If you're thinking about implants, your first question usually isn't about titanium or crown design. It's much simpler. How long will recovery take, and what will those first few days feel like?
That concern is normal, especially if you live a busy Inner West life and can't disappear from work, school runs, sport, or family commitments for weeks. Most patients want a straight answer. They also want to know the difference between what feels healed and what is actually healed.
Dental implants recovery time has two parts. The first is the part you notice: soreness, swelling, eating carefully, and getting back into your routine. The second is the part you don't notice: the implant settling into the jawbone and becoming stable enough to support the final tooth for the long term.
The practical overview is this. The early recovery is usually quicker than people expect, while the deeper healing takes longer and needs patience. If you're considering dental implants in Inner West Sydney, it helps to understand the whole process from day one to the final restoration, so nothing catches you off guard.
Your Guide to Dental Implant Recovery in the Inner West
Individuals in Dulwich Hill don't want a technical lecture. They want to know whether they'll be swollen for days, whether they can talk normally, when they can eat properly again, and how long it will be before the implant feels like part of them.
Those are the right questions.
A good recovery plan starts with realistic expectations. The gum and soft tissue settle first. Your comfort usually improves well before the implant has fully integrated with bone. That gap matters, because feeling fine too early can lead patients to chew too hard, push activity too soon, or assume the job is finished when the biology is still catching up.
What recovery usually feels like
In the early stage, tenderness, mild bleeding, and some swelling are common. Then things become more manageable, often quite quickly. After that, there is a quieter phase where you may feel normal, but the implant is still doing its most important work under the surface.
Recovery is rarely one long stretch of discomfort. It's usually a short active healing period followed by a longer waiting period where protection and patience matter more than pain relief.
What makes recovery smoother
The implants themselves are only one part of the experience. The rest comes down to planning, surgical technique, aftercare, and how well the healing phase is protected.
What tends to help most is straightforward:
- Careful surgical technique: Less tissue trauma usually means less swelling and an easier first few days.
- Clear instructions: Patients recover better when they know exactly what to eat, how to clean, and what not to do.
