If you're reading this, there's a good chance food has become something you manage rather than enjoy. Maybe you're chewing on one side, avoiding photos, worrying about a loose bridge, or feeling that one broken tooth has turned into a whole-mouth problem.
That kind of dental fatigue is real. People often arrive at this point after years of patch repairs, emergency fixes, and trying to “put up with it” for a bit longer. What started as a few worn teeth, a missing molar, or an old crown can slowly affect your bite, your comfort, your confidence, and even how relaxed you feel in social situations.
Full mouth rehab is the point where dentistry stops being about isolated fixes and starts becoming a joined-up plan. It isn't just about making teeth look better. It's about rebuilding stability, function, comfort, and appearance together so your mouth works properly again.
Rebuilding Your Smile Your Confidence Your Life
A failing smile rarely fails all at once. More often, it happens in layers. A cracked tooth gets crowned. Another tooth starts wearing down. A bridge becomes harder to clean. You clench at night. Your jaw feels tight in the morning. Over time, you stop trusting your own bite.

That's why full mouth rehab can feel so different from routine dental treatment. It addresses the whole system at once. Teeth, gums, bite position, muscle comfort, appearance, and long-term durability all need to work together. If one part is ignored, the result often doesn't last.
Many patients feel anxious when they first hear the term. It sounds big, expensive, and clinical. In practice, it means something much more reassuring. It means your dentist is no longer guessing from tooth to tooth. There is a clear plan, a sequence, and a reason for each decision.
Why a complete plan matters
A mouth with multiple problems usually can't be repaired successfully with isolated treatment alone. If the bite is unstable, beautiful crowns can chip. If gum health is poor, implants may be delayed. If grinding isn't managed, even excellent ceramic work can be overloaded.
Full mouth rehab works best when health, function, and aesthetics are planned together rather than in competition with each other.
This is also why patients often describe the outcome as life-changing. They don't just notice straighter teeth or whiter ceramics. They notice they can chew with confidence, speak more naturally, and stop thinking about their mouth all day.
If you'd like to see what this kind of transformation can look like in real patients, the before and after smile gallery gives a helpful sense of what's possible when treatment is planned thoroughly.
What Full Mouth Rehab Really Means
Think of full mouth rehab as renovating a house with structural problems. If the foundation is shifting, repainting one room won't solve much. It may look better briefly, but the cracks return because the core issue was never addressed.
Dentistry works the same way. A single crown, veneer, or implant can be excellent treatment when the rest of the mouth is healthy and stable. But when several things are going wrong at once, the smarter move is to create a master plan before any final work begins.
It's not one treatment
Full mouth rehab is a customised combination of treatments, chosen according to what your mouth needs. For one patient, that may mean gum therapy, crowns, and bite correction. For another, it may involve implants, veneers, provisional restorations, and protective night guards.
What matters is the sequence. Stabilise disease first. Rebuild function next. Refine appearance after the bite is dependable.
That order prevents many of the problems I see in patchwork dentistry.
Patching problems versus rebuilding stability
Short-term fixes usually fail for predictable reasons:
- The bite is ignored. A tooth may be restored beautifully, but if it hits too hard, it won't stay comfortable.
- Old work is treated in isolation. Replacing one crown without considering adjacent wear can create a new imbalance.
- Cosmetics are rushed. A nice-looking smile that doesn't function well often becomes a maintenance headache.
- Underlying causes stay active. Grinding, acid wear, gum disease, and missing support teeth keep damaging new work.
By contrast, a well-planned rehab looks at how every tooth meets, how the jaw closes, how the gums support the restorations, and what materials suit the job. That's why full mouth rehab is usually a long-term investment rather than a quick cosmetic upgrade.
Practical rule: If you've had multiple dental issues recurring in different parts of the mouth, it's usually time to stop thinking tooth-by-tooth and start thinking system-by-system.
Patients who've already had several crowns or bridges often find it useful to understand how larger restorations behave over time. This overview of dental crowns and bridges is a good place to start if some of your current work is wearing out.
Is Full Mouth Rehabilitation Right for You
Some people know immediately that they need more than a filling or a single crown. Others sense something isn't right but can't quite define it. They just know their teeth don't feel reliable anymore.

