You’re probably here because something at the back of your mouth has started to feel off. It might be a dull pressure behind your last molar, a gum flap that keeps getting irritated, or pain that seems to travel into your jaw and ear when you’re trying to get through work, school pick-up, or dinner at home.
That’s usually when people search for wisdom tooth removal near me. They want a local answer, a clear plan, and a dentist who can explain what’s going on without making the whole thing feel bigger or scarier than it needs to be. In Dulwich Hill and across the Inner West, that matters. Patients typically aren’t looking for a dramatic surgical experience. They’re looking for a careful assessment, a gentle procedure, and the shortest practical recovery.
Your Local Guide to Wisdom Tooth Removal in Dulwich Hill
Wisdom teeth tend to cause subtle trouble at first. A little tenderness. Food trapping at the back. A bad taste near the gum. Then one day it’s hard to chew on one side, or your jaw feels tight when you wake up. By then, many individuals are juggling discomfort with a busy schedule and trying to work out whether it’s urgent or whether they can ignore it for another month.
In a family dental practice, this pattern is familiar. The earlier a wisdom tooth is assessed, the simpler the conversation usually becomes. Sometimes the answer is monitoring. Sometimes the tooth is healthy and fully functional. Other times the position of the tooth, the surrounding gum, or the way it’s pressing on the second molar tells us it’s unlikely to settle down on its own.
For Inner West patients, convenience matters almost as much as treatment quality. If you’re comparing options, it helps to choose a clinic that already understands family care, anxious patients, and the reality of weekday time pressure. That’s the same reason many local patients start with a broader look at what to expect from a family dentist near you before booking a wisdom tooth assessment.
A good wisdom tooth consultation should leave you less confused than when you arrived. You should know what the tooth is doing, why it matters, and what your options are.
Modern removal is also very different from the old stories people still hear. Careful imaging, more precise planning, and minimally invasive tools have made the process more controlled and more comfortable for many patients. If you’ve been putting this off because you expect a rough recovery or a stressful appointment, that expectation often belongs to an older style of treatment, not the one many patients receive today.
Recognising the Signs You Need Wisdom Tooth Removal
Wisdom teeth don’t always arrive with dramatic pain. In many cases, the earliest sign is the back of the mouth becoming harder to keep clean. The gum may feel tender when brushing. Food may lodge behind the second molar. You might notice occasional pressure without being able to point to one exact tooth.
That matters because wisdom tooth problems often build from limited space and poor access. If a tooth doesn’t have room to come through properly, it behaves like a car trying to fit into a parking spot that’s already occupied. It presses, tilts, traps debris, and irritates the tissues around it. The discomfort may come and go, but the underlying issue usually doesn’t.

In Australia, wisdom tooth removal is a highly prevalent procedure. Data from the Australian Institute of Health and Welfare indicates oral surgeons performed approximately 65,000 third molar extractions in 2019-20, representing about 25% of all tooth extractions in public hospitals according to this summary of AIHW wisdom tooth extraction figures. In other words, if you’re dealing with this in the Inner West, you’re not dealing with anything unusual.
Common early warning signs
Some symptoms are mild enough that people dismiss them for months. The most common signs include:
- Aching at the back of the jaw that flares during chewing or in the evening
- Tender gum tissue behind the last visible molar
- A bad taste or bad breath caused by food and bacteria collecting around a partly erupted tooth
- Pressure against nearby teeth, especially if the wisdom tooth is angled
- Difficulty cleaning the area even with a good toothbrush and floss routine
A partly erupted wisdom tooth is especially prone to irritation because the gum around it forms a sheltered space. Bacteria love sheltered spaces. Once they settle in, the tissue can become inflamed very quickly.
Signs that need prompt attention
Other symptoms suggest the area has moved beyond simple irritation and into infection or significant inflammation. These signs usually deserve an examination sooner rather than later:
- Swelling near the back teeth or along the jaw
- Jaw stiffness or trouble opening wide
- Pain when swallowing
- Pus, a foul taste, or obvious gum infection
- Pain spreading into the ear, temple, or throat
Practical rule: If pain is strong enough to change how you eat, sleep, speak, or open your mouth, it’s time to stop monitoring and get the tooth assessed.