- Support during the waiting phase: The months after placement matter just as much as the day of surgery.
- Technology that reduces tissue disruption: Minimally invasive approaches can make the early phase more comfortable.
The Full Dental Implant Recovery Timeline at a Glance
Think of implant recovery as a staged build, not a one-day fix. You may have the implant placed in a single appointment, but the finished result depends on several separate healing milestones.
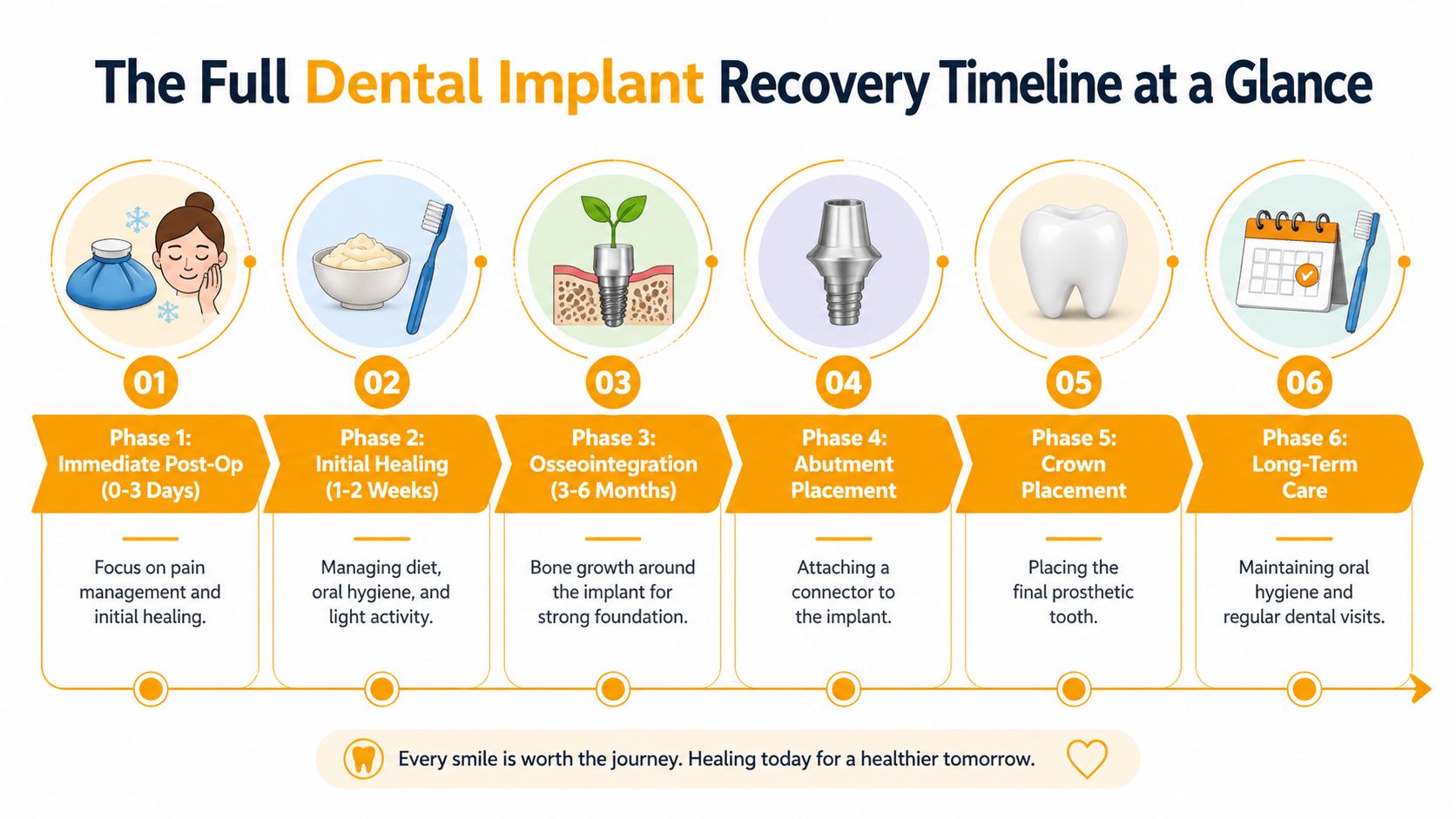
The shortest phase is the one that commonly causes concern. The longest phase is the one that generally goes unfelt.
The recovery map
| Phase | What you notice | What matters most |
|---|---|---|
| Immediate post-op | Soreness, swelling, minor bleeding | Rest, cold compresses, medication, protecting the site |
| Initial healing | Eating gets easier, mouth feels more normal | Soft diet, gentle cleaning, no unnecessary pressure |
| Osseointegration | Usually very little day-to-day discomfort | Bone fusing to the implant without overload |
| Abutment stage | Minor procedure if needed | Letting the gum settle around the connector |
| Crown placement | Function and appearance come together | Ensuring the bite is balanced and comfortable |
| Long-term care | Normal daily life | Maintenance, hygiene, and regular reviews |
The stage that sets the pace
The key term to know is osseointegration. That is the biological fusion between the implant and your jawbone. It is the pacing item for the whole process.
According to this overview of how long dental implants take to heal, osseointegration typically takes 3 to 6 months, and clinical verification is performed at the 3 to 6 month mark before moving to abutment and crown placement. That waiting period isn't optional. If a restoration is placed too early, implant failure becomes a real risk.
Why the timeline can feel confusing
Patients often judge healing by symptoms. That's understandable, but it's incomplete. You may feel largely back to normal while the implant is still stabilising inside the bone.
The best way to think about dental implants recovery time is this: your comfort improves first, your function returns next, and the biology finishes last.
If you'd like a broader sense of the long-term outcome after healing, our article on how long dental implants last explains what helps implants stay healthy for years.
Managing the First 72 Hours After Your Implant Procedure
This is the part patients tend to fear most. In practice, it's usually very manageable when you know what's normal and when you've prepared properly.

The first day is about protection, not testing yourself. Don't poke the area, don't keep checking it in the mirror, and don't try to “eat normally” just to see if you can. The less disturbance around the site, the calmer those first few days usually are.