You may be a strong candidate for full mouth rehab if several of these apply at the same time:
- Missing teeth that have changed how you chew or caused neighbouring teeth to drift
- Failing dental work such as old crowns, bridges, or large fillings that keep breaking down
- Severe tooth wear from grinding, clenching, or acid erosion
- Jaw discomfort or bite instability that leaves your teeth feeling uneven
- Multiple cosmetic concerns that can't be solved properly with one isolated treatment
You are not alone in needing major rebuilding
Extensive dental treatment is far more common than many people realise. In the United States, an estimated 40 million adults have lost all their natural teeth, according to this summary of full mouth restoration statistics. That doesn't mean every patient needs the same solution, but it does show how many people eventually need extensive rehabilitation rather than minor repair.
For older adults, this matters even more because many have been told, directly or indirectly, that they're “too old” for advanced treatment. That isn't a sound way to assess candidacy.
Age doesn't rule you out
The same statistics summary notes that implant success rates exceed 90% even in patients over 70, and All-on-4 systems report survival rates above 94% after 10 years. Age alone isn't the deciding factor. Bone support, medical history, oral health, and the quality of planning matter far more.
That's why some of the best full mouth rehab candidates are patients in their sixties, seventies, and beyond who want to eat properly again, smile without hesitation, and stop managing failing teeth one problem at a time.
A short explanation can also help if you're exploring whether implants might be part of your plan:
Signs I'd take seriously in a consultation
When I assess a possible rehab case, I'm less interested in one dramatic symptom and more interested in patterns. These are the combinations that usually point to a full-mouth issue:
Repeated breakage
If restorations keep chipping, loosening, or cracking, the bite may be overloading them.Shrinking chewing comfort
Patients often start avoiding crusty bread, steak, nuts, or apples long before they say they have “serious dental problems”.A smile that feels older than you are
Worn front teeth can flatten the smile and collapse facial support.Daily self-consciousness
If you're thinking about your teeth every day, that matters clinically as well as emotionally.
Your Potential Treatment Options Explained
A full mouth rehab plan is built from a set of treatment tools. The right combination depends on what is damaged, what is missing, what can be saved, and how your bite needs to function when everything is finished.
One patient may need implants and bridges. Another may keep most natural teeth and restore them with crowns or veneers. The key is choosing treatments for the job they're meant to do, not forcing one solution onto every problem.
The main options and when they help
| Treatment | Best For | Key Benefit |
|---|---|---|
| Crowns | Heavily damaged or worn teeth that can still be saved | Rebuilds strength and shape |
| Bridges | Replacing a missing tooth where support teeth are suitable | Restores function without a removable appliance |
| Dental implants | Replacing one or more missing teeth with independent support | Helps restore chewing confidence and preserves a fixed solution |
| All-on-4 | Extensive tooth loss or failing dentition across an arch | Replaces a full arch with a fixed implant-supported restoration |
| Veneers | Front teeth with shape, colour, or surface concerns | Improves smile aesthetics with conservative preparation in selected cases |
| Night guards | Bruxism and post-rehab protection | Protects restorations from grinding overload |
A more detailed look at All-on-4 dental implants in Sydney is useful if you're deciding between replacing a few teeth and rebuilding an entire arch.
Why material choice matters
Material selection isn't cosmetic trivia. It affects strength, fit, wear characteristics, and how natural the final result looks. According to this overview of the planning and process of full mouth rehabilitation, final restorations often use E.max with 530 MPa strength or Zirkonzahn zirconia for veneers, which allows attractive results with minimal tooth preparation.
In practical terms, that means different materials suit different roles:
- E.max works well when aesthetics and conservative preparation matter.
- Zirkonzahn zirconia is a strong option where precision, durability, and refined appearance are both important.
- Zirconia-based prostheses are often favoured in larger rehabilitations where long-term resilience matters.
Where Biolase laser dentistry fits
Biolase laser technology is useful when soft tissue management needs to be more precise and less invasive. That can help with gum contouring, managing inflamed tissue, and improving comfort around certain procedures. It's not a gimmick. It's one of the tools that can make treatment cleaner and recovery easier in the right case.