Why waiting often makes things worse
Patients often hope the pain will pass once the tooth “comes through properly”. Sometimes that happens. Often it doesn’t. A wisdom tooth that’s partly trapped under gum or bone may continue to flare because the position itself is the problem.
When I explain this chairside, I usually keep it simple. If a tooth can’t clean itself, and you can’t clean it properly either, the mouth keeps paying for that design flaw. The result may be repeated infection, gum damage around the second molar, or decay in an area that’s difficult to restore predictably.
The main value of early diagnosis isn’t just pain relief. It’s avoiding a more complex problem later.
Understanding Your Wisdom Teeth Erupted vs Impacted
Not every wisdom tooth needs removal. The right decision depends on how the tooth has erupted, whether it can be cleaned, and whether it’s affecting the teeth and bone around it. Patients often hear the word “impacted” without being told what that really means, so it helps to break it down clearly.
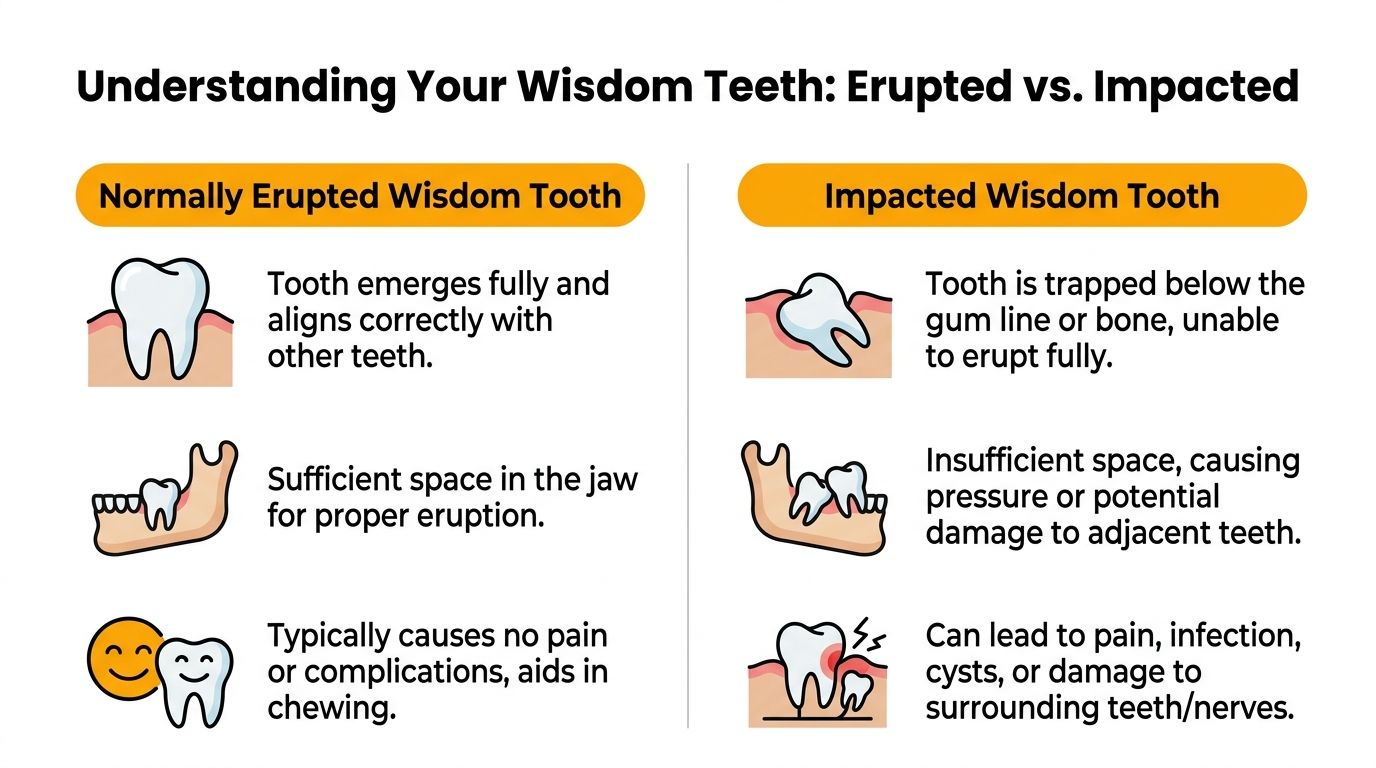
Australian-specific data indicates that wisdom tooth impaction affects approximately 37% of adults aged 20-30, with NSW at 42% prevalence, based on this reported University of Sydney study summary. That’s one reason proactive assessment matters so much in younger adults.