Day 0 and the first evening
Minor oozing can happen early on. That's different from heavy bleeding. Keep pressure where instructed, rest, and stay with cool or lukewarm fluids and soft foods if you're eating at all.
Your jaw may feel tight. That's common. If you had sedation, plan for a quiet day and avoid making decisions, driving, or trying to jump back into work.
A simple first-evening routine helps:
- Take medication as directed: Don't wait until discomfort builds.
- Use a cold compress: This helps limit swelling in the early window.
- Sleep with your head propped up: Many patients find this reduces throbbing.
- Keep food soft and low effort: Yoghurt, soup that's not hot, smoothies eaten carefully, and mashed foods are usually easier.
What changes by day 1 to day 3
Most discomfort and swelling peak early and then settle. In Australia, dental implant recovery timing by region reports that peak pain and swelling usually resolve by days 3 to 5, analgesic use averages 2.5 days, and 90% of patients resume work by day 2. The same source notes that Biolase laser technology can reduce the initial recovery period by 20 to 30% through reduced tissue trauma.
That matches what patients usually report in a practical sense. Day 1 may feel puffy and a bit awkward. By day 2 or 3, patients often feel more in control and less worried.
Practical rule: If symptoms are gradually easing, you're usually on the right track. Recovery doesn't need to feel perfect. It needs to keep moving in the right direction.
What's normal and what isn't
A lot of avoidable anxiety comes from misreading normal symptoms.
A short guide helps:
| Usually normal | Worth calling about promptly |
|---|---|
| Mild bleeding or oozing early on | Bleeding that seems persistent or heavy |
| Swelling that peaks then starts to ease | Swelling that keeps worsening |
| Tenderness when chewing near the area | Pain that feels stronger each day |
| Bruising or jaw stiffness | A sense that the implant area is moving |
What helps, and what tends not to
The first 72 hours reward restraint. Patients who recover comfortably usually follow simple rules well.
- Helpful: Rest, soft foods, medication taken on time, gentle hydration, and avoiding pressure on the site.
- Not helpful: Crunchy foods, smoking, hard rinsing, excessive gym work, alcohol if you've been advised to avoid it, and repeated touching of the area with the tongue or fingers.
- Very helpful for anxious patients: Sedation can make the procedure itself feel much less stressful, and lower stress often makes the immediate recovery easier to manage.
If you've ever had an extraction and want a sense of pain relief guidance, our article on Panadeine Forte for tooth extraction covers the kind of post-operative comfort questions patients often ask in those first few days.
Navigating Diet Hygiene and Activity in the First Weeks
Once the first few days pass, patients often make one of two mistakes. They either stay overly cautious and become anxious about every mouth sensation, or they feel so much better that they forget healing is still underway.
The first couple of weeks are about returning to routine carefully, not all at once.

Eating without disturbing the site
Soft food doesn't have to mean poor nutrition. In fact, this period is a good time to prioritise hydration, protein, and foods that are easy to chew without driving pressure into the surgical area.
Good early choices often include:
- Smooth meals: Soup, blended vegetables, dal, and soft casseroles.
- Protein that doesn't fight back: Eggs, fish, yoghurt, tofu, and very soft shredded meats if comfortable.
- Easy breakfast options: Porridge, soft fruit, smoothies, or soaked cereals.
- Low-effort snacks: Cottage cheese, avocado, hummus, and mashed vegetables.
What usually causes trouble is texture, not flavour.
- Avoid hard foods: Nuts, crusty bread, chips, and raw crunchy vegetables can overload the site.
- Avoid sticky foods: Caramel and chewy lollies can tug at healing tissue.
- Be careful with very hot foods: Heat can be irritating when the area is still fresh.
If you're trying to build meals around gentler ingredients, an AI Meal Planner anti-inflammatory plan can be a useful starting point for soft, easy-to-tolerate meal ideas during recovery.
Oral hygiene without overdoing it
A clean surgical site heals better, but “clean” doesn't mean aggressive. Most problems in the first fortnight come from one of two extremes. Patients either avoid the area entirely, or they brush it too confidently too soon.
The aim is controlled hygiene.
You don't need to attack the area to keep it healthy. Gentle, consistent cleaning is safer than occasional over-cleaning.
