You’ve got something coming up. A wedding, work event, family photos, maybe just the point where you’re tired of seeing coffee and tea stains every time you catch yourself in the mirror.
You want whiter teeth. You don’t want the zingers.
That hesitation is completely reasonable. If your teeth already react to cold water, sweet food, or even a deep breath on a winter morning, whitening can sound like the last thing you should try. A lot of people put it off for exactly that reason. They assume bleaching and sensitivity always go together, and that a brighter smile has to come with a few miserable days afterward.
That isn’t how careful whitening should work. Modern teeth bleaching for sensitive teeth is much more controlled than the aggressive approaches many people still picture. Product strength, contact time, tray fit, gum protection, pre-treatment care, and desensitising agents all matter. So does choosing the right method for your teeth rather than the fastest one on the shelf.
A Whiter Smile Without the Worry
A common story goes like this. Someone used whitening strips years ago, felt sharp pain that evening, and decided whitening just wasn’t for them. Or they’ve never tried it, but a friend told them their teeth “ached for days”, so they’ve stayed away.
That fear makes sense. It also leaves a lot of people stuck with a smile they’d like to brighten but don’t feel safe treating.

Sensitive teeth don’t automatically rule out whitening. They mean the plan needs to be gentler and more deliberate. In practice, that usually means avoiding one-size-fits-all products, checking for causes of baseline sensitivity first, and choosing a method that lets a dentist control the variables that trigger discomfort.
What anxious patients usually need
Individuals with sensitivity aren’t asking for the brightest result possible in the shortest time. They want three things:
- Comfort first: they want to know the process won’t leave them miserable afterward
- Predictability: they want to understand what will happen before, during, and after treatment
- A realistic plan: they want an option that suits their enamel, fillings, lifestyle, and pain threshold
That’s why a gentle approach matters so much. A good whitening plan doesn’t start with gel. It starts with diagnosis.
Practical rule: If your teeth hurt before whitening, the answer usually isn’t stronger whitening. It’s finding out why they hurt first.
Sometimes the best first step is a proper examination and a conversation with a gentle dentist near you. Once the cause of sensitivity is clear, whitening becomes much less of a gamble and much more of a controlled cosmetic treatment.