The main difference at a glance
| Tooth position | What it means | Typical concern |
|---|---|---|
| Normally erupted | The tooth has come through fully and lines up with the bite | Often manageable if it’s healthy and cleanable |
| Partially erupted | Part of the tooth is visible, but some remains under gum | Food trapping, inflammation, repeated infection |
| Fully impacted | The tooth remains trapped under gum or bone | Pressure, decay risk, damage to nearby structures |
A normally erupted wisdom tooth can sometimes stay if it’s healthy, functional, and easy to maintain. The key phrase is easy to maintain. A tooth can be fully visible and still be a poor long-term keeper if it sits too far back to clean properly.
A partially erupted wisdom tooth tends to cause the most day-to-day nuisance. It sits in an awkward middle state. Not fully through, not fully buried, and often covered by a small gum flap that catches bacteria.
A fully impacted wisdom tooth may cause no symptoms at all for a period of time. That doesn’t mean it should automatically stay or automatically come out. It means the position needs to be evaluated in the context of risk.
Types of impaction and why they matter
Dentists also describe impacted wisdom teeth by angle. These terms sound technical, but the idea is straightforward.
- Mesioangular impaction means the tooth leans forward into the tooth in front
- Distoangular impaction means it angles backward
- Vertical impaction means it’s upright but still trapped
- Horizontal impaction means it lies sideways against the adjacent tooth
Each pattern changes the treatment plan. A forward-leaning tooth may threaten the second molar. A horizontal tooth may need sectioning into smaller pieces for safer removal. A vertical tooth may be more straightforward than it first appears, or less so if it sits deep in bone.
An impacted wisdom tooth isn’t defined by pain alone. It’s defined by position, access, and the effect it’s having on the rest of the mouth.
When an erupted tooth can still be a problem
This catches many patients by surprise. A wisdom tooth can be visible in the mouth and still be the wrong tooth to keep. If it sits beyond your normal brushing reach, if the gum behind it stays inflamed, or if it contributes little to chewing, removal may still be the cleaner long-term option.
That’s why diagnosis shouldn’t stop at “it has come through”. Rather, the question is whether it has come through in a way that serves your mouth well.
The Wisdom Tooth Removal Procedure at The Smile Spot
Most anxiety around wisdom tooth removal comes from not knowing what will happen. Once the process is broken into steps, it usually feels far more manageable. The modern appointment is planned, measured, and adapted to the position of the tooth rather than handled as a one-size-fits-all extraction.
The first visit and treatment planning
The first step is a proper assessment. We listen to the history first. Where is the pain, how long has it been happening, is it constant or intermittent, has there been swelling, and is there any difficulty eating or opening? Those details matter because symptoms don’t always match the visible appearance of the tooth.
Imaging then does the heavy lifting. Standard dental imaging often shows the broad picture, but impacted wisdom teeth sometimes need more detailed planning to assess roots, angulation, and proximity to nearby structures. Consequently, modern diagnostics transform the patient experience. The more precisely a tooth is mapped before treatment, the less guesswork there is during the procedure itself.