A good rehab plan doesn't chase technology for its own sake. It uses the right tool only when that tool improves precision, comfort, or healing.
Some patients also have jaw discrepancies that aren't primarily dental. If your bite problem stems from skeletal alignment rather than worn or missing teeth alone, information about surgery for jaw realignment can help you understand where dentistry ends and jaw surgery may need to be considered as part of a broader plan.
Your Rehab Journey Step By Step at The Smile Spot
Most anxious patients calm down once the process is broken into clear stages. Full mouth rehab feels overwhelming when it's imagined as one giant procedure. It feels manageable when you understand what happens first, what waits until later, and why.
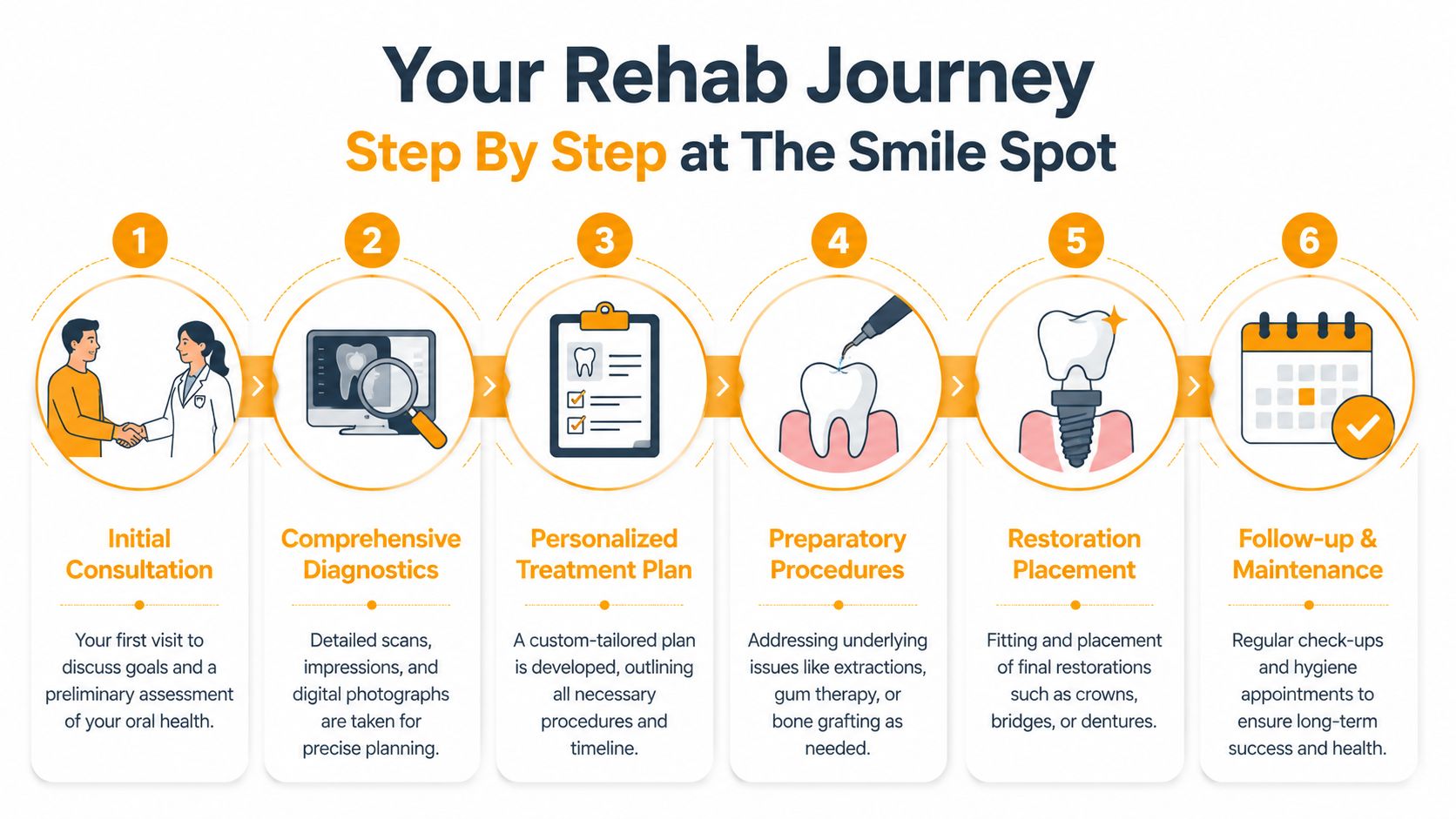
Step one and step two
The first appointment is about listening before planning. We look at your symptoms, concerns, past dental history, and what you want your mouth to do better. Some patients want to chew without pain. Some want to stop breaking teeth. Some want a smile that looks like them again.