Why Your Teeth Feel Sensitive During Whitening
Whitening sensitivity isn’t random. There’s a biological reason for it, and once you understand that, the solutions make more sense.
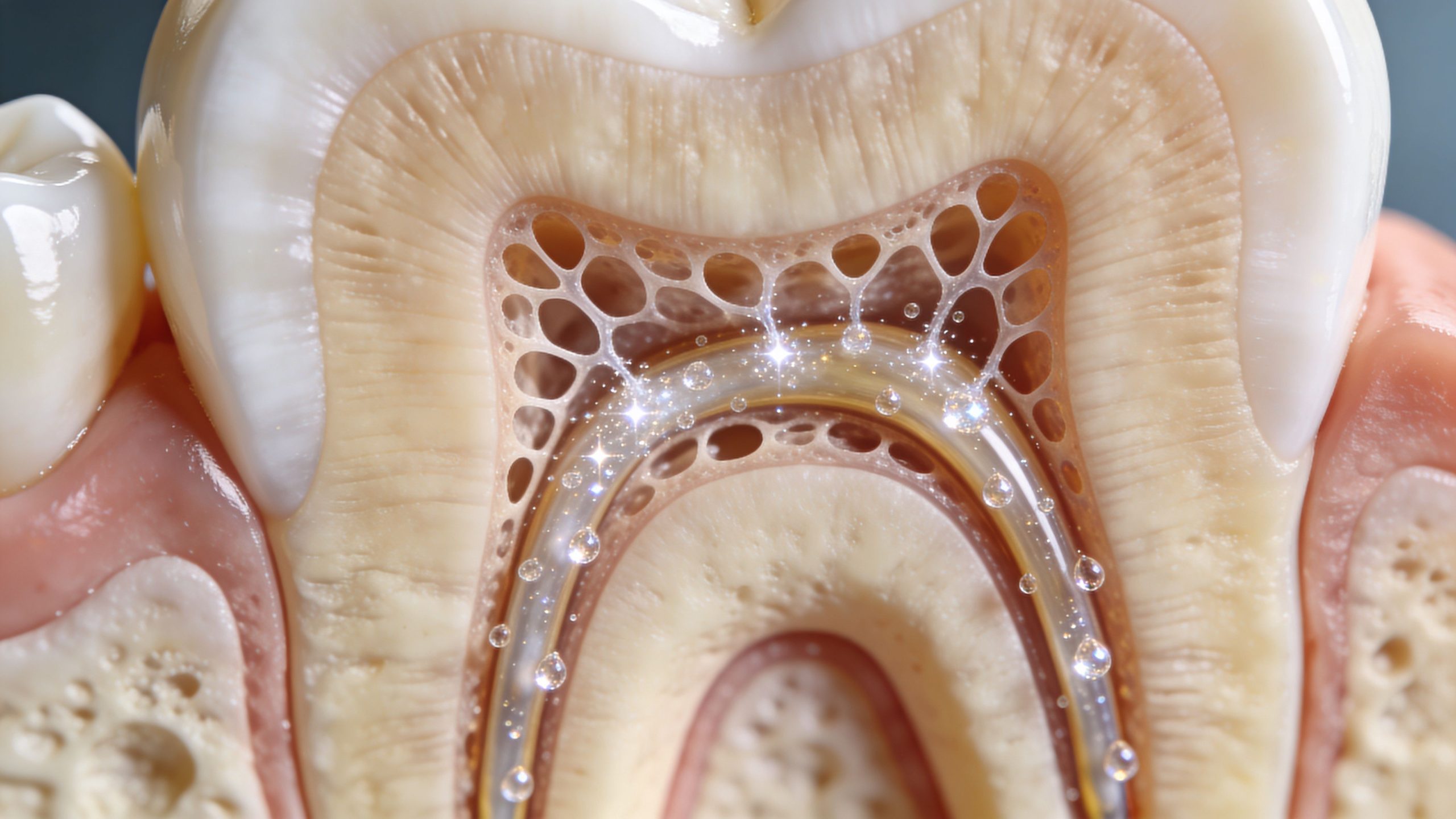
Under the enamel is a layer called dentine. Dentine contains tiny channels called dentinal tubules. The easiest way to think of them is as thousands of microscopic straws that lead toward the nerve inside the tooth. When enamel is thin, worn, or naturally more porous, those tubules are easier to irritate.
Whitening gels use peroxide to break down stain molecules. That same peroxide can travel through those tiny channels. When it does, the nerve inside the tooth can react with a short, sharp pain or a lingering ache.
In Australia, tooth sensitivity is a common side effect of bleaching, affecting up to 70% of patients having hydrogen peroxide-based whitening, and this is often linked to protocols using 38% H2O2 for 20 minutes that can cause significant discomfort, according to this clinical review of bleaching sensitivity.
Baseline sensitivity and whitening sensitivity aren’t the same
These two problems overlap, but they aren’t identical.
Baseline sensitivity is what you notice in daily life. Cold drinks, sweets, brushing near the gumline, or breathing in cold air may trigger it. Common causes include enamel wear, gum recession, grinding, cracks, decay, or exposed root surfaces.
Whitening sensitivity is triggered by the bleaching process itself. Even teeth that normally feel fine can react during or after treatment if the gel is too strong, left on too long, or applied in a way that irritates the gums and exposed dentine.
That difference matters. If someone already has sensitive teeth, whitening can amplify it. If someone has no symptoms at all, they can still develop temporary sensitivity from an aggressive whitening protocol.
Why some whitening methods feel harsher than others
A few things increase the chance of discomfort:
- Higher peroxide concentration: stronger gels work faster, but they also raise sensitivity risk
- Longer contact time: the longer gel sits on the teeth, the more chance it has to penetrate
- Poor tray fit or strip fit: leaking gel can irritate gums and exposed root surfaces
- Existing enamel problems: cracks, erosion, and recession make teeth more reactive
A simple analogy helps here. If dentinal tubules are tiny straws, then aggressive whitening pushes more irritant through those straws, more quickly. Gentle whitening reduces the amount, shortens exposure, or helps seal the straws before and after treatment.