A sensible approach usually looks like this:
- Brush the rest of the mouth normally. Don't let one surgical area cause neglect everywhere else.
- Clean near the implant site carefully. Follow the specific instructions you've been given about when and how to brush around the area.
- Don't force tools into the site. Toothpicks, vigorous flossing, and forceful rinsing can set you back.
- Keep follow-up appointments. Healing tissue often looks better to a clinician than it does to an anxious patient in the bathroom mirror.
For another recovery guide built around protecting a healing site, our post on wisdom teeth removal recovery tips covers many of the same practical habits that help oral tissues settle well.
Returning to work, exercise, and normal life
This stage often feels deceptively easy. Many people feel minimal pain by the end of the first week, but that doesn't mean the implant is ready for full chewing pressure. According to this article on normal recovery time for dental implants, most patients feel minimal pain by days 5 to 7, yet that symptomatic improvement can hide the longer biological healing still in progress.
That mismatch is where trouble starts. Patients feel normal, so they chew steak on the implant side, return to heavy lifting, or clench through exercise sessions.
A safer way to think about activity is:
- Work: Many people can return relatively early if discomfort is controlled and the job isn't physically demanding.
- Walking and light movement: Usually easier to resume before strenuous training.
- Gym sessions: Better restarted progressively, especially if you tend to brace your jaw or hold your breath under effort.
- Chewing: Return to harder foods only when you've been advised the site is ready.
A short visual guide can help if you're more comfortable learning this way.
Understanding Osseointegration The 3 to 6 Month Healing Phase
The longest part of dental implants recovery time happens where you can't see it. This is osseointegration, the stage where the implant and the surrounding bone form a stable union.
The easiest analogy is a house foundation. You can build the visible parts later, but if the base isn't secure, everything above it is at risk.
What is happening inside the jaw
After placement, the body begins adapting around the titanium implant. Early bone activity starts around the implant first. Over time, that contact becomes stronger and more mature, creating the support needed for the final restoration.
This phase doesn't usually announce itself with dramatic symptoms. In many patients, that is exactly why it gets underestimated. If the area feels settled, it's tempting to assume the implant is already “finished”.
That assumption is risky.
Why patience matters more than comfort
According to this PubMed-listed implant recovery summary, 95% of dental implant patients in Australia achieve full functional recovery within 3 to 4 months, soft tissue closure occurs by week 2, and osseointegration for enhanced implants is confirmed via ISQ measurements at an average of 3.2 months. The same source states that laser-assisted implants show 97.6% success rates with healing 1.5x faster than untreated cases.
Those figures are useful because they explain something patients often struggle with. The gums can look settled quite early, while the deeper recovery continues much longer. The visible healing and the structural healing are not the same thing.

The quiet months are often the most important months. When nothing seems to be happening, the implant is either gaining stability or losing it, depending on how well the site is protected.
What patients should do during this phase
This period isn't passive. You still have a job to do.
- Keep the bite protected: Don't test the implant with hard chewing.
- Maintain excellent home care: Plaque around healing tissue is avoidable.
- Attend review visits: Healing needs to be checked, not guessed.
- Report changes early: Pressure, mobility, or unusual soreness should never be ignored.
If you'd like a more detailed explanation of the implant fixture itself and how it sits in bone, our article on the endosseous dental implant gives that background in plain language.
How Your Health and Procedure Affect Healing Time
No dentist should pretend every implant case heals on the exact same clock. The broad timeline is useful, but your own recovery depends on the condition of your bone, your medical background, your habits, and the complexity of the procedure.
A straightforward single implant in healthy bone usually behaves differently from a case involving grafting, full-arch treatment, or systemic health issues.
Single implant compared with more complex treatment
For many patients, a single implant is the simplest path. The surgery is usually more limited, the site is easier to protect, and aftercare is more straightforward.
Complexity rises when one or more of these factors are present:
| Situation | Likely effect on recovery |
|---|---|
| Bone grafting | Healing can take longer before the site is ready for the final stage |
| Full-arch treatment | Function may return in a different pattern, but the case still needs careful protection |
| Upper jaw sites with poorer bone quality | Integration may be slower than in denser lower jaw bone |
| Medical risk factors | Healing may be less predictable and need closer monitoring |
Earlier in the article, the key biological timing was covered. What changes here is not the principle, but how much support your body needs to reach that endpoint safely.