For patients who are especially nervous about surgery, comfort planning is just as important as surgical planning. Some people are completely fine with local anaesthetic and a calm explanation. Others need a stronger sense of control and want to know their options ahead of time. If you’ve been searching for more information on sedation and deeper comfort options, this guide to a full anaesthesia dentist can help you understand where that fits into dental care.
What the procedure actually feels like
During the appointment, the goal is numbness first, then control. Patients shouldn’t feel sharp pain. They may feel pressure, movement, or vibration, but not pain. That distinction helps because people often confuse “I can feel something happening” with “something is wrong”. It usually isn’t.
The exact technique depends on the tooth. A simple erupted tooth may be removed with a more conventional extraction approach. A buried or awkwardly angled tooth may need the gum gently opened, small amounts of surrounding bone adjusted, and the tooth divided into sections so it can be lifted out with less force.
The smoothest removals don’t rely on strength. They rely on access, visibility, and precision.
Here’s a helpful visual overview of the treatment process and what patients can expect during a wisdom tooth procedure:
Why minimally invasive tools matter
The biggest shift in modern wisdom tooth removal is the move away from unnecessarily traumatic techniques. According to this review of minimally invasive third molar surgery techniques, piezoelectric or laser-assisted surgery can reduce bone vibration by 80% compared with traditional drills. The same source reports 30-50% less postoperative pain and 40% faster healing, with return to a normal diet in 3-5 days instead of 7-10.
That difference is practical, not theoretical. Less vibration usually means the procedure feels calmer. More precise cutting means less disturbance to surrounding tissue. Better control of the surgical site usually means less swelling and a cleaner recovery.
In the right case, Biolase laser dentistry is one of the tools that supports that gentler approach. It allows soft tissue management with precision, helps with haemostasis, and can make the area easier to keep clean during the early healing phase. It isn’t a magic wand and it doesn’t replace sound surgical judgement, but used properly, it can make the experience noticeably smoother.
After the tooth is removed
Once the tooth is out, the focus shifts immediately to protecting the blood clot and reducing inflammation. You’ll be given clear instructions on biting pressure, food texture, cleaning, and what to avoid in the first few days. If the site has been handled carefully from the beginning, the aftercare phase tends to be simpler too.
Patients usually cope best when the whole experience is explained in ordinary language. Not every wisdom tooth is easy. But very few are as mysterious as people fear before they’ve had them properly assessed.
Navigating Costs Health Funds and Financing in NSW
Cost matters. It matters even more when you’re trying to plan treatment around school fees, rent, travel, or a week that already feels too full. The most helpful discussion about wisdom tooth fees is a direct one. What affects the total, what might your health fund cover, and where can people accidentally pay more than they need to?
According to this reported AIHW NSW cost summary, the average out-of-pocket cost for impacted wisdom teeth surgery in NSW is AU$800-$1,500 before rebates. The same source says 52% of Inner West residents under-claim their private health extras, and that extras can cover up to 80% of the cost at clinics that accept major health funds. That under-claiming point is important. Many patients focus on the gross fee without first checking what their policy includes.
What usually changes the fee
Wisdom tooth removal isn’t priced by one factor alone. A quote usually reflects several moving parts:
- Tooth position. A fully erupted tooth is usually less complex than a deep impaction.
- Number of teeth. One tooth and four teeth are very different appointments.
- Imaging needs. More detailed planning may be necessary where roots or nearby structures need closer evaluation.
- Sedation choice. More comfort support often changes the total cost.
- Surgical time. The more difficult the access, the more careful time the procedure takes.
A transparent quote should itemise these parts in plain English. If it doesn’t, ask. Patients should know what they’re paying for before treatment begins.
How to use your health fund properly
Private health cover can help, but only if it’s used correctly. Before you book treatment, ask for:
- Your level of extras cover
- Any waiting periods
- Whether surgical extraction items are included
- Whether sedation attracts a separate fee or rebate
- Any annual limits that may affect your claim
One practical reason patients like an examination-first approach is that it separates diagnosis from the final treatment decision. At The Smile Spot, for example, there’s a $240 care package that includes an exam, X-rays, scale and fluoride. That gives patients a starting point for planning without committing to a procedure before they understand the case.