This short video gives a helpful visual overview of the process:
The pain some people feel after whitening doesn’t mean their teeth are “weak”. It usually means the treatment didn’t match the biology of their teeth.
If you’ve ever searched for strong pain relief after dental discomfort, you’ll know why prevention is better than chasing symptoms afterward. That’s one reason a dentist will usually focus on cause, not just relief, much like the thinking behind guidance on Panadeine Forte for tooth extraction.
Professional In-Office Whitening A Controlled Approach
For patients with sensitive teeth, professional in-office whitening is the most controlled way to bleach teeth. That doesn’t mean it’s automatically the right choice for everyone. It means the dentist can manage the parts of whitening that most often go wrong.
That control starts before the gel ever touches the teeth. The gums can be protected, exposed root surfaces can be identified, the peroxide strength can be selected more carefully, and contact time can be shortened if the teeth start reacting.
What professional control changes
A standard over-the-counter product treats every mouth as if it’s the same. Clinical whitening doesn’t.
A dentist can adjust the treatment based on things a box kit can’t assess:
- Where sensitivity is coming from: recession, enamel wear, recent dental work, cracks, or decay
- Which teeth need caution: some teeth react more strongly than others
- How much gel is appropriate: enough to lift stain, not so much that discomfort becomes the main event
- When to stop: if a patient starts feeling significant sensitivity, the protocol can be changed immediately
This is why in-office bleaching often suits patients who want visible change but don’t want to manage the whole process alone.
Desensitising agents aren’t an optional extra
A proper sensitivity-focused protocol often includes a desensitising step before or after bleaching, and sometimes both. Agents such as 5% potassium fluoride and CPP-ACP are used because they help occlude dentinal tubules, which reduces the movement that triggers pain.
Professional in-office treatments use desensitising agents like 5% potassium fluoride and CPP-ACP, which can reduce sensitivity scores by up to 70%, and combining these agents with Biolase laser dentistry can lead to 40 to 50% faster sensitivity resolution than conventional methods, as described in this clinical overview of whitening for sensitive teeth.
Clinical takeaway: Sensitive patients usually do better when whitening and desensitising are planned together, not treated as separate issues.
Where Biolase fits into a gentler whitening plan
Biolase technology matters because it supports a more conservative approach. In practical terms, laser-assisted care can help with precision and comfort. It can reduce unwanted gel spread, support post-treatment desensitising, and fit well with minimally invasive treatment planning.
For an anxious patient, that matters. Less mess, more control, and faster settling afterward can change the whole experience of whitening.
Here’s how many dentists think through the trade-offs in the chair:
| Consideration | Standard aggressive whitening | Sensitivity-focused in-office whitening |
|---|---|---|
| Gel strength | Often chosen for speed | Chosen for tolerance and safety |
| Contact time | Longer or fixed | Adjusted to patient response |
| Gum protection | Limited in DIY use | Carefully controlled |
| Sensitivity support | Usually after symptoms begin | Built into the protocol |
| Monitoring | None at home | Immediate chairside supervision |
If you want a faster cosmetic result but don’t want to guess your way through it, a professionally supervised option is usually the safer path. It’s also why many patients start by learning how professional teeth whitening differs from strips, generic trays, and social media advice.
Custom Take-Home Trays A Safer At-Home Alternative
Some patients don’t want an in-chair procedure. They want to whiten at home, in their own time, with the ability to slow down if a tooth starts to react. For sensitive teeth, that can be a very sensible choice, as long as the kit is professionally designed.
Custom take-home trays are different from pharmacy trays and strips in one significant way. They’re made to fit your teeth, not a generic mouth.
Why custom trays are gentler
A custom tray holds the gel where it’s meant to be and helps keep it off the gums. That sounds simple, but it changes the comfort level considerably. When whitening gel leaks, patients often blame “sensitive teeth” when the actual problem is poor fit and soft-tissue irritation.
Dentist-prescribed custom take-home trays using 10 to 15% carbamide peroxide have been shown to cause 50 to 60% less sensitivity than standard 35% in-office gels, and using a fluoride toothpaste for two weeks beforehand can cut sensitivity risk by up to 65%, according to this review of preparation for whitening sensitive teeth.