After that comes thorough diagnostics. That usually includes photographs, radiographs, bite analysis, and 3D imaging when implant or complex restorative planning is involved. At this stage, hidden problems often become clearly visible.
Step three and step four
Once the records are complete, the treatment plan is built in sequence. If gum inflammation, infection, hopeless teeth, or unstable bite contacts are present, those issues are addressed before final restorations are made. This stage may involve provisional work so the bite can be tested before anything definitive is locked in.
Then comes active treatment. Depending on the case, that might include extractions, implant placement, crowns, bridges, veneers, soft tissue refinement, or full-arch provisional restorations. For patients who are nervous, oral sedation dentistry can make longer visits much more manageable.
The best rehab cases are rarely rushed. We test, adjust, and confirm comfort before finalising the details that need to last.
Step five and step six
The delivery of final restorations is a major milestone, but it isn't the end of treatment. Once the new bite is in place, small refinements are often needed as the muscles adapt and the patient starts chewing, speaking, and smiling normally again.
Long-term maintenance then becomes part of the plan, not an afterthought. That includes review appointments, hygiene care, monitoring of implants or restorations, and protective strategies if you grind or clench.
A typical rehab journey often follows this pattern:
Consultation and discussion
Understand the problem fully, including your goals.Records and diagnostics
Build the case on evidence, not assumptions.Planning and smile design
Decide what to save, replace, rebuild, or improve.Foundation treatment
Stabilise disease, remove failure points, and prepare the mouth.Restoration phase
Fit the restorations that rebuild function and appearance.Maintenance phase
Protect the result and keep it stable over time.
Recovery Outcomes and Lifelong Success
Most patients are surprised that recovery is less dramatic than they feared. The experience depends on which procedures are involved, but modern planning, careful sequencing, and minimally invasive techniques can make the process much easier than people expect.
The bigger issue isn't whether you'll have a few recovery days here and there. It's whether the end result is stable enough to justify the effort. That's where long-term evidence matters.
What long-term success looks like
A five-year retrospective study of 150 full-mouth fixed dental prosthesis cases reported an overall survival rate of 92%, with survival rates consistently exceeding 90% over five years. The same study also found that zirconia-based prostheses performed better than traditional metal-ceramic alternatives. Those findings are discussed in this clinical review of full-mouth fixed dental prostheses.
That's encouraging, but it doesn't mean maintenance can be casual. In the same five-year period, 15% of patients experienced technical complications and 12% experienced biological complications. Good work can last very well, but it still needs review, hygiene, and timely adjustment when something small starts to drift.
What protects the result
Long-term success usually comes down to habits and monitoring more than glamour. The restorations may be advanced, but the principles are straightforward.
- Keep review appointments so minor wear or bite changes are caught early.
- Clean around restorations carefully because biological problems often begin subtly.
- Wear a custom guard if you grind rather than assuming strong ceramics are indestructible.
- Report changes early if something feels high, loose, sore, or different.
New teeth should feel dependable, not precious. The way we achieve that is by combining durable treatment with disciplined follow-up.
Bruxism and relapse risk
Bruxism is a real concern in worn-dentition cases. An Australian Dental Journal study discussed in this article on TMD prevalence and related wear patterns notes that bruxism affects up to 30% of adults. That matters because grinding doesn't politely stop once beautiful new restorations are placed.
Custom mouthguards become part of the rehab itself, not an optional extra. If a patient has a history of clenching, cracked teeth, or heavy wear facets, protecting the new bite is part of responsible treatment.