When payment plans are worth considering
Some patients prefer to spread treatment costs rather than delay care while symptoms worsen. That can be sensible, especially when repeated infections are disrupting work and home life. If you’re comparing ways to budget treatment, this guide to dentists with payment plans near me is a useful place to start.
A cheaper quote isn’t automatically the better option if it leaves out imaging, aftercare, or a realistic comfort plan. The better question is whether the quote matches the complexity of your case.
The strongest financial decision is usually the one that combines a clear diagnosis, an itemised estimate, and an understanding of your rebate options before the appointment is booked.
Your Guide to a Smooth and Fast Recovery
Those asking about wisdom tooth removal near me are also asking a second question they don’t always say out loud. How quickly can I get back to normal? If you live in the Inner West, your normal may mean commuting, working face to face, managing children, or fitting treatment around a packed week. Recovery advice needs to match real life.
According to this reported University of Sydney laser-assisted recovery summary, traditional recovery can cause 3-5 missed workdays, while clinics using Biolase laser technology report up to 40% faster healing. The same source says recovery for laser-assisted extractions was often reduced to 2-3 days in that study. That’s a meaningful difference for patients who can’t disappear from their routine for a full week.
The first day matters most
The first 24 hours are about protecting the site. The blood clot that forms in the socket is part of normal healing. If that clot gets disturbed too early, pain usually increases and healing becomes slower.

Use this simple approach on day one:
- Rest with your head slightly raised rather than lying flat for long stretches
- Use the gauze as instructed to control early bleeding
- Apply a cold pack externally in short intervals if swelling begins
- Stick to soft, cool foods that don’t need vigorous chewing
- Avoid straws, smoking, or forceful rinsing because suction can disturb the clot
If your throat feels scratchy after treatment, that can be from mouth breathing, dryness, or keeping the mouth open during the procedure. It isn’t always a sign of infection. Patients who already wake dry or irritated may find this guide on waking up with a sore throat helpful for understanding the non-dental reasons throat discomfort can linger overnight.
Days two and three
This is usually the point where people decide whether recovery is going well. Mild swelling, tenderness, and some stiffness can still be normal. The key is that things should feel stable or gradually easier, not dramatically worse.
A practical routine looks like this:
- Keep meals soft but nourishing. Think yoghurt, soup once it’s cooled appropriately, scrambled eggs, mashed vegetables, soft pasta, or smoothies eaten without a straw.
- Resume gentle cleaning. Brush the rest of the mouth normally, but avoid knocking the surgical area.
- Take medications exactly as directed. Don’t wait for discomfort to spike before using recommended pain relief.
- Give yourself margin. If you can work from home or reduce talking for a day, use that flexibility.
Recovery usually goes best when patients do less, not more, in the first couple of days.
The first week
By this stage, many people are steadily returning to ordinary meals and routine. That doesn’t mean the site is fully healed. It means the most delicate phase has passed. Keep the area clean, avoid poking at it with your tongue, and don’t rush back into crunchy or sharp foods if the socket still feels tender.
Watch for symptoms that need a call to the clinic:
| Likely normal | Worth checking promptly |
|---|---|
| Mild swelling | Swelling that keeps increasing |
| Aching that improves with time | Pain that becomes more intense after initial improvement |
| Small oozing early on | Ongoing heavy bleeding |
| Temporary jaw stiffness | Difficulty opening that worsens rather than settles |
| Mild throat dryness | Fever or a strong foul taste with worsening pain |
If you want a more detailed checklist for meals, cleaning, and warning signs, this guide on wisdom teeth removal recovery tips is useful to keep on hand after the appointment.
What helps and what doesn’t
Some habits consistently support healing. Rest helps. Soft foods help. Clear instructions help. Gentle surgical technique helps most of all.