That lower, slower approach is often exactly what sensitive patients need.
What the process usually looks like
A take-home system works best when it’s simple and structured:
Assessment first
The teeth and gums are checked to make sure the sensitivity isn’t being caused by decay, cracks, gum recession, or a restoration problem.Custom tray fabrication
Impressions or scans are used to make trays that sit closely against the teeth.Low-concentration gel selection
Carbamide peroxide is commonly chosen because it releases peroxide more gradually.Short, flexible wear time
Instead of pushing through discomfort, the patient can shorten a session, skip a day, or pause altogether.Desensitising support
Fluoride and other soothing products can be used before, during, or after the whitening course.
What works and what usually doesn’t
The main advantage of trays is control. You can spread the treatment out. You can monitor exactly how your teeth respond. You can stop before a small twinge becomes a bad night.
What usually works well:
- Starting with a lower-strength gel
- Using shorter sessions at first
- Whitening every other day if needed
- Using desensitising toothpaste consistently
- Reporting uneven sensitivity early
What tends to go badly:
- Buying the strongest kit available
- Sleeping in ill-fitting trays
- Doubling up sessions before an event
- Continuing through sharp pain
- Using whitening on untreated dental problems
If a patient tells me, “I want the safest way to whiten at home,” custom trays are usually the conversation worth having, not strips.
There is a trade-off, of course. Results come more gradually than in-office bleaching. For many people with sensitivity, that isn’t a disadvantage. It’s the reason the treatment remains tolerable.
Comparing Your Gentle Whitening Options
Not every patient wants the same thing. Some want the quickest possible result under close supervision. Others want the freedom to go slowly at home and stay in control of every session.
That’s why the best choice isn’t “the strongest whitening”. It’s the option that matches your teeth, your schedule, and your tolerance for sensitivity.
A side-by-side look
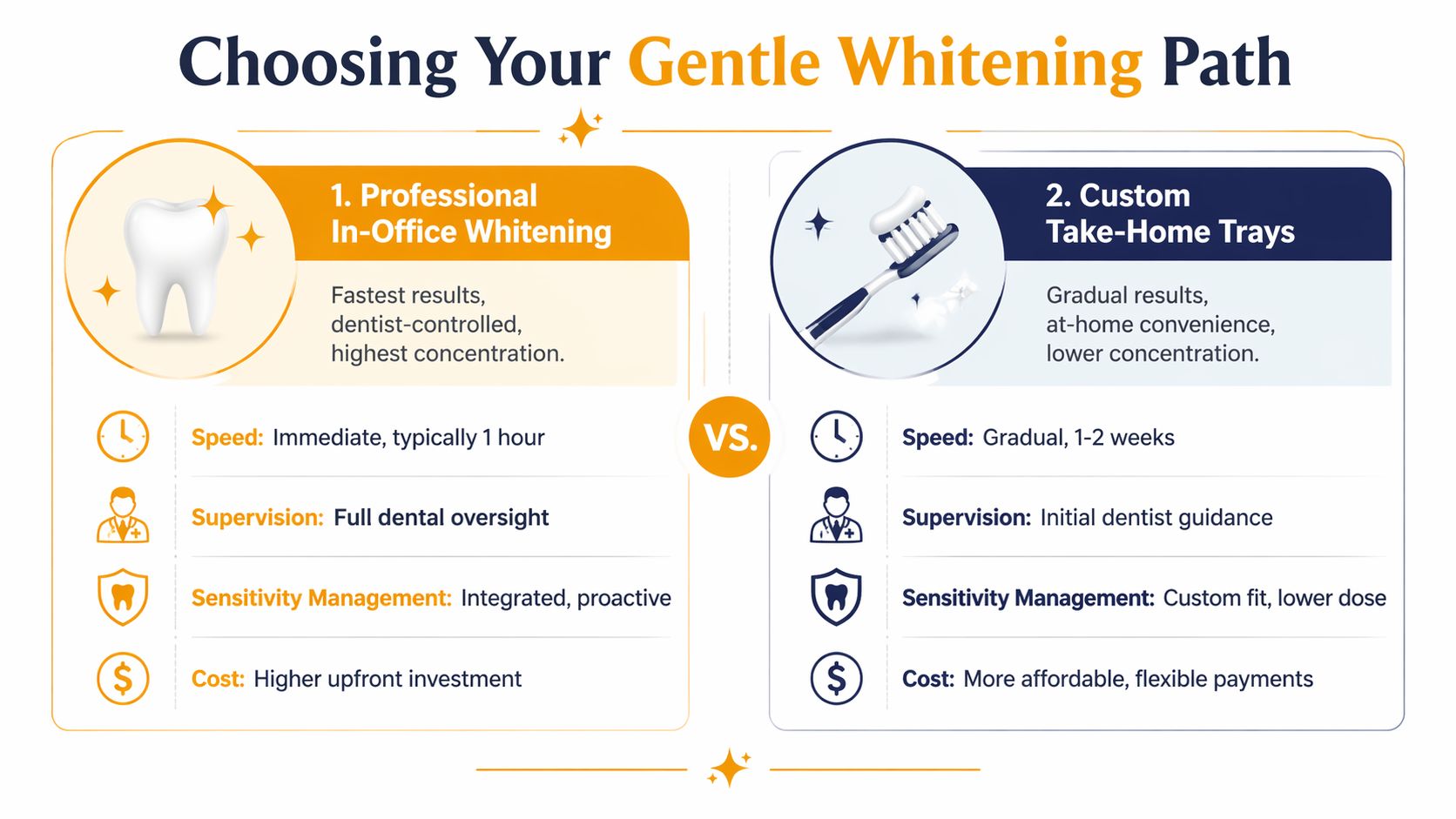

The infographic above summarises the practical differences. In everyday terms, the decision often comes down to this:
| Factor | In-office whitening | Custom take-home trays |
|---|---|---|
| Best for | Faster change with supervision | Gradual change with flexibility |
| Sensitivity management | Immediate chairside adjustment | Patient-controlled pacing |
| Convenience | One planned appointment | Home use over multiple sessions |
