaw or near the angle of the neck, especially when swallowing or turning the head. If opening wide becomes painful, the infection may be causing deeper inflammation.
When swelling becomes urgent
Facial swelling linked to tooth pain needs prompt assessment. If the swelling is increasing, you have a fever, you feel generally unwell, or swallowing is difficult, seek urgent care the same day.
I tell patients not to judge the problem by pain alone. A tooth can stop throbbing and still be infected. In some cases, pressure has found a path into nearby tissue.
What to do now
Home care has a limited role here. Saltwater rinses may keep the mouth cleaner, and appropriate pain relief may help while you arrange treatment, but neither fixes the source of infection.
A better plan is:
- Book an urgent dental assessment: The goal is to identify whether the tooth can still be saved and whether the swelling is coming from that tooth.
- Avoid pressing, rubbing, or heating the area: That often makes soreness worse.
- Take medication only as directed: Leftover antibiotics are a poor substitute for diagnosis and can delay the right treatment.
- Follow through with full restoration: If the tooth is treatable, root canal therapy removes the infected pulp, and the tooth is then protected with the right restoration, often a dental crown after root canal treatment.
This is also where the patient journey becomes clearer. First, we confirm the source with an exam and imaging. Then we focus on getting you comfortable. At The Smile Spot, that may include sedation options and Biolase-assisted care where appropriate, followed by restoring the tooth properly so you can chew with confidence again.
Swelling does not automatically mean the tooth cannot be saved. It does mean the decision should be made quickly. The earlier the source is treated, the better the chance of settling the infection and keeping the tooth.
6. A Cracked or Chipped Tooth Causing Persistent Pain
A crack changes the rules. Some cracks are superficial and mostly cosmetic. Others create a pathway for bacteria to reach the pulp, and that’s when a simple chip can turn into a root canal problem.
Australian data has highlighted cracked molars as a major reason people end up needing treatment, including teeth that had little or no pain at first and then progressed to pulpitis over time. That delayed pattern is exactly why cracked teeth get missed. The patient thinks, “If it was serious, it would hurt constantly.” That isn’t always how cracks behave.
The pain pattern that makes dentists suspicious
Cracked tooth pain is often inconsistent. You bite and feel nothing. Then the next bite, especially on something firm, sends a sudden pain through the tooth. Some people feel it more when releasing pressure than when biting down.
That’s because the crack can flex microscopically. As it moves, it irritates the nerve or surrounding structures. A front tooth chip can also trigger temperature pain if the damage exposes deeper layers of the tooth. A back molar with a fine crack may be harder to see, which is why imaging and clinical testing matter.
One practical example is the patient who bit on an olive pit or ice and noticed a sharp pain afterward. Another is the grinder who wakes with soreness in one molar and assumes it’s sinus pressure or general jaw tension.
Saving the tooth usually means protecting it
The first step is reducing stress on the damaged tooth. Avoid hard foods, don’t chew ice, and stop testing it with your tongue or by repeatedly biting to “see if it still hurts”.
If the crack has reached the pulp, root canal therapy may be the best way to save the tooth. After that, strength matters. A treated back tooth often needs coverage to reduce the risk of splitting further. That’s why many patients move from root canal therapy to a crown, and it helps to understand how dental crowns and bridges protect weakened teeth.
Cracks are a good example of what works versus what doesn’t. Waiting rarely seals a crack. Soft foods may reduce symptoms, but they don’t reverse structural damage. Diagnosis, then protection, is the path that gives the tooth the best chance.
7. Tooth Mobility or Looseness
An adult tooth that suddenly feels loose should never be ignored. Mild natural movement exists in all teeth, but if one tooth feels wobbly, changes position slightly, or moves more than the teeth around it, something is wrong.
Sometimes gum disease is the main cause. Sometimes an infection from the tooth itself has started affecting the structures that support it. When mobility appears alongside pain, swelling, or a history of untreated tooth problems, the tooth needs urgent assessment.
Why looseness can be a late sign
By the time a tooth feels mobile, the issue may have moved beyond the pulp alone. Infection or inflammation can affect the ligament around the root and the bone supporting it. That doesn’t automatically mean the tooth can’t be saved, but timing becomes much more important.
A typical scenario is the person who’s had on-and-off discomfort for months, then notices a front tooth shifting when biting into a sandwich. Another is a molar that feels tender and unstable after a longstanding crack or deep decay.
This is also where honesty helps. Tell your dentist how long the tooth has been loose, whether the movement is worsening, and whether you’ve avoided chewing on it. Those details influence whether root canal therapy, splinting, periodontal treatment, or extraction is the realistic option.
What to do right away
Don’t keep wiggling the tooth to check it. That adds trauma to an already compromised area.
Use these basics instead:
- Get seen promptly: Mobility narrows your treatment window.
- Be gentle with cleaning: Plaque control still matters, but rough brushing won’t help.
- Avoid biting on the tooth: Cut food smaller and use the other side.
- Ask about the full plan: Saving the tooth may involve endodontic treatment and later restoration.
If the tooth can’t be predictably saved, replacement planning matters. Patients facing that possibility often want to understand the longer-term options, including implants and full-arch solutions. These dental implant case studies can help you see what tooth replacement may look like if extraction becomes necessary.
A loose tooth doesn’t always mean you need a root canal. But it is one of the more serious signs you need a root canal assessment urgently, because the cost of waiting can be the tooth itself.
7 Signs You Need a Root Canal, Quick Comparison
| Symptom | Diagnosis Complexity 🔄 | Resource Requirements ⚡ | Expected Outcome ⭐ | When to Seek Care / Tip 💡 |
|---|---|---|---|---|
| Severe Tooth Pain When Chewing or Biting | Moderate, clinical exam, percussion/bite tests, X‑ray | X‑ray, clinical tests; possible endodontic treatment | ⭐⭐⭐, high chance to save tooth if treated promptly | See dentist promptly; avoid chewing on affected side; temporary analgesics |
| Prolonged Sensitivity to Hot and Cold Temperatures | Low–Moderate, thermal and vitality testing | Clinical exam, thermal tests, trial of desensitizing toothpaste; X‑ray if persistent | ⭐⭐, may resolve with conservative care; root canal if pulp necrosis | Try desensitizing toothpaste 2 weeks; consult dentist if symptoms persist |
| Tooth Discolouration or Darkening | Moderate, history, pulp testing, radiographs | X‑ray, vitality tests; likely root canal plus cosmetic restoration options | ⭐⭐⭐, good functional prognosis with root canal + restoration; aesthetics require additional work | Book evaluation; consider root canal then crown/veneer to restore appearance |
| Persistent or Recurring Pimple‑Like Bump on the Gums | Moderate–High, signs of localized abscess, drainage assessment | X‑ray, clinical exam, possible antibiotics, root canal or extraction; emergency appointment recommended | ⭐⭐, often savable with timely root canal; risk of spread if delayed | Do not squeeze; seek emergency dental care for drainage and definitive treatment |
| Swelling of the Face, Jaw, or Lymph Nodes | High, systemic involvement possible, urgent assessment needed | Urgent dental/medical exam, imaging, antibiotics, possible hospital referral | ⭐, outcome depends on rapid intervention; potential for serious complications | Seek immediate care (urgent/emergency) if swelling, fever, or difficulty swallowing |
| A Cracked or Chipped Tooth Causing Persistent Pain | Moderate, visual exam, bite test, X‑ray/CBCT if needed | X‑ray or CBCT, restorative work (crown), root canal if pulp exposed | ⭐⭐⭐, good if crack is treatable and treated early; poor if crack extends below root | Avoid chewing on tooth; see dentist quickly for assessment and restoration |
| Tooth Mobility or Looseness | High, indicates bone/periodontal involvement, specialist input often required | X‑ray, periodontal probing, possible endodontic or surgical treatment, replacement options | ⭐⭐, variable; early intervention may save tooth, advanced cases often need extraction | Seek urgent evaluation; avoid wiggling tooth; discuss preservation vs replacement options |
Your Next Steps to a Pain-Free Smile in Dulwich Hill
You bite down on lunch and feel that same sharp jolt again. The pain settles after a minute, so it is easy to tell yourself it can wait. That is how many root canal cases drift from manageable to urgent.
Catching these signs early gives you a better chance of keeping the tooth and avoiding a more complicated problem later. Root canal treatment is designed to remove infection, settle pain, and preserve your natural tooth. For many patients, it is the treatment that prevents extraction, not a last resort.
At The Smile Spot, the first step is diagnosis. We look at how the pain behaves, test the tooth, and use digital imaging to check the roots, surrounding bone, and tooth structure. A painful tooth does not always need a root canal, and a tooth with very little pain can still have a serious infection.
That distinction matters.
Some teeth are better treated with a filling, a crown, or monitoring over time. Some symptoms are linked to grinding, a cracked cusp, gum disease, or recent trauma rather than irreversible nerve damage. Good care means choosing the treatment that fits the diagnosis, not forcing every sore tooth into the same plan.
If a root canal is the right option, the process is straightforward. The infected or inflamed tissue inside the tooth is removed, the canals are cleaned and sealed, and the tooth is then restored so it can function properly again. At The Smile Spot, Biolase laser dentistry helps us treat teeth with a minimally invasive approach, and sedation is available for patients who feel anxious or have avoided care because of fear.
Root canal treatment relieves pain by removing the source of the infection.
The final stage matters too. Many teeth that need root canal treatment have already lost strength from decay, a crack, or a large filling. Restoring the tooth with a crown or another custom restoration helps protect it from fracture and lets you chew comfortably again while keeping your smile looking natural.
Delays are common. Patients often hope the pain will settle, or they manage it with tablets while work, school pickups, and day-to-day life take priority. Short-term pain relief may help you get through the day, and this complete acetaminophen and codeine guide explains that option, but medication does not remove an infection or repair a damaged tooth.
The Smile Spot cares for patients across Dulwich Hill and the Inner West, including Marrickville, Earlwood, and Ashfield. With late evening and Saturday appointments, treatment is easier to fit into real life. If these signs sound familiar, book an assessment before the problem gets worse. Early treatment is often the fastest way back to comfort, function, and peace of mind.
If you’re noticing signs you need a root canal, The Smile Spot can help you get clear answers and gentle treatment in Dulwich Hill. Dr. Dimitrios Thanos and the team offer thorough diagnosis, advanced Biolase laser dentistry, sedation options for anxious patients, and complete restoration after treatment, so you can move from pain and uncertainty to a healthy, functional smile.