Understanding Costs Financing and Comfort
Cost is one of the biggest reasons people delay full mouth rehab. I understand that hesitation. These cases are significant, and patients want to know whether they're committing to something realistic, not just ideal on paper.
According to this overview of full mouth reconstruction costs, a complete full mouth rehab in Australia typically ranges from $30,000 to $60,000 AUD, and up to 25% of people in NSW delay necessary treatment due to cost concerns. That lines up with what many patients say in the chair. They're not avoiding treatment because they don't care. They're trying to work out how to make it possible.
What affects the fee
No two rehab plans cost the same because no two mouths start in the same condition. The major variables usually include:
- How many teeth can be saved versus replaced
- Whether implants are needed
- The type of final restorations used
- How much stabilisation is required first, such as gum treatment or removal of failing work
- Whether treatment is staged over time or completed more intensively
A staged approach is often the most practical answer. The first phase focuses on health, pain, infection control, and stabilisation. Later phases rebuild the bite and appearance in a structured way.
Comfort matters just as much
Many patients asking about cost are also asking something else underneath it. They want to know whether they can cope physically and emotionally with treatment.
That concern deserves a direct answer. Full mouth rehab should be planned around comfort as well as outcomes. For some patients, that means shorter visits. For others, it means sedation support, carefully paced appointments, or provisional stages that let them adjust gradually instead of all at once.
If you're comparing ways to spread treatment costs more manageably, this article on dentists with payment plans near me may help you think through what staged financing can look like in practice.
Practical questions to ask before saying yes
Before committing to treatment, ask these questions plainly:
What must be done first, and what can wait?
This separates urgent care from ideal long-term planning.Which parts of the treatment are fixed versus flexible?
Not every choice has the same impact on longevity.What support is available if I'm anxious?
Comfort planning should be part of the quote discussion.How will maintenance costs look after treatment?
Good dentistry includes a plan for protecting the investment.
Frequently Asked Questions About Full Mouth Rehab
Patients usually ask better questions once they understand the basics. That's a good sign. It means the fear is starting to give way to practical decision-making.

How long does full mouth rehab take
It depends on what your mouth needs. A case built mostly around crowns and bite rehabilitation may move quite differently from a case involving extractions, implants, and healing periods. The most honest answer is that the timeline should be customised after full diagnostics, not guessed at during a quick phone call.
Is full mouth rehab painful
Most patients report that the anticipation is worse than the treatment. Discomfort varies by procedure, but careful planning, local anaesthetic, gentle technique, and sedation where appropriate make a major difference. The goal is to keep you comfortable during treatment and predictable afterwards, not to “push through” difficult appointments.
Can I fix only the front teeth if that's what bothers me most
Sometimes, yes. Often, no. If the front teeth are damaged because the bite is unstable or the back teeth no longer support properly, treating the front alone usually doesn't last. That's why many cosmetic complaints turn out to be functional cases in disguise.
Am I too old for implants or full mouth rehab
Age by itself usually isn't the deciding issue. General health, bone support, gum condition, medications, and treatment goals matter more. Many older adults are excellent candidates once those factors are assessed properly.
Will my new teeth look natural
They should. A successful rehab doesn't produce a generic smile. It rebuilds tooth shape, bite position, facial support, and colour in a way that suits your features and personality. The best result is one that looks healthy, balanced, and believable.
What if I grind my teeth
That has to be planned for from the beginning. If you grind or clench, your dentist should factor that into material choice, bite design, and long-term protection. In many cases, a custom night guard is part of the final plan.
Can private health insurance help
It may help with parts of treatment, depending on your level of cover and the procedures involved. The only reliable way to know is to have the treatment mapped out clearly and itemised properly. Broad assumptions are where confusion usually starts.
What's the first step if I'm interested but overwhelmed
Start with diagnosis, not commitment. You don't need to decide on every treatment option immediately. You need a clear understanding of what's going on in your mouth, what is urgent, what is optional, and what sequence gives you the best long-term result.
If you're tired of living around broken, worn, or failing teeth, the next step is a proper plan. The Smile Spot helps Dulwich Hill and Inner West patients understand their options clearly, move at a comfortable pace, and rebuild function and confidence with modern, carefully sequenced care.