| Monitoring | Continuous during treatment | Reviewed before and after |
| Pace | Quicker | Slower and steadier |
How whitening got to this point
Modern whitening is much better than early one-size-fits-all approaches. The shift really started in the 1990s, when carbamide peroxide trays became the standard for at-home use because they were associated with lower sensitivity, and a 2018 Cochrane review confirmed that sensitivity is the top adverse effect of whitening methods, reinforcing the need for gentler protocols and better technology, as outlined in this review of whitening statistics and trends.
That history matters because it explains why dentists no longer think in simple terms like “in-chair is best” or “home whitening is safer”. The details matter more than the setting.
Which option usually suits which patient
A few patterns show up often:
- Choose in-office whitening if you want a faster result, prefer professional supervision, and feel more comfortable with the dentist managing the process
- Choose custom trays if you want more control, prefer a gentler pace, and don’t mind waiting longer for the final shade
- Pause and reassess if your sensitivity is already active day to day, because whitening may need to wait until the cause is treated
Patients often ask about cost before they ask about comfort, but the more useful question is usually value. If you’re weighing those trade-offs, it helps to compare the practical considerations around how much teeth whitening costs alongside comfort, maintenance, and suitability.
Beyond Bleaching Cosmetic Alternatives for a Brighter Smile
Sometimes bleaching isn’t the best answer. That isn’t bad news. It just means the smile problem is different.
If the discolouration sits inside the tooth rather than on the surface, if enamel is already worn, or if there are multiple crowns, fillings, or bonding on the front teeth, bleaching may give a limited or uneven result. Restorations don’t whiten the way natural enamel does.
Whitening is especially difficult for restored teeth. In patients with restored teeth, 35% hydrogen peroxide causes sensitivity in 100% of cases, with pain intensity 2 to 3 times greater than in sound teeth, and this matters because over 60% of NSW adults aged 35 to 54 have at least one restoration, according to this review on bleaching sensitivity in restored teeth.
When veneers make more sense
Veneers don’t lighten the original enamel. They cover the visible front surface of the tooth. That means they can improve colour, shape, edge wear, and minor alignment issues at the same time.