What doesn’t help is trying to “test” the area. Crunchy foods, smoking, aggressive rinsing, and constant checking with your tongue all tend to irritate the site. Patients often feel better sooner when they leave the area alone and let the tissue do its job.
Why Choose The Smile Spot for Your Procedure
Choosing where to have a wisdom tooth removed comes down to more than location. The right clinic should make the process feel organised, not rushed. Careful, not vague. Modern, but also grounded in experience.
Dr. Dimitrios Thanos has served as principal dentist since 1996, and that kind of continuity matters in a procedure people often approach with some hesitation. Experience doesn’t just affect technical skill. It affects judgement. Knowing when a tooth should be monitored, when it should come out, and how to tailor the plan to the person in the chair is what patients feel during treatment.
What patients usually care about most
For busy professionals and families in Dulwich Hill, the decision often rests on a few practical factors:
- Can the clinic explain things clearly so you understand the diagnosis and next step?
- Is the approach gentle enough for an anxious or pain-sensitive patient?
- Does the technology support faster healing rather than merely sounding impressive?
- Are appointments workable if you need late or Saturday availability?
- Will the quote be transparent before the procedure is booked?
These are sensible questions. They’re also the same questions that tend to lead patients toward a more comfortable experience overall.
A better fit for anxious patients
Many people don’t fear the extraction itself as much as the feeling of losing control. A clinic that takes time with numbness, explains sensations in advance, and offers comfort options usually changes that experience dramatically.
If that sounds like you, it may also help to read more broadly about what patients often mean when they search for a gentle dentist near me. The principles are the same. Clear communication, steady technique, and no unnecessary roughness.
A wisdom tooth appointment feels very different when the dentist plans around your anxiety instead of expecting you to simply cope with it.
Local care that suits real schedules
Inner West patients don’t need generic advice. They need care that works around workdays, school runs, traffic, and short windows of availability. That’s why local access, online booking, and practical appointment times make such a difference. When the process is easier to start, people are less likely to wait until the pain is impossible to ignore.
If your symptoms keep returning, the most useful next step is a consultation. Not because every wisdom tooth must come out, but because once the position is properly assessed, the uncertainty usually disappears.
Frequently Asked Questions About Wisdom Tooth Removal
Do all four wisdom teeth need to be removed at once
No. Treatment should match the condition of the teeth, not a blanket rule. Some patients only need one removed. Others benefit from removing multiple wisdom teeth in one appointment because the teeth are all likely to cause trouble and it’s more practical to recover once rather than several times. The right choice depends on symptoms, position, cleaning access, and your schedule.
What’s the best age for wisdom tooth removal
Earlier adulthood is often the period when wisdom teeth first start causing issues or become easier to assess clearly on imaging. The key isn’t age by itself. It’s whether the tooth is likely to erupt properly, whether it can be maintained, and whether delaying treatment is likely to make removal more difficult. If a younger patient has recurring gum irritation or an impacted tooth, an early opinion is usually worthwhile.
What should I do if I have severe pain right now
Start with simple measures. Avoid chewing on that side. Keep the area as clean as you can without traumatising it. Use any pain relief that’s appropriate for you and that you would normally take safely. If there’s swelling, jaw stiffness, a foul taste, or difficulty swallowing, don’t wait for it to “settle”.
Is wisdom tooth removal always surgical
No. A fully erupted wisdom tooth may sometimes be removed more easily. A buried or angled tooth often needs a surgical approach because the gum or bone blocks direct removal. The purpose of the assessment is to inform you which type of appointment you require.
Will I be awake during the procedure
Many patients are treated comfortably with local anaesthetic, which means you’re awake but numb. Some patients also prefer sedation support depending on anxiety level, complexity, and medical suitability. That decision is part of planning, not something that should surprise you on the day.
If you’ve been putting off that aching, swollen, or hard-to-clean wisdom tooth, the next step is simple. Book a consultation with The Smile Spot to have the area assessed properly, discuss your options clearly, and plan treatment around comfort, recovery, and your schedule.