Smoking, diabetes, and slower healing
Some patients heal efficiently and predictably. Others need a more cautious approach because their tissue response is slower or less strong.
Smoking and diabetes are two of the best-known examples. They don't automatically rule implants out, but they can make healing more fragile. That means fewer shortcuts, tighter aftercare, and stronger emphasis on keeping the site clean and protected.
If healing is likely to be slower, the answer isn't wishful thinking. It's better planning, lower tissue trauma, and stricter follow-through.
Where laser-assisted treatment can change the picture
For patients with risk factors, minimally invasive treatment matters. According to this overview of dental implant recovery and care FAQs, Biolase laser dentistry can reduce healing time by up to 50%, and University of Sydney 2025 data cited there reports 40% faster soft tissue healing in laser-assisted cases compared with traditional methods. The same source presents this as particularly helpful for patients affected by smoking or diabetes, with full integration potentially shortened to 2 to 4 months.
Because that source includes 2025 material, it's best read as a cited projection and emerging practice trend rather than a universal promise for every case. In real clinical life, laser technology is helpful, but it doesn't remove the need for good habits. A patient who smokes heavily, misses reviews, or chews too aggressively can still compromise an otherwise well-placed implant.
What actually works
Patients often ask for the one thing that speeds healing up. There usually isn't one. There is a combination.
What works best is:
- Selecting the right case timing: Implants do better when the site is prepared properly.
- Reducing surgical trauma where possible: Less disruption can make the early healing phase calmer.
- Controlling risk factors: Smoking reduction, stable medical management, and good oral hygiene matter.
- Following restrictions longer than feels necessary: This is one of the hardest parts, and one of the most valuable.
What doesn't work is trying to “push through” recovery because the area no longer hurts.
Your Recovery Partnership with The Smile Spot
A successful implant isn't just placed well. It is also monitored well. Recovery goes more smoothly when patients know what follow-up is for, what warning signs matter, and when to call.
Review appointments aren't formalities. They help confirm that the gum is settling, the implant remains stable, and your bite, hygiene, and healing pattern are all moving in the right direction.
What follow-up appointments are checking
At each stage, the focus changes.
Early reviews often look at:
- Soft tissue healing: Is the gum closing and calming as expected?
- Comfort and swelling: Are symptoms easing in the right pattern?
- Cleaning access: Can you keep the area clean without damaging it?
Later reviews become more about stability and readiness for the next restorative step. If an X-ray or clinical assessment is needed before progressing, that check protects the long-term result.
When you should call sooner
Patients sometimes wait too long because they don't want to “bother” the clinic. That's the wrong instinct after implant surgery. It's better to ask early than to sit on a problem.
Call promptly if you notice:
- Pain that worsens instead of easing
- Swelling that keeps increasing
- Persistent bleeding that doesn't seem to settle
- A bad taste, discharge, or signs that worry you
- Any feeling that the implant area is moving
- A bite that suddenly feels very wrong
Most post-operative concerns turn out to be manageable. The important thing is timing. Small issues are easier to deal with when they're raised early.
What makes the process feel easier for patients
Patients usually cope best when the practical side is organised from the start. That means knowing how to contact the clinic, understanding the fee discussion before treatment begins, and having appointment times that fit around ordinary life.
For busy Inner West patients, these details make a real difference:
- Clear communication: Written and verbal instructions reduce uncertainty.
- Sedation availability: Helpful for anxious patients who put off treatment because of fear.
- Experience with advanced cases: Important when the treatment is more complex than a routine single implant.
- Late evening and Saturday access: Easier follow-up means fewer missed checks.
- Transparent planning: Patients recover more calmly when there are no surprises around the treatment pathway.
The best recovery experiences usually don't feel dramatic. They feel organised, well-supported, and predictable.
If you're weighing up implants and want honest guidance about your likely recovery, The Smile Spot can help you understand the timeline, the trade-offs, and the treatment options that suit your case. Whether you need a single implant or a full-arch solution, the right plan starts with a careful consultation, clear answers, and a recovery pathway built around safe healing.