This is often the better path when someone has:
- Dark internal staining that won’t respond evenly to bleaching
- Old fillings on front teeth that already differ in colour
- Worn or chipped enamel where extra bleaching may not be wise
- A smile makeover goal rather than a simple shade improvement
Porcelain options such as E.max are usually chosen when patients want a more extensive cosmetic change. Composite bonding can be a more conservative option for smaller improvements.
When bonding is the better fit
Bonding is useful when the problem is local rather than full-smile. A single dark tooth, a chipped incisor, uneven edges, or a patchy area around an old filling may be better corrected by adding tooth-coloured material than by trying to bleach everything around it.
That’s one of the more important trade-offs in cosmetic dentistry. Bleaching is excellent when the underlying tooth structure is healthy and the stains are suitable. It’s not a cure-all.
Some smiles don’t need stronger whitening. They need a different tool.
If you’re trying to improve oral habits while protecting sensitive teeth, simple low-abrasion routines matter as much as cosmetic treatment. Some patients also like to learn about traditional options such as natural herbal chew sticks for oral health, especially when they’re looking for gentler daily care alongside professional advice.
Your Pre-Care and Post-Whitening Comfort Plan
A comfortable whitening experience usually starts before treatment and continues for a few days after it. Most of the avoidable discomfort happens when patients prepare poorly, then go straight back to hot coffee, cold drinks, and hard brushing once the session is over.
A simple plan works better than a long list of rules.
Before whitening
Think of the lead-up as enamel preparation, not just appointment prep.
Use a desensitising toothpaste consistently
Products with potassium nitrate or fluoride need time to work. Using them for a couple of weeks before whitening is more useful than starting the night before.Brush gently
A soft-bristled toothbrush helps. If you scrub, you can irritate the gumline and make exposed areas more reactive.Deal with existing problems first
Whitening over decay, cracks, leaking fillings, or inflamed gums is asking for trouble.Reduce other irritants
Very acidic food and drink can leave teeth feeling more reactive. Keeping them in check before whitening often helps.
After whitening
The teeth are often temporarily more responsive after bleaching, so the first day or two matter.
| Time | What to do | Why it helps |
|---|---|---|
| First few hours | Avoid very hot and very cold food and drinks | Limits temperature-triggered discomfort |
| First day or two | Choose lighter-coloured foods and drinks where possible | Helps reduce immediate restaining |
| Ongoing | Keep using a soft brush and sensitivity toothpaste | Supports recovery and comfort |
| If advised | Apply prescribed desensitising gel or mousse | Helps settle post-treatment zing |
Aftercare advice: If sensitivity appears, don’t panic and don’t push ahead with more whitening. Give the teeth time to settle.
One of the best foundations for any cosmetic treatment is a recent examination and professional clean. If there’s plaque, tartar, gum inflammation, or an undiagnosed issue, comfort tends to suffer. That’s why many whitening plans sensibly begin with a check-up and clean.
Begin Your Journey to a Confident Smile in Dulwich Hill
Sensitive teeth can make whitening feel risky, but sensitivity isn’t the end of the conversation. It’s the reason the treatment needs to be chosen carefully.
For some people, the best option is controlled in-office bleaching with integrated desensitising support. For others, custom take-home trays offer the right mix of comfort, convenience, and flexibility. And for patients with restorations, enamel wear, or stain types that won’t respond predictably, veneers or bonding may be the smarter cosmetic path.
The important part is not guessing.
A proper assessment can tell you whether your sensitivity is manageable, what’s causing it, and which whitening method is least likely to trigger pain. That’s especially valuable if you’ve had a bad whitening experience before or have been avoiding treatment because you expect the worst.
If you’re in Dulwich Hill or the Inner West and want a brighter smile without taking unnecessary risks, book a consultation and get a plan that suits your teeth rather than a generic kit.
If you’re ready to explore gentle whitening, veneers, or a personalised plan for sensitive teeth, contact The Smile Spot. Dr. Dimitrios Thanos and the team provide family-focused dental care in Dulwich Hill with a strong emphasis on comfort, clear advice, and modern treatment options, including Biolase laser dentistry and support for anxious patients.