If you’re reading this with a knot in your stomach, you’re not alone. A lot of people put off the dentist for months, sometimes years, because the thought of the chair, the sounds, the numb feeling, or not being in control feels overwhelming.
That avoidance can become a cycle. You delay a check-up because you’re anxious. A small problem gets bigger. Then the next visit feels even more intimidating because you expect more treatment, more time in the chair, and more stress.
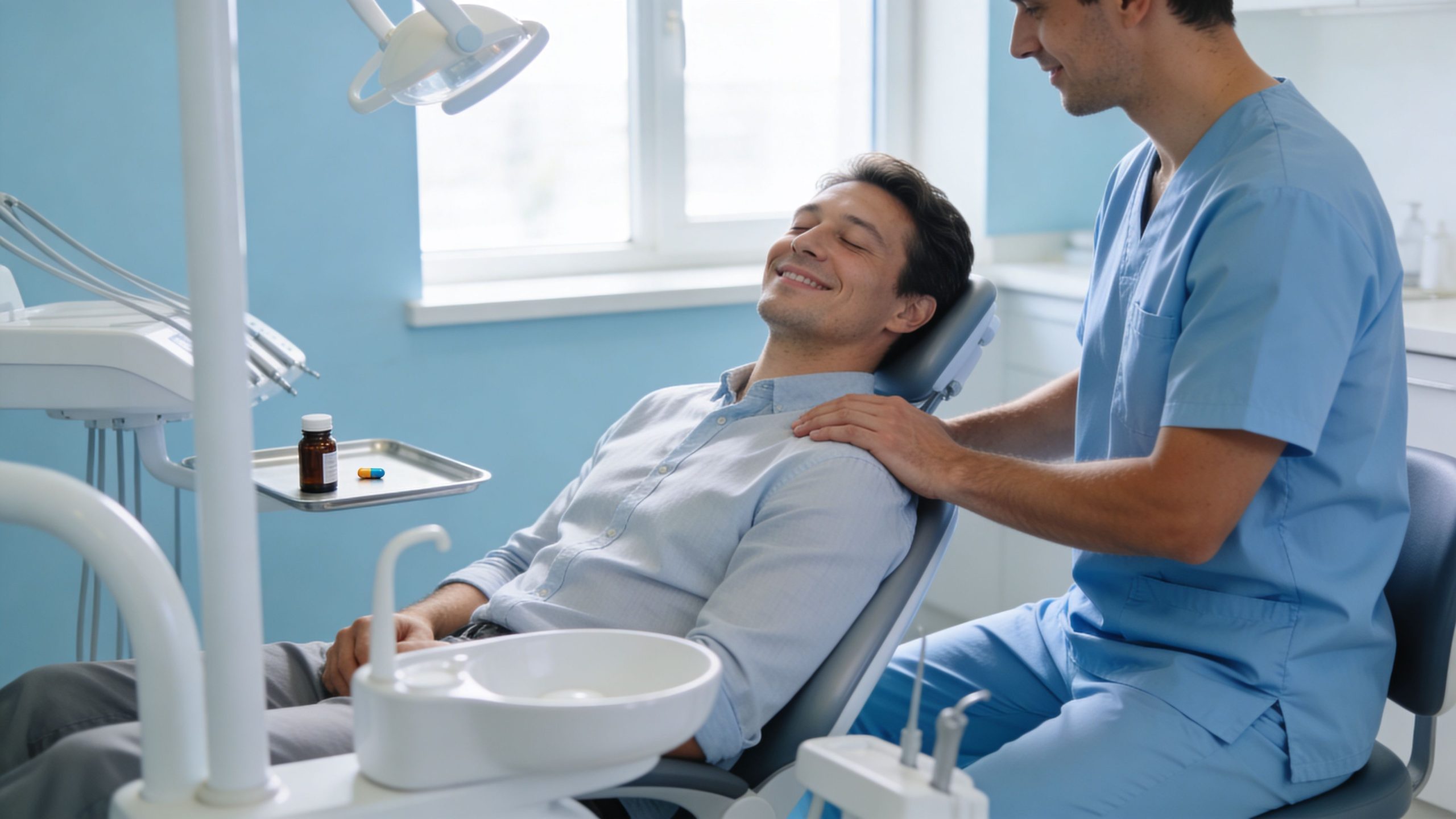
Oral sedation dentistry is designed to interrupt that cycle. It helps anxious patients feel calm enough to get the care they need, while staying awake and able to respond. For many people, it changes dentistry from something they dread into something they can manage.
Overcoming Dental Anxiety with Oral Sedation
A common story goes like this. Someone notices sensitivity, a broken filling, or a wisdom tooth that’s starting to flare up. They mean to book. Then they remember a bad experience, feel their chest tighten, and close the browser.
That reaction is more common than is generally understood. In Australia, approximately 40 to 50% of adults experience some level of dental fear, and 36% of Australians aged 15 and over have moderate to high dental anxiety, with prevalence higher in women (42%) than men (30%) according to Australian dental anxiety figures summarised here.

What oral sedation actually changes
Oral sedation dentistry doesn’t erase your personality or put you into a dramatic “sleep.” It reduces the intensity of the fear response so your body isn’t on high alert the whole time. It’s akin to turning the volume down on panic so you can get through treatment without feeling overwhelmed.
For anxious patients, that matters in very practical ways:
- Booking becomes possible because the appointment no longer feels impossible.
- Longer treatment feels more manageable because you’re more relaxed in the chair.
- You can stop the delay cycle before small issues become painful or expensive problems.
- Your memories of the visit may feel softer because the experience is less emotionally charged.
Anxiety is real, not “just nerves”
Many patients minimise what they’re feeling. They’ll say, “I know it sounds silly,” or “I should be able to handle it.” But dental anxiety isn’t a character flaw. It can be linked to past painful treatment, a strong gag reflex, fear of needles, embarrassment about oral health, sound sensitivity, or a general tendency toward anxiety.
Oral sedation can be the bridge between wanting care and being able to accept it.
It also helps to work on anxiety outside the dental setting. If your nervous system is often on edge, broader coping strategies can support you before and after treatment. This guide on how to reduce anxiety symptoms for lasting calm may be useful alongside dental support.
Why patients often feel relieved once they understand the option
People sometimes assume sedation is only for major surgery or extreme phobia. It isn’t. Oral sedation can be appropriate for everyday dental care if fear is the main barrier.
The biggest shift often happens during the first conversation. Once patients learn they can remain awake, be monitored carefully, and have a calmer experience, many stop seeing the dentist as something they have to “push through.” They start seeing treatment as something that can be adapted to them.
Understanding How Oral Sedation Dentistry Works
The simplest way to explain oral sedation dentistry is this. It turns down the volume on anxiety without switching off consciousness. You’re not under general anaesthetic. You’re awake, but much calmer, often drowsy, and far less reactive to the usual triggers.
That distinction matters because many anxious patients confuse oral sedation with being “put under.” They worry about losing complete control or not waking properly. Oral sedation works differently.
What the medication does in your brain
The medicines used in oral sedation dentistry are usually benzodiazepines. They work by enhancing the effect of GABA at the GABA_A receptor, which increases chloride ion movement into the neuron, reduces cortical excitability, and lowers anxiety without compromising consciousness, with patient-reported anxiety reduction up to 70% under ADA-aligned protocols according to this patient-friendly summary of the pharmacology.
That sounds technical, so let’s translate it.
Your brain has “go” signals and “slow down” signals. GABA is one of the main calming messengers. Oral sedative medication helps that calming system work more strongly. The result is that thoughts race less, physical tension eases, and the sights and sounds of treatment don’t hit you with the same force.
What it feels like from the patient’s side
Patients don’t describe oral sedation as dramatic. They usually say things like:
- “I felt much less bothered by everything.”
- “I knew what was happening, but I didn’t care as much.”
- “I felt sleepy and relaxed.”
- “The appointment seemed to pass faster than I expected.”
You can still respond to simple instructions. If the dentist asks you to open a little wider or turn slightly, you can do that. That’s why this is called conscious sedation.
Conscious sedation versus general anaesthesia
Here’s the comparison that clears up most confusion:
| Option | State of awareness | How it feels | Typical setting |
|---|---|---|---|
| Oral sedation | Awake but deeply relaxed | Drowsy, calm, less reactive | Dental clinic |
| General anaesthesia | Unconscious | Fully asleep | Hospital or specialised setting |
With oral sedation dentistry, you’re still breathing on your own and able to respond. With general anaesthesia, you’re unconscious and need a very different level of medical management. If you’ve been wondering whether you need something lighter first, this explanation of a dentist with nitrous oxide can help you compare another common calming option.
Practical way to think about it: oral sedation doesn’t remove you from the appointment. It makes the appointment feel more tolerable.
Why that matters for fearful patients
When you’re highly anxious, your body treats the dental visit like a threat. Your shoulders tense. Your breathing changes. You focus on every sound. Time feels slow.
Oral sedation changes that internal environment. The procedure itself may be the same filling, crown, extraction, or implant appointment, but your experience of it is very different because your nervous system isn’t firing so loudly.
That’s why patients often say the anticipation was worse than the treatment. Once the medication takes effect, the fear that had been building for days or weeks often loses its grip.
The Life-Changing Benefits of Sedation Dentistry
The primary benefit of oral sedation dentistry isn’t just “feeling calmer.” It’s what that calm allows you to do. You can finally deal with the tooth that’s been bothering you. You can complete more treatment in one sitting. You can stop organising your life around avoiding the dentist.

It helps with more than fear alone
Some patients aren’t mainly afraid of pain. They’re afraid of the whole setup. The reclined position. The need to keep their mouth open. The sounds. The smell. The feeling that they might gag.
Oral sedation can help when the problem is a cluster of sensitivities rather than one single fear. It can be especially useful for:
- Strong gag reflexes that make treatment hard to tolerate
- Low tolerance for lengthy appointments
- Needle fear, especially when anxiety starts before the injection
- Extensive treatment needs, where several issues have built up over time
- Pain sensitivity, where tension makes discomfort feel worse
A good example is wisdom tooth treatment. If you’ve been postponing it because the idea feels too intense, this guide to wisdom tooth removal near me gives useful background on what that process can involve.
Why fewer, calmer visits can matter so much
When someone has multiple dental needs, anxiety often multiplies the problem. They don’t just fear one appointment. They fear a whole string of them. Oral sedation can make it easier to complete more work in a single visit when that’s clinically appropriate.
That matters for people considering things like multiple restorations, veneers, implant-related procedures, or treatment after a long gap in care. Instead of bracing yourself over and over, you may be able to approach care in a more organised, less emotionally draining way.
Patients often say the biggest benefit wasn’t just comfort in the chair. It was finally getting unstuck.
The added comfort of combining sedation with laser dentistry
Another important comfort factor is the technology used during treatment. The integration of oral sedation with laser dentistry, such as Biolase, can reduce recovery time by 30% and post-operative pain by 40%, with 78% better tolerance in pain-sensitive patients compared with traditional methods alone, based on Australian data on sedation and laser synergy.
That combination can make a meaningful difference for anxious patients because it addresses two parts of the experience at once. Sedation helps the mind feel calmer. Laser-based treatment can help the procedure itself feel gentler and recovery feel easier.
Here’s a closer look at how patient comfort can change during treatment:
What people often notice afterwards
After a well-planned sedation appointment, patients commonly feel relieved for reasons that go beyond the procedure itself:
- They proved to themselves they could do it
- They stopped dreading the next step
- They no longer felt trapped by avoidance
- They began to rebuild trust in dental care
That emotional shift can be as important as the clinical work. Once someone has one manageable experience, the next visit usually feels less daunting.
Is Oral Sedation the Right Choice for You
Oral sedation dentistry can be an excellent option, but it isn’t automatically right for every patient. The safest approach is always individual. Your dentist needs to understand not just your anxiety level, but also your medical history, current medications, and the type of treatment planned.
That pre-sedation conversation is not a formality. It’s the part that makes the whole process safe and individualized.
Signs you may be a good candidate
You may benefit from oral sedation if any of these sound familiar:
- You avoid appointments even when you know you need care
- You’ve had a difficult or traumatic dental experience in the past
- Your gag reflex makes treatment hard
- You become tense, shaky, or tearful before treatment
- You need a longer procedure and don’t feel able to cope comfortably
- You’re frightened of injections, sounds, or loss of control
Some people also have no major phobia but still become so keyed up in the chair that routine treatment feels exhausting. Oral sedation can help lower that stress load.
When extra caution is needed
There are also situations where a dentist may recommend a different approach, delay treatment until medical clearance is obtained, or decide oral sedation isn’t suitable. That can apply if you have certain breathing issues, a complex medical history, medication interactions, past reactions to sedatives, or other factors that change the risk profile.
Pregnancy also needs careful discussion. Sedation choices should never be assumed to be routine in that setting.
A safe sedation plan starts with honesty. Tell your dentist about every medication, every supplement, every medical condition, and any past reaction you’ve had to sedation or anaesthesia.
What the consultation usually covers
A proper assessment often includes:
| Topic | Why it matters |
|---|---|
| Medical history | Helps identify conditions that may affect sedation safety |
| Current medicines | Some drugs can interact with sedatives |
| Past sedation experience | Guides planning and risk assessment |
| Anxiety triggers | Helps the team tailor the visit |
| Type of procedure | Determines whether oral sedation is the right level |
This is also where patients often realise they may not need the deepest option available. Some need oral sedation. Others are better suited to inhalation sedation. A smaller group may need something more advanced, which is why it helps to understand the difference between sedation and a full anesthesia dentist.
Safety is built on systems, not guesswork
One reason oral sedation dentistry can feel less frightening once explained is that it’s governed by clinical protocols. Dentists don’t merely hand out a tablet and hope for the best. Suitability, dose selection, monitoring, escort arrangements, and aftercare instructions all matter.
The safest experience comes from matching the right patient to the right type of sedation, with the right preparation. That’s why your consultation should feel like a collaborative conversation, not a sales pitch.
If your instinct has been, “I think I need something, but I’m not sure what,” that’s usually the right place to start. You don’t need to arrive with the answer. You just need to be open about what makes dental care hard for you.
Your Oral Sedation Journey A Step-by-Step Guide
Fear often gets worse in the gaps. Not knowing when to take the tablet, whether you’ll be asleep, how you’ll get home, or what recovery feels like can make the whole thing seem bigger than it is. A clear roadmap usually lowers that stress straight away.
Before your appointment
The process starts with planning, not medication. Your dentist reviews your health history, asks about anxiety, and decides whether oral sedation is appropriate for the treatment you need. If your fear has been stopping you even from attending routine care, it may help to start with something familiar like a checkup and clean and discuss sedation in that context.
If oral sedation is the right fit, you’ll be given specific instructions about the medication and timing. Don’t improvise. Don’t change the dose yourself. The details matter because the goal is controlled, predictable relaxation.
You’ll also need to organise practical support before the day.
- Arrange an escort because you won’t be able to travel home alone in the usual way.
- Clear your schedule so you can rest afterwards.
- Follow any fasting instructions exactly if your dentist gives them.
- Wear comfortable clothing and keep the day simple.
What taking the medication feels like
Many patients expect a dramatic sensation the moment they take the tablet. Usually, it’s gentler than that. The effect tends to build gradually. You may notice your thoughts slowing down, your body softening, and a growing sense that the appointment feels less threatening.
Some people feel chatty. Some feel sleepy. Some feel that the edge has come off everything.
The goal isn’t to make you unconscious. The goal is to make treatment feel manageable.
During the procedure
Once you’re in the chair, the team monitors you and keeps the pace calm. In Australia, oral sedation is associated with a high efficacy rate, and scores above 12 on Corah’s Dental Anxiety Scale correlate with 80% efficacy in calming patients. During treatment, pulse oximetry is used to monitor oxygen saturation and keep SpO2 above 95%, and after treatment a mandatory escort and a 24-hour driving ban apply according to this summary of oral sedation protocols.
From the patient perspective, time can feel blurred. You’ll still be able to respond, but the sensations that would normally keep you tense often feel muted. That’s especially helpful during longer appointments, where anxiety usually builds as time passes.
What the team is watching while you relax
Even when you feel drowsy, the clinical team remains focused on the details that keep treatment safe. They’re observing your comfort, your responsiveness, and your oxygen levels. This is one reason oral sedation should feel structured and organised, not casual.
Here’s a simple snapshot of the treatment phase:
| Stage | What you notice | What the team focuses on |
|---|---|---|
| Settling in | Drowsiness, less tension | Readiness and baseline observations |
| Active treatment | Relaxed, less reactive | Comfort, communication, monitoring |
| Completion | Groggy, calm, often hazy | Safe transition to recovery and discharge |
After the appointment
This is the part many generic articles skip, but it matters a lot in real life. After oral sedation, you may feel sleepy, slow, or foggy for the rest of the day. Even if you feel “mostly fine,” you are not considered fit to drive.
That means no driving yourself home, no solo school pickup, no work decisions that require full concentration, and no treating the day as normal.
A sensible recovery setup looks like this:
- A trusted adult takes you home
- You rest at home rather than returning to errands
- You keep meals simple if your dentist advises it
- You avoid driving for the full 24-hour period
- You follow the specific aftercare instructions for your procedure
What recovery is usually like at home
Patients spend the rest of the day resting, drifting in and out of sleep, and feeling better as the hours pass. You may remember the appointment clearly, vaguely, or in fragments. All of that can be normal.
If the dental procedure itself was more involved, such as an extraction or implant-related appointment, your recovery instructions for the treatment site still matter just as much as the sedation advice. The sedation helps you get through the visit. The aftercare helps you heal well afterwards.
For Inner West patients, the simplest way to make the day easier is to treat transport as part of the treatment plan, not an afterthought. Choose your support person early. Confirm who’s taking you home. Make sure someone can stay reachable. Those small steps remove a lot of last-minute stress.
Comparing Different Dental Sedation Options
Oral sedation dentistry is one useful option, but it sits within a bigger group of calming methods. The right choice depends on your anxiety level, the type of procedure, your medical history, and how much support you want during and after the visit.
Some patients want the lightest option possible. Others know they need something stronger than reassurance alone.
Side-by-side view of common options
| Sedation option | How it’s given | Depth of effect | Recovery considerations | Often suits |
|---|---|---|---|---|
| Nitrous oxide | Inhaled through a mask | Light relaxation | Usually wears off quickly | Mild anxiety, shorter visits |
| Oral sedation | Tablet taken before treatment | Moderate relaxation | Escort needed, rest afterwards | Moderate anxiety, longer visits |
| IV sedation | Medication through a vein | Deeper and more adjustable | Higher level of support and monitoring | Strong anxiety, more complex care |
Nitrous oxide is often the most flexible entry point. It works quickly and is commonly chosen by patients who need help taking the edge off but don’t want a long recovery.
Oral sedation sits in the middle. It doesn’t involve a cannula, which many needle-averse patients appreciate, but it typically creates a deeper feeling of relaxation than laughing gas alone.
IV sedation offers more control over timing and depth, but it’s also a bigger step. For some patients, that’s exactly what makes sense. For others, it’s more than they need.
The practical issue many people forget
The choice isn’t only about how calm you feel in the chair. It’s also about what your day looks like afterwards. In NSW, oral sedation comes with a mandatory escort and a 24-hour driving ban under Road Rules 2014 (Reg 297), and a 2023 ADA survey found 68% of anxious patients are concerned about transport logistics, as noted in this discussion of sedation travel planning.
That’s important in the Inner West, where people often try to fit dental care around work, school runs, or public transport routines. Nitrous oxide may be simpler logistically for some. Oral sedation may be worth the added planning if your anxiety is stronger.
Don’t choose a sedation option based only on fear. Choose based on fear, procedure type, medical suitability, and what recovery support you can realistically arrange.
How the final decision is made
A good dental team won’t push everyone toward the same solution. They’ll look at the whole picture. If your anxiety is mild, a lighter option may be enough. If you’ve been avoiding treatment for a long time or become very distressed in the chair, oral sedation or another stronger approach may be more appropriate.
The best sedation plan is the one that helps you receive care safely, comfortably, and with the least disruption overall.
Experience Comfortable Dentistry in Dulwich Hill
For many people in Dulwich Hill and the Inner West, the hardest part isn’t the treatment itself. It’s making the first call after a long time away. Shame, fear, and uncertainty can all pile up together.
The good news is that comfortable dentistry is possible. With a thoughtful assessment, clear instructions, modern technology, and the right sedation option when needed, dental visits don’t have to feel like something you endure. They can feel calm, respectful, and manageable.

A gentler path can start small
You don’t have to begin with a major procedure. Some patients start with a conversation. Others start with an exam and ask about sedation for future work. What matters is finding a team that listens carefully and doesn’t make you feel rushed or judged.
If comfort is a priority for you, it may help to read more about finding a gentle dentist near me and what that means in day-to-day care.
What local patients often need most
Inner West families and professionals usually want the same few things:
- Clear explanations instead of jargon
- Flexible scheduling that fits real life
- Treatment options that account for anxiety
- A practical recovery plan so the day runs smoothly
Oral sedation dentistry can be part of that solution, especially when paired with a patient-centred approach and technology designed to make care less invasive.
If fear has been keeping you away, you don’t need to solve that alone first. You just need a starting point and a team that understands why this feels hard.
If you’ve been delaying care because you’re anxious, The Smile Spot in Dulwich Hill offers gentle, high-tech dentistry with sedation options suited to your needs. Whether you want to talk through oral sedation, compare it with other comfort options, or take the first step with a calm consultation, you can book with The Smile